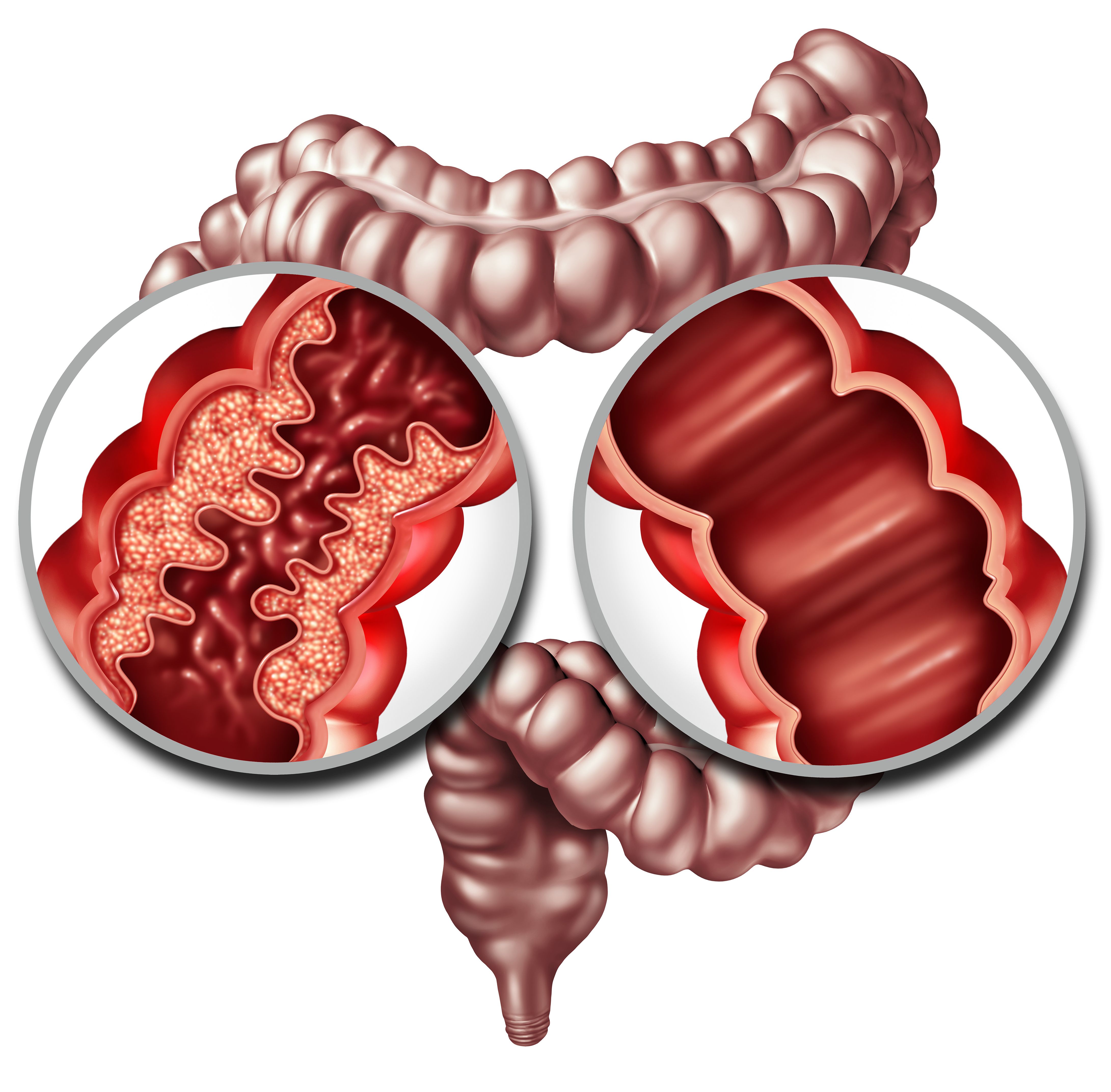
Crohn’s Disease Treatment: A Paradigm Shift Towards Early, Aggressive Intervention
Nearly 1.6 million Americans live with inflammatory bowel disease (IBD), and Crohn’s disease accounts for a significant portion of these cases. But the landscape of Crohn’s treatment is rapidly evolving. Recent updates to the American Gastroenterological Association (AGA) clinical practice guidelines signal a decisive move towards utilizing advanced therapies – biologics and small molecule inhibitors – earlier in the disease course, rather than reserving them for later stages of treatment failure. This isn’t simply a tweak to existing protocols; it represents a fundamental shift in how we approach Crohn’s, and it foreshadows a future of increasingly personalized and proactive IBD management.
The New Guidelines: A Focus on Proactive Control
Traditionally, Crohn’s disease treatment followed a “step-up” approach, starting with less potent medications like aminosalicylates and immunomodulators, escalating to biologics only when these proved ineffective. The AGA’s updated guidelines, however, advocate for a “treat-to-target” strategy. This means aiming for endoscopic remission – the visible healing of the intestinal lining – and utilizing advanced therapies, including anti-TNF agents, anti-integrins, and JAK inhibitors, as first-line options for moderate to severe Crohn’s disease.
This change is driven by a growing body of evidence demonstrating that early intervention with these powerful drugs can not only improve symptoms but also alter the disease course, preventing complications like strictures, fistulas, and the need for surgery. The guidelines emphasize the importance of shared decision-making between clinicians and patients, carefully weighing the benefits and risks of each treatment option.
Beyond Biologics: The Rise of Small Molecule Inhibitors
While biologics have been the mainstay of advanced Crohn’s treatment for years, a new class of drugs – small molecule inhibitors – is gaining prominence. Specifically, JAK inhibitors like upadacitinib are showing remarkable efficacy in inducing and maintaining remission, offering an oral alternative to injectable biologics. The AGA guidelines acknowledge this progress, incorporating JAK inhibitors as viable first-line options, particularly for patients who may not respond well to anti-TNF therapy.
The Future of Crohn’s Treatment: Personalization and Predictive Modeling
The shift towards early, aggressive treatment is just the beginning. The future of Crohn’s disease management will be defined by two key trends: personalized medicine and predictive modeling. Advances in genomics, metabolomics, and the microbiome are providing unprecedented insights into the underlying causes of IBD and the factors that influence disease progression.
Imagine a future where a simple blood test can identify a patient’s specific Crohn’s “endotype” – a distinct molecular profile that predicts their response to different therapies. This would allow clinicians to tailor treatment plans from the outset, maximizing efficacy and minimizing side effects. Furthermore, machine learning algorithms are being developed to analyze patient data – including genetic information, clinical history, and microbiome composition – to predict disease flares and proactively adjust treatment accordingly.
The integration of digital health technologies, such as wearable sensors and mobile apps, will also play a crucial role. These tools can continuously monitor patients’ symptoms, medication adherence, and lifestyle factors, providing real-time data that can inform treatment decisions.
The development of novel therapeutic targets is also on the horizon. Researchers are exploring new approaches to modulate the immune system, restore gut barrier function, and address the dysbiosis that characterizes IBD. These include therapies targeting specific cytokines, signaling pathways, and microbial metabolites.
Implications for Healthcare Systems and Patients
This evolving treatment landscape has significant implications for healthcare systems. The higher cost of advanced therapies necessitates innovative reimbursement models and value-based care arrangements. Furthermore, increased access to specialized IBD care is crucial to ensure that patients receive timely and appropriate treatment.
For patients, the AGA guidelines offer a message of hope. Early and aggressive intervention can significantly improve their quality of life and prevent long-term complications. However, it also underscores the importance of active participation in their care, engaging in shared decision-making with their clinicians, and adhering to their treatment plans.
Frequently Asked Questions About Crohn’s Disease Treatment
What is “treat-to-target” therapy in Crohn’s disease?
“Treat-to-target” therapy means actively aiming for endoscopic remission – visible healing of the intestinal lining – and adjusting treatment until that goal is achieved, rather than simply managing symptoms.
Are small molecule inhibitors a good alternative to biologics?
Small molecule inhibitors, like JAK inhibitors, offer an oral alternative to injectable biologics and have shown promising efficacy in treating Crohn’s disease, particularly for patients who don’t respond well to anti-TNF therapy.
How will personalized medicine impact Crohn’s disease treatment?
Personalized medicine aims to tailor treatment plans based on a patient’s unique genetic makeup, microbiome composition, and other individual factors, maximizing efficacy and minimizing side effects.
What role does the microbiome play in Crohn’s disease?
The gut microbiome is increasingly recognized as a key player in IBD. Imbalances in the microbiome can contribute to inflammation and disease progression, and therapies aimed at restoring microbial balance are being actively investigated.
The future of Crohn’s disease treatment is bright, driven by scientific innovation and a commitment to personalized, proactive care. As we continue to unravel the complexities of this disease, we can expect even more effective and targeted therapies to emerge, offering hope for a better quality of life for millions of people living with Crohn’s.
What are your predictions for the future of Crohn’s disease management? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.