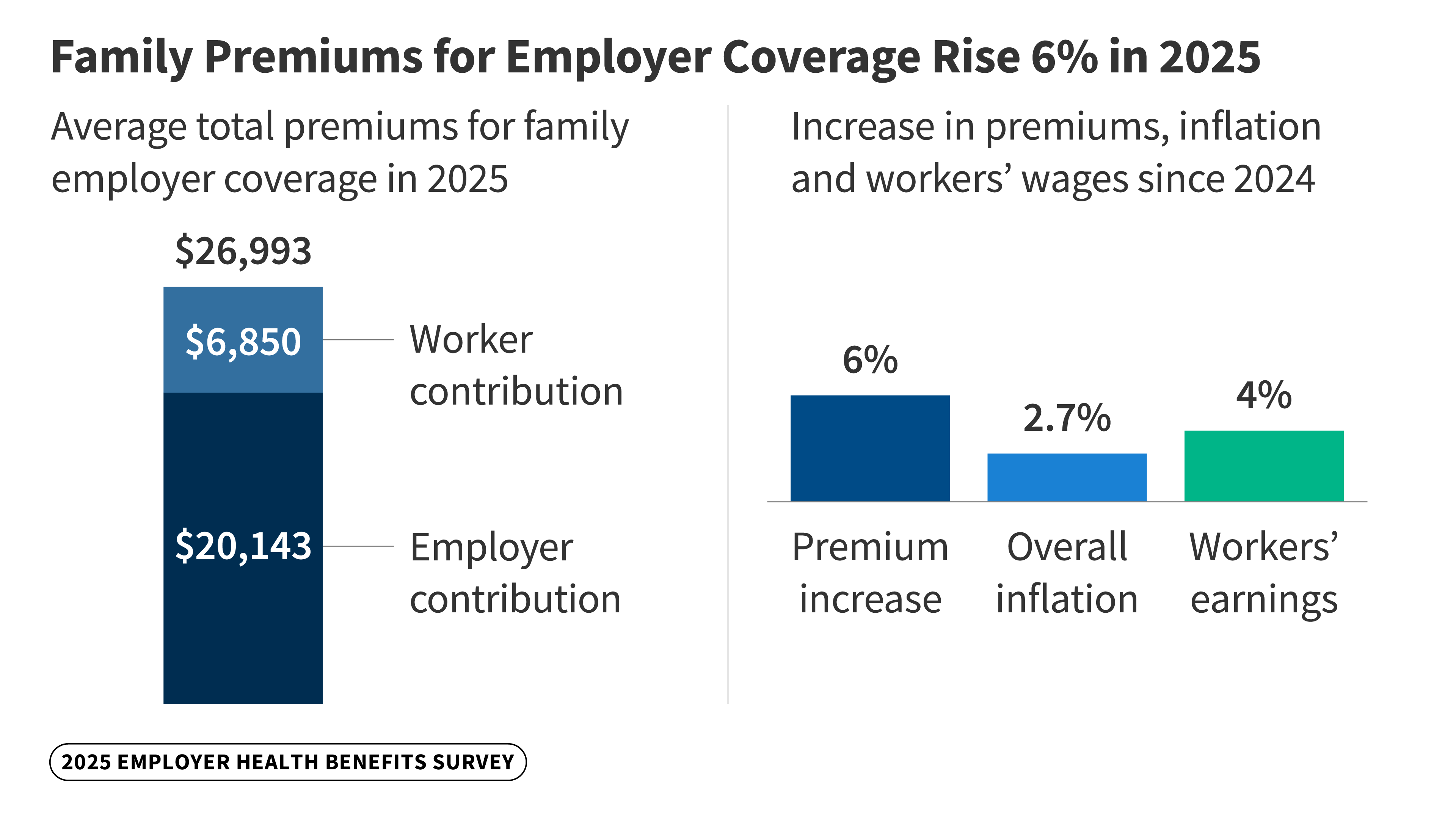Employer Health Coverage Costs Rise, GLP-1 Drug Access a Growing Concern
Washington D.C. – A newly released analysis reveals a continuing upward trend in employer-sponsored health coverage costs, coupled with increasing scrutiny over how companies will navigate the emerging landscape of glucagon-like peptide-1 (GLP-1) medications used for weight loss. The report highlights significant shifts in premium contributions, cost-sharing arrangements, and the overall affordability of healthcare for American workers.
The Evolving Landscape of Employer-Sponsored Health Plans
For decades, employer-sponsored health insurance has been the cornerstone of healthcare access for millions of Americans. However, the system faces persistent challenges, including escalating costs and complex administrative burdens. This latest data underscores these difficulties, showing that premiums continue to outpace wage growth, placing a greater financial strain on both employers and employees.
The report details how employers are responding to these pressures. Many are adjusting cost-sharing provisions – such as deductibles, copayments, and coinsurance – to shift more of the financial responsibility to workers. This trend, while helping employers manage costs, can create barriers to care for employees, particularly those with chronic conditions or limited financial resources.
Offer rates, the percentage of employers offering health coverage, remain relatively stable, but the types of plans offered are evolving. High-deductible health plans (HDHPs) paired with health savings accounts (HSAs) are becoming increasingly popular, offering potential tax advantages but also requiring employees to shoulder a larger upfront financial burden.
The GLP-1 Medication Dilemma
A significant focus of this year’s analysis is the growing demand for GLP-1 drugs, initially developed for managing type 2 diabetes but now widely used for weight loss. These medications, including drugs like Ozempic and Wegovy, have demonstrated remarkable efficacy in promoting weight reduction, but their high cost and potential for off-label use are raising concerns among employers.
Many employers are grappling with whether to cover these drugs, and if so, under what conditions. Some are implementing prior authorization requirements, limiting coverage to individuals with diabetes, or excluding coverage altogether. The potential for widespread use of GLP-1s, even among individuals who don’t meet clinical criteria, could significantly impact healthcare spending.
What impact will the increasing demand for these medications have on overall healthcare costs? Will employers be able to effectively manage utilization and ensure appropriate prescribing practices? These are critical questions facing the healthcare industry today.
Beyond cost, employers are also considering the ethical implications of covering weight loss drugs. Some worry about perpetuating societal pressures around body image and potentially stigmatizing individuals who choose not to use these medications.
To gain further insight into the complexities of healthcare benefits, consider exploring resources from the Kaiser Family Foundation, a leading non-profit organization dedicated to healthcare policy research.
Understanding the nuances of health insurance is crucial for both employers and employees. For a broader perspective on healthcare trends, the America’s Health Insurance Plans (AHIP) website provides valuable information and advocacy resources.
Frequently Asked Questions About Employer Health Coverage
-
What is driving the increase in employer health coverage costs?
Several factors contribute to rising costs, including advancements in medical technology, increasing prescription drug prices, and the aging of the population. Administrative costs and hospital consolidation also play a role.
-
Are high-deductible health plans (HDHPs) a good option for employees?
HDHPs can be beneficial for employees who are generally healthy and don’t anticipate frequent medical expenses. However, they require employees to pay more out-of-pocket before coverage kicks in, which can be a challenge for those with chronic conditions.
-
How are employers addressing the cost of GLP-1 drugs?
Employers are employing various strategies, including prior authorization, limiting coverage to individuals with diabetes, and implementing utilization management programs to ensure appropriate prescribing.
-
What is the potential impact of GLP-1 drugs on the healthcare system?
Widespread adoption of GLP-1 drugs could significantly increase healthcare spending, potentially leading to higher premiums and cost-sharing for all. It could also strain the supply chain and create access issues.
-
Will employers cover GLP-1 drugs for weight loss even if they aren’t prescribed for diabetes?
Coverage decisions vary widely among employers. Some are choosing to cover these drugs for weight loss, while others are excluding coverage due to cost and ethical concerns.
The future of employer-sponsored health coverage remains uncertain. Navigating these challenges will require collaboration between employers, insurers, policymakers, and healthcare providers to ensure affordable and accessible care for all Americans.
What steps can employers take to mitigate rising healthcare costs while still providing comprehensive benefits to their employees? How can we ensure equitable access to innovative medications like GLP-1 drugs?
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.