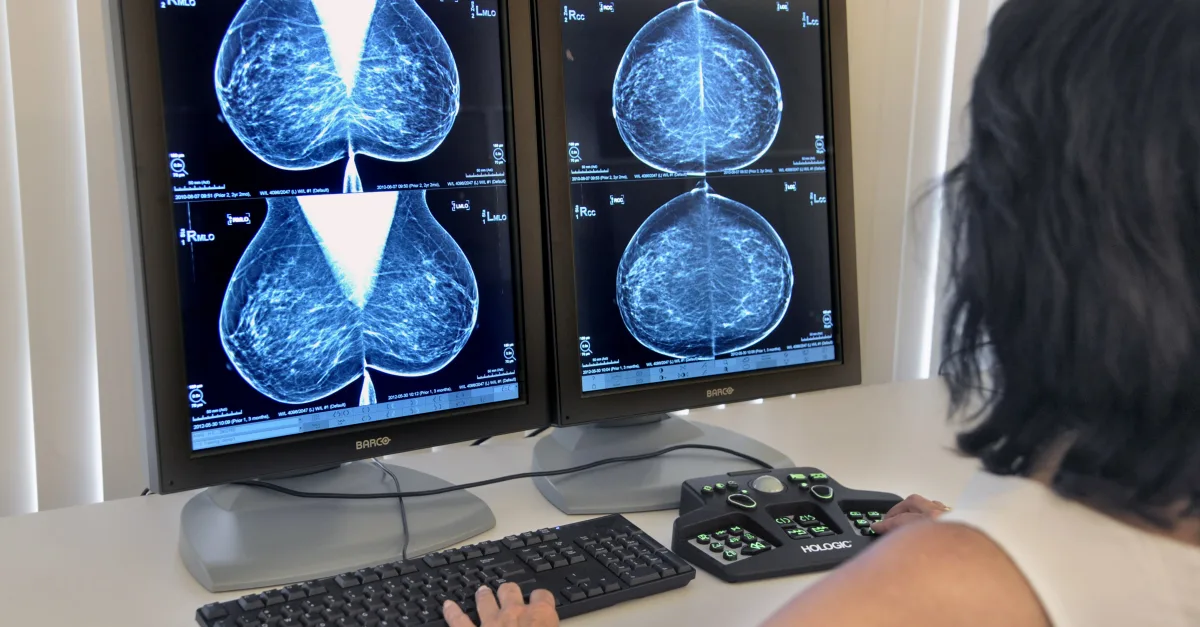
Unproven Breast Screening Methods Pose Risks to Women’s Health
A growing number of clinics are offering alternative breast cancer screening methods that lack scientific validation, raising concerns among medical professionals and patient advocacy groups. These unproven techniques, often marketed as safer or more effective than traditional mammography, can provide false reassurance or lead to delayed diagnoses, potentially endangering women’s lives. Investigations reveal a persistent market for these dubious screenings, despite repeated warnings from health authorities.
From thermography to unverified ultrasound interpretations, providers are capitalizing on anxieties surrounding breast cancer. These methods often appeal to women seeking alternatives to radiation exposure from mammograms or those who have dense breast tissue, where mammograms can be less accurate. However, experts emphasize that these alternatives have not undergone rigorous testing and are not recognized as legitimate cancer screening tools.
The Science Behind Mammography and Why Alternatives Fall Short
Mammography remains the gold standard for breast cancer screening, backed by decades of research demonstrating its ability to detect tumors at an early, treatable stage. While not perfect, mammography has significantly reduced breast cancer mortality rates. The technology has also advanced, with digital mammography and 3D mammography offering improved image quality and accuracy.
Thermography, for example, measures heat patterns in the breast, theorizing that cancerous tumors generate more heat. However, numerous studies have shown that thermography cannot reliably distinguish between cancerous and non-cancerous tissue. AD.nl reports that companies continue to market this technology despite its proven ineffectiveness, preying on women’s fears.
Similarly, some clinics offer ultrasound screenings with interpretations that go beyond standard diagnostic practices. These interpretations often lack standardization and can lead to unnecessary biopsies or, conversely, missed cancers. Heart of the Netherlands highlights the promotion of unreliable breast examinations as cancer screening.
What steps can women take to ensure they are receiving evidence-based breast cancer screening? And how can we better protect vulnerable individuals from misleading health claims?
The National Cancer Institute provides comprehensive information on recommended breast cancer screening guidelines. Additionally, consulting with a board-certified radiologist or oncologist is crucial for personalized advice.
The Financial Incentives Behind Dubious Screening
Investigations by Follow the Money reveal that many clinics offering these unproven screenings operate with a strong financial incentive. They often charge high fees for services that are not covered by insurance, capitalizing on patients’ desperation and fear.
These clinics frequently employ aggressive marketing tactics, targeting women with misleading advertisements and testimonials. They may downplay the limitations of their methods and exaggerate their potential benefits. NOT reports that providers of these dubious methods remain active, despite ongoing scrutiny.
Frequently Asked Questions About Breast Cancer Screening
-
What is the most reliable method for breast cancer screening?
Mammography is currently the most reliable method for breast cancer screening, backed by extensive research and proven to reduce mortality rates.
-
Are there risks associated with mammography?
While mammography involves low-dose radiation, the benefits of early detection generally outweigh the risks. Digital mammography and 3D mammography further minimize radiation exposure.
-
Can thermography detect breast cancer?
No, thermography has not been proven to reliably detect breast cancer and should not be used as a substitute for mammography or other evidence-based screening methods.
-
What should I do if a provider offers an unproven breast screening method?
Discuss the method with your primary care physician or a board-certified radiologist to get an unbiased assessment of its effectiveness and safety.
-
How can I protect myself from misleading health claims?
Rely on information from reputable sources, such as the National Cancer Institute and the American Cancer Society, and be wary of clinics that make exaggerated promises or pressure you into unnecessary screenings.
The persistence of these unproven screening methods underscores the need for greater public awareness and stricter regulation. Women deserve access to accurate information and evidence-based care, empowering them to make informed decisions about their health.
What role should government agencies play in regulating these alternative screening practices? And how can we foster a more critical and informed approach to healthcare choices?
Share this article to help spread awareness and protect women’s health. Join the conversation in the comments below.
Disclaimer: This article provides general information and should not be considered medical advice. Always consult with a qualified healthcare professional for personalized guidance on breast cancer screening and treatment.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.