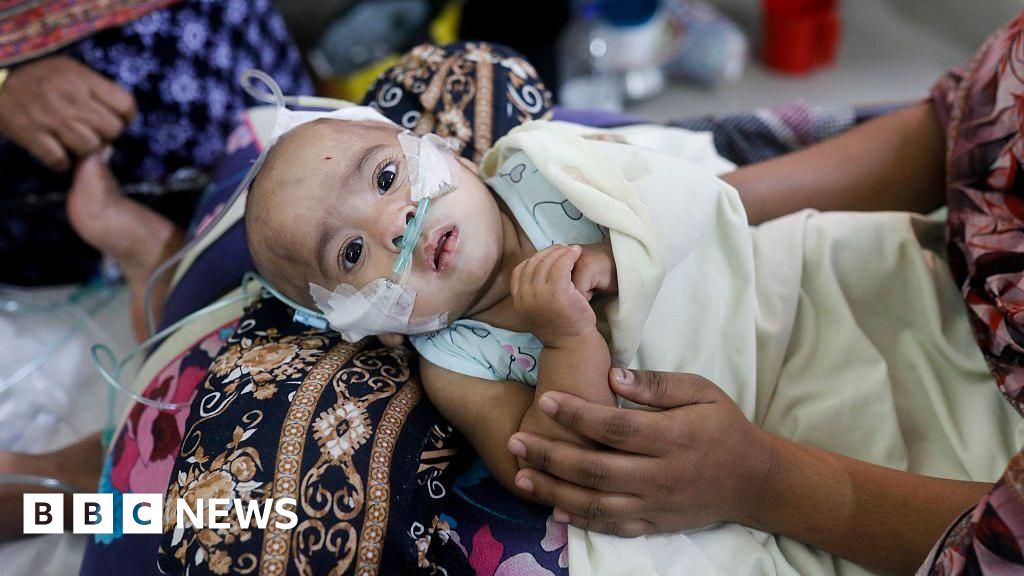
Bangladesh Measles Crisis: A Harbinger of Global Vaccine Hesitancy and Future Outbreaks
Nearly 100 children have died in Bangladesh in just three weeks due to a resurgent measles outbreak, a tragedy that isn’t simply a localized health crisis. This alarming spike, coupled with similar outbreaks globally, isn’t a random occurrence; it’s a stark warning about the fragility of global immunization infrastructure and the escalating threat of vaccine hesitancy in a world increasingly shaped by climate change and geopolitical instability. The situation demands a re-evaluation of pandemic preparedness and a proactive approach to safeguarding global health security.
The Perfect Storm: Why Bangladesh?
Bangladesh’s recent outbreak is rooted in a complex interplay of factors. Reports indicate a significant decline in measles vaccination rates following disruptions caused by the COVID-19 pandemic. Resources were diverted, routine immunization programs were stalled, and public trust in healthcare systems was eroded. This created a pool of susceptible children, ripe for infection. However, to view this solely as a consequence of the pandemic is a simplification. Pre-existing challenges within the healthcare system, including logistical hurdles in reaching remote populations and a persistent struggle against misinformation, exacerbated the problem.
The Hindu reports that the outbreak began in late April and quickly overwhelmed local health facilities. Al Jazeera highlights the urgent need for a coordinated response, while News18 emphasizes the potential for spillover effects into neighboring India, a nation with its own complex immunization challenges. The Deccan Herald confirms the devastating toll – 94 children lost in just 19 days – a statistic that should serve as a global wake-up call.
Beyond COVID-19: The Rise of Vaccine Hesitancy
While the pandemic undeniably disrupted immunization schedules, the underlying issue of **vaccine hesitancy** is far more insidious. Fueled by online misinformation, conspiracy theories, and a growing distrust of scientific institutions, vaccine hesitancy is no longer confined to fringe groups. It’s becoming increasingly mainstream, impacting vaccination rates across diverse demographics and geographic regions. This trend isn’t limited to measles; we’re seeing similar declines in coverage for other preventable diseases, like polio and diphtheria.
This hesitancy is often amplified by socio-economic factors. Access to reliable information, healthcare services, and even basic sanitation can significantly influence a parent’s decision to vaccinate their child. Addressing these systemic inequalities is crucial to building trust and ensuring equitable access to immunization.
Climate Change: An Unexpected Amplifier
The connection between climate change and infectious disease outbreaks is often overlooked, but it’s becoming increasingly clear. Extreme weather events – floods, droughts, and heatwaves – can displace populations, disrupt healthcare infrastructure, and create conditions conducive to the spread of infectious diseases. In Bangladesh, a country highly vulnerable to climate change, these factors are likely contributing to the severity of the measles outbreak.
Furthermore, changing climate patterns can alter the geographic distribution of disease vectors, potentially introducing measles to new areas where populations have little or no immunity. This underscores the need for climate-resilient healthcare systems and proactive surveillance programs.
The Future of Immunization: A Proactive Approach
The Bangladesh crisis is a microcosm of a larger global challenge. To prevent similar tragedies, we need a fundamental shift in our approach to immunization. This requires:
- Strengthening Surveillance Systems: Real-time monitoring of vaccination rates and disease outbreaks is essential for early detection and rapid response.
- Combating Misinformation: Investing in public health education campaigns that address vaccine hesitancy and promote scientific literacy.
- Building Climate-Resilient Healthcare: Developing healthcare infrastructure that can withstand the impacts of climate change.
- Global Collaboration: Strengthening international partnerships to ensure equitable access to vaccines and technical assistance.
- Innovative Vaccine Delivery: Exploring new technologies and strategies to improve vaccine delivery, particularly in remote and underserved areas.
The development of mRNA vaccine technology, proven during the COVID-19 pandemic, offers a promising pathway for rapid vaccine development and deployment in response to future outbreaks. However, equitable access to these technologies remains a significant hurdle.
| Metric | 2019 (Pre-Pandemic) | 2023 (Estimated) | Projected 2025 (If Trends Continue) |
|---|---|---|---|
| Global Measles Vaccination Coverage | 86% | 81% | 76% |
| Measles Cases Globally | 900,000 | 9 million | 15 million |
Frequently Asked Questions About Measles and Global Health Security
Q: What is the biggest threat posed by declining vaccination rates?
A: The biggest threat is the resurgence of preventable diseases like measles, polio, and diphtheria, leading to outbreaks, hospitalizations, and deaths, particularly among vulnerable populations. It also strains healthcare systems and undermines progress towards global health goals.
Q: How can we effectively combat vaccine misinformation?
A: Combating misinformation requires a multi-pronged approach, including fact-checking initiatives, public health education campaigns, and collaboration with social media platforms to remove false or misleading content. Building trust in healthcare professionals and scientific institutions is also crucial.
Q: What role does climate change play in the spread of infectious diseases?
A: Climate change exacerbates the spread of infectious diseases by displacing populations, disrupting healthcare infrastructure, altering disease vector distributions, and creating conditions conducive to outbreaks. Investing in climate-resilient healthcare systems is essential.
Q: Is a global pandemic of measles a realistic possibility?
A: If current trends continue, a global measles pandemic is a very real possibility. The combination of declining vaccination rates, vaccine hesitancy, and climate change creates a perfect storm for widespread outbreaks.
The tragedy unfolding in Bangladesh is a stark reminder that global health security is not guaranteed. It demands urgent action, sustained investment, and a proactive approach to safeguarding the health of future generations. Ignoring this warning will only lead to more preventable suffering and a world increasingly vulnerable to the ravages of infectious disease. What are your predictions for the future of global immunization efforts? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.