Native American Health Crisis: Stark Disparities Demand Urgent Action
A new examination of public health data reveals a deeply concerning reality: Native American individuals in the United States face significantly diminished health outcomes compared to their White counterparts. The gap in life expectancy, coupled with disproportionately high rates of chronic illness and mental health challenges, underscores a systemic crisis demanding immediate and sustained attention.
The Scope of the Disparity
Data consistently demonstrates a stark difference in life expectancy. While the average American can expect to live approximately 78.4 years, Native American individuals, identifying as AIAN alone, have a life expectancy of just 70.1 years. This nearly decade-long gap isn’t attributable to a single factor, but rather a complex interplay of socioeconomic determinants, historical trauma, and systemic barriers to healthcare access.
Beyond longevity, the prevalence of chronic diseases paints a troubling picture. Native Americans experience higher rates of diabetes, heart disease, and liver disease than the national average. These conditions are often exacerbated by limited access to nutritious food, safe environments for physical activity, and culturally competent healthcare providers. The Centers for Disease Control and Prevention offers comprehensive information on diabetes prevention and management.
Mental Health and Substance Use
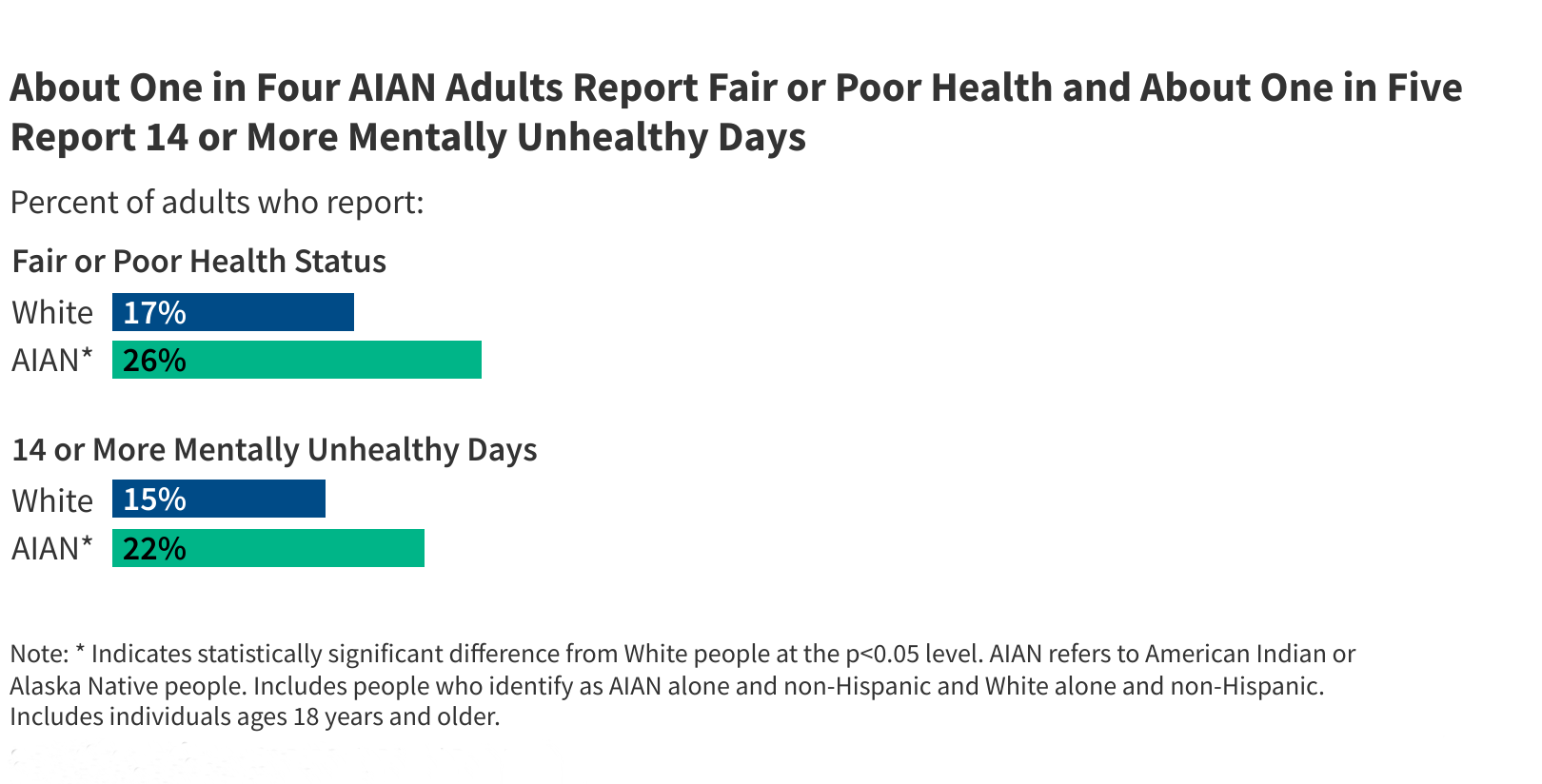
The mental health crisis within Native American communities is particularly acute. Suicide rates are significantly higher among AIAN individuals, especially young people. This is often linked to historical trauma, poverty, discrimination, and a lack of culturally appropriate mental health services. Substance use disorder also presents a major challenge, frequently co-occurring with mental health conditions and contributing to increased morbidity and mortality.
What role does historical trauma play in the current health crisis facing Native American communities? And how can we ensure that healthcare systems are truly responsive to the unique needs of these populations?
Access to quality healthcare remains a significant obstacle. Many Native Americans live in remote areas with limited healthcare facilities, and even when facilities are available, they may lack the resources to provide comprehensive care. Furthermore, cultural barriers and historical mistrust of the healthcare system can deter individuals from seeking treatment. The Indian Health Service (IHS) is the primary federal health care provider and health advocate for Indian people, but faces chronic underfunding.
Addressing these disparities requires a multifaceted approach. This includes increased funding for the IHS, expansion of healthcare access in rural areas, culturally competent training for healthcare providers, and community-based prevention programs. It also necessitates addressing the underlying social and economic factors that contribute to poor health outcomes, such as poverty, discrimination, and lack of educational opportunities. The National Institute on Minority Health and Health Disparities conducts and supports research on health disparities.
Frequently Asked Questions About Native American Health Disparities
-
What are the primary drivers of health disparities among Native American populations?
The primary drivers include historical trauma, socioeconomic factors like poverty and lack of education, limited access to healthcare, and systemic discrimination.
-
How does the Indian Health Service (IHS) address these health challenges?
The IHS provides direct healthcare services to eligible Native Americans and Alaska Natives, but it is chronically underfunded and faces significant challenges in meeting the healthcare needs of these populations.
-
What is meant by “historical trauma” in the context of Native American health?
Historical trauma refers to the cumulative emotional and psychological wounding across generations resulting from massive group trauma, such as colonization, forced removal, and cultural suppression.
-
What can be done to improve mental health outcomes in Native American communities?
Improving mental health outcomes requires culturally appropriate mental health services, addressing the root causes of trauma, and promoting community-based healing initiatives.
-
Are there specific chronic diseases that disproportionately affect Native American individuals?
Yes, Native Americans experience higher rates of diabetes, heart disease, liver disease, and certain types of cancer compared to the national average.
The health of Native American communities is a moral imperative. By acknowledging the systemic factors that contribute to these disparities and investing in culturally responsive solutions, we can work towards a future where all individuals have the opportunity to live long and healthy lives.
What further steps can be taken to ensure equitable healthcare access for Native American communities? And how can we foster greater understanding and empathy towards the unique challenges they face?
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.