India is currently navigating a complex epidemiological transition. While the country is achieving landmark successes in curbing certain cancers, it is simultaneously seeing a surge in others—a trend that reflects the collision of ingrained cultural habits and the rapid adoption of “Westernized” lifestyles.
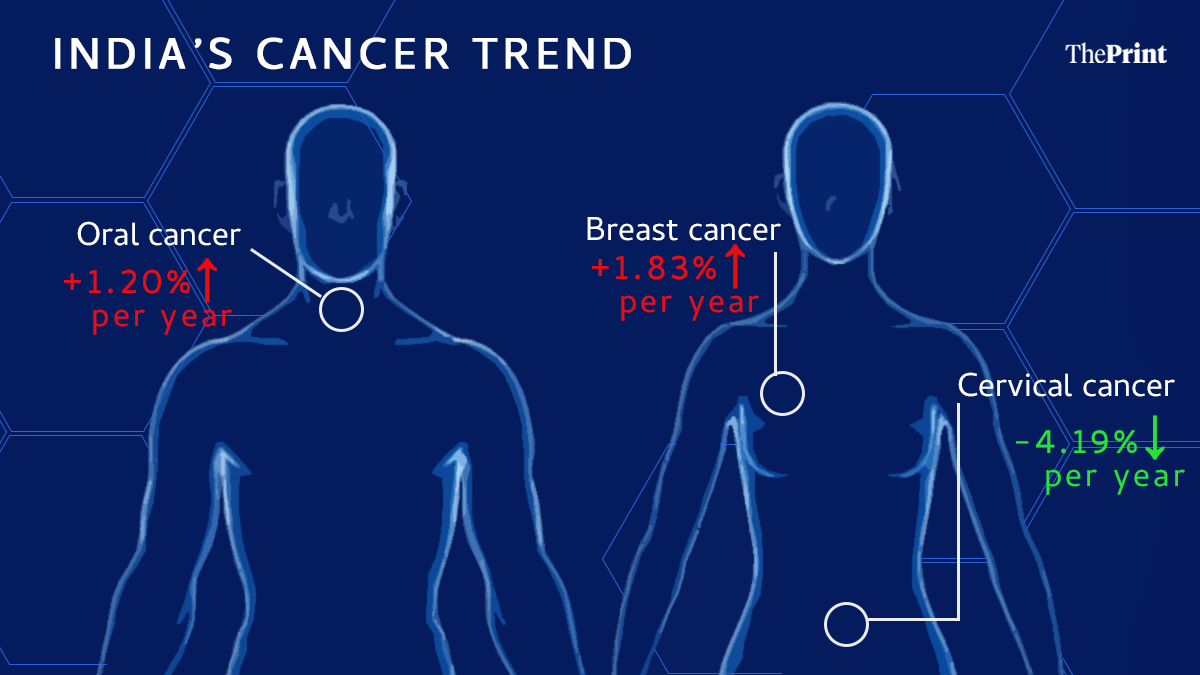
- The Divergence: Breast cancer (up 1.83% annually) and male oral cancer (up 1.20% annually) are rising steadily, while cervical cancer is seeing a sharp decline of 4.19% per year.
- The Lifestyle Catalyst: The rise in breast cancer is linked to reproductive shifts (delayed childbearing) and metabolic changes (obesity, alcohol), mirroring trends in other developing economies.
- The Tobacco Trap: Unlike wealthy G20 nations where cancer risks decline across generations, India’s oral cancer risk remains persistently high due to the continued prevalence of smokeless tobacco and betel quid.
A new analysis by the Indian Council of Medical Research (ICMR), published in the Journal of Public Health, reveals a stark contrast between India and high-income G20 nations. In most wealthy countries, breast and oral cancer rates are plateauing or falling. India, however, is moving in the opposite direction, suggesting that the socioeconomic drivers of cancer are shifting as the nation develops.
The Deep Dive: A Tale of Two Trends
To understand these numbers, one must look at the Age-Period-Cohort analysis used by the ICMR. This method is critical because it filters out the “noise” of an aging population. The data confirms that the rise in breast and oral cancers isn’t simply because people are living longer; the actual risk for younger generations is increasing or remaining stubbornly high.
The Oral Cancer Stagnation: Oral cancer remains India’s most distinct public health challenge. The study highlights a gender-based acceleration: while rates for men and women are similar until age 40, male incidence spikes sharply thereafter. This is a direct result of persistent exposure to smokeless tobacco and betel nut—habits that have not declined across successive generations, unlike in high-SDI (Socio-Demographic Index) countries.
The “Westernization” of Breast Cancer: The increase in breast cancer cases is a symptom of a broader societal shift. The ICMR identifies a “lifestyle transition”—characterized by obesity, alcohol consumption, and reproductive changes such as earlier menstruation and shorter breastfeeding durations. This mirrors a pattern seen in other emerging economies, including China and Turkey, where rapid urbanization often brings health trade-offs.
The Cervical Success Story: The most encouraging data point is the 4.19% annual decline in cervical cancer. This success is attributed to improved hygiene, better reproductive health awareness, and the groundwork laid for HPV prevention. It serves as a proof-of-concept: targeted public health interventions can effectively bend the curve of cancer incidence.
The Forward Look: What Happens Next?
As India scales its healthcare infrastructure, the focus must shift from mere treatment to aggressive, stratified prevention. Here is what to watch in the coming years:
1. The “Detection Gap” vs. Mortality: A critical void in the current data is the lack of mortality figures for India. As screening improves—such as the move toward affordable ultrasound in rural areas and mammography in cities—we may see “incidence” continue to rise simply because we are finding more cases earlier. The real metric of success in the next five years will be whether mortality rates drop despite rising incidence.
2. The HPV Vaccination Pivot: With the Union government launching a nationwide HPV vaccination program for 14-year-old girls, India is attempting to replicate its cervical cancer success on a massive scale. If successfully implemented, this could make cervical cancer a rarity in future generations, shifting the clinical burden entirely toward lifestyle-driven cancers.
3. The Policy War on Smokeless Tobacco: Since oral cancer risk is “persistently high” across cohorts, current tobacco control measures are clearly insufficient. Expect to see calls for more stringent regulations on betel quid and smokeless tobacco, as these are no longer just “bad habits” but systemic drivers of a national health crisis.
Ultimately, India’s cancer profile is a mirror of its development. The challenge for policymakers is to ensure that economic progress does not come at the cost of a permanent increase in non-communicable diseases.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.