The delicate balance between rapid diagnostic speed and clinician safety in neurointensive care is shifting. For years, the medical community has grappled with a critical trade-off: the necessity of bedside imaging for unstable patients versus the cumulative radiation risks faced by the staff operating the machinery. New data suggests that this tension may soon be a thing of the past.
- Dramatic Risk Reduction: Integrated shielding in mobile head CT systems can slash occupational radiation exposure by 91% to 99%.
- PPE Evolution: Effective hardware shielding may significantly reduce the reliance on bulky personal protective equipment (PPE), streamlining emergency workflows.
- Precision Safety: Real-world dosimetry shows that clinicians and nurses can maintain exposure levels well below detectable limits when following optimized positioning protocols.
The Deep Dive: Why Bedside Imaging is a High-Stakes Game
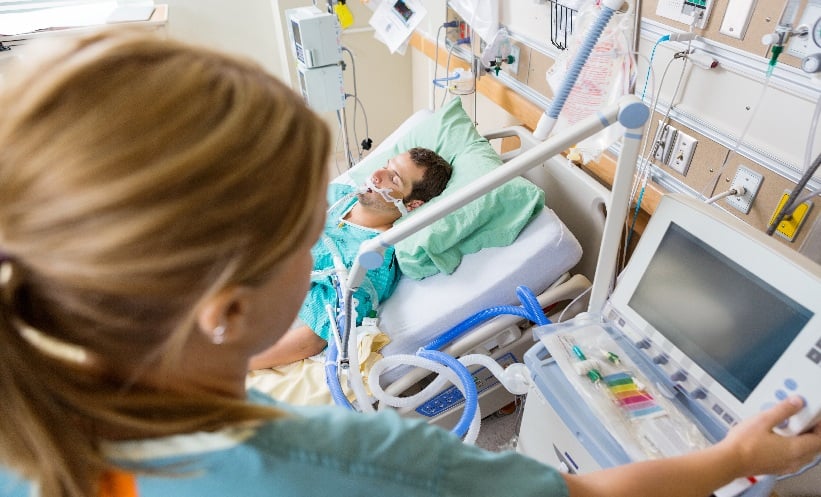
In a Neurointensive Care Unit (NICU), time is brain. Transporting a critically ill patient—often hemodynamically unstable or requiring complex life-support—to a radiology department is a high-risk maneuver that can lead to adverse events during transit. Mobile head CTs solve this by bringing the scanner to the patient.
However, the “cost” of this convenience has traditionally been scatter radiation. Unlike fixed CT suites, which are housed in lead-lined rooms, mobile units operate in open environments. This has forced staff to rely on heavy lead aprons and strict distance protocols, which can be cumbersome in the chaotic, high-pressure environment of an ICU. The system evaluated in the recent study by Hillergren P et al. addresses this by integrating the shielding directly into the hardware—utilizing a 0.5 mm lead curtain at the front and a 1 mm detachable shield at the rear.
The results are striking: mean effective doses for radiology nurses (0.07 µSv) and clinicians (0.03 µSv) remained negligible. This suggests that the “shielding-at-the-source” approach is far more effective than relying solely on individual PPE.
The Forward Look: What Happens Next?
This shift toward integrated shielding signals a broader trend in medical technology: the movement from passive protection (wearing lead) to active engineering (shielding the source). As these systems become standardized, we can expect several industry shifts:
First, workflow optimization will become the primary safety metric. Since the study noted that staff behind the console benefited most, hospitals will likely implement standardized “safety zones” within the NICU, treating the mobile CT’s footprint as a temporary radiation-controlled area.
Second, we may see a regulatory shift in PPE requirements. If integrated shielding consistently proves to keep exposure below detectable limits, healthcare institutions may reduce the mandatory use of heavy lead aprons for certain bedside procedures. This would not only reduce physical strain on nurses—who often suffer from musculoskeletal issues due to heavy PPE—but also decrease the time spent “gearing up” during critical emergencies.
While the study was limited to a single center over three months, the evidence provides a blueprint for the next generation of bedside diagnostics: equipment that protects the provider as effectively as it diagnoses the patient.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.