Declining Vaccination Rates in Seniors Raise Public Health Concerns
A concerning trend is emerging in the United States: vaccination rates among individuals aged 65 and older have been steadily decreasing since 2019. This decline poses a significant personal health risk to aging Americans and their families, while simultaneously escalating into a critical public health challenge for the nation. Recent data released on January 21, 2026, by the Centers for Disease Control and Prevention’s National Center for Health Statistics (Data Brief 547) underscores the severity of this issue.
The timing of this report coincides with the launch of The Value of Vaccines, a crucial conversation series spearheaded by Pfizer. I was honored to contribute to this important project alongside esteemed colleagues Elif Alyanak from Avalere, Venesa Day with Fox Chubby Health Policy Consulting, and Kim Thiboldeaux of the Northeast Business Group on Health. The series was expertly moderated by Dr. Geeta Nayyar, author of Dead Wrong: Diagnosing and Treating Healthcare’s Misinformation Illness.
The Growing Gap in Adult Immunization
The CDC’s data paints a clear picture: protecting the health of the population requires consistent and widespread vaccination. The decline in influenza and pneumococcal vaccination rates among older adults is particularly alarming. As individuals age, their immune systems naturally weaken, making them more susceptible to severe illness from preventable diseases. This vulnerability is often compounded by underlying health conditions like heart disease and chronic obstructive pulmonary disease (COPD).
The most dramatic drop in flu vaccination rates among older Americans occurred between 2023 and 2024, signaling a potentially dangerous shift in preventative healthcare practices. What factors are contributing to this decline, and how can we reverse this trend?
Disparities in Vaccination Access and Uptake
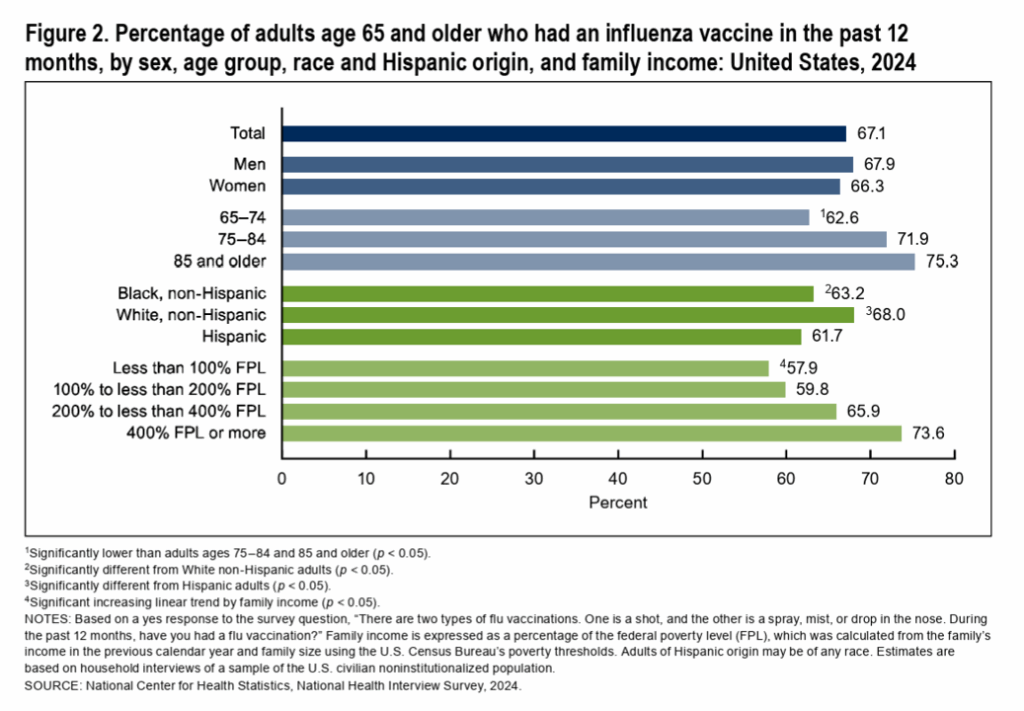
A closer examination of the CDC data reveals disparities in influenza vaccination rates based on age, race, and socioeconomic status. Older adults (75.3%) generally exhibit higher rates of flu vaccination compared to younger seniors (62.6%). Furthermore, individuals with higher household incomes are more likely to receive the flu vaccine than those with limited financial resources. This highlights the critical role of socioeconomic factors in accessing preventative healthcare.

These findings underscore the need for targeted interventions to address barriers to vaccination among vulnerable populations. Could improved outreach programs and increased access to affordable vaccines help bridge these gaps?
The conversations within the Value of Vaccines series provided valuable insights into the complex landscape of adult vaccination. We explored how stakeholders across the healthcare ecosystem – from providers and policymakers to community organizations and individuals – can collaborate to promote vaccine confidence and improve vaccination rates.
Further research from the Kaiser Family Foundation highlights ongoing challenges in equitable vaccine distribution and access, particularly among underserved communities.
The World Health Organization also emphasizes the importance of global vaccine equity to protect populations worldwide.
Frequently Asked Questions About Adult Vaccinations
-
What vaccinations are recommended for seniors?
Seniors are typically recommended to receive annual influenza vaccines, pneumococcal vaccines, shingles vaccines, and tetanus-diphtheria-pertussis (Tdap) boosters. Consult with your healthcare provider for personalized recommendations.
-
Why is it important for seniors to get vaccinated?
As people age, their immune systems weaken, making them more vulnerable to severe complications from vaccine-preventable diseases. Vaccination helps protect seniors from illness, hospitalization, and even death.
-
Are vaccines safe for older adults?
Vaccines undergo rigorous testing and are generally considered safe for older adults. However, it’s essential to discuss any concerns with your healthcare provider.
-
What can be done to improve vaccination rates among seniors?
Strategies to improve vaccination rates include increasing access to vaccines, addressing vaccine hesitancy, and providing culturally sensitive education about the benefits of vaccination.
-
How does income affect access to vaccinations?
Individuals with lower incomes may face barriers to vaccination due to cost, lack of insurance, or limited access to healthcare facilities. Programs that provide free or low-cost vaccines can help address these disparities.
Tune into the four episodes of the Value of Vaccines podcast series for a deeper dive into these critical issues.
Share this article to help raise awareness about the importance of adult vaccinations and encourage a national conversation about protecting the health of our aging population.
Disclaimer: This article provides general information and should not be considered medical advice. Please consult with a qualified healthcare professional for personalized guidance on vaccinations.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.

