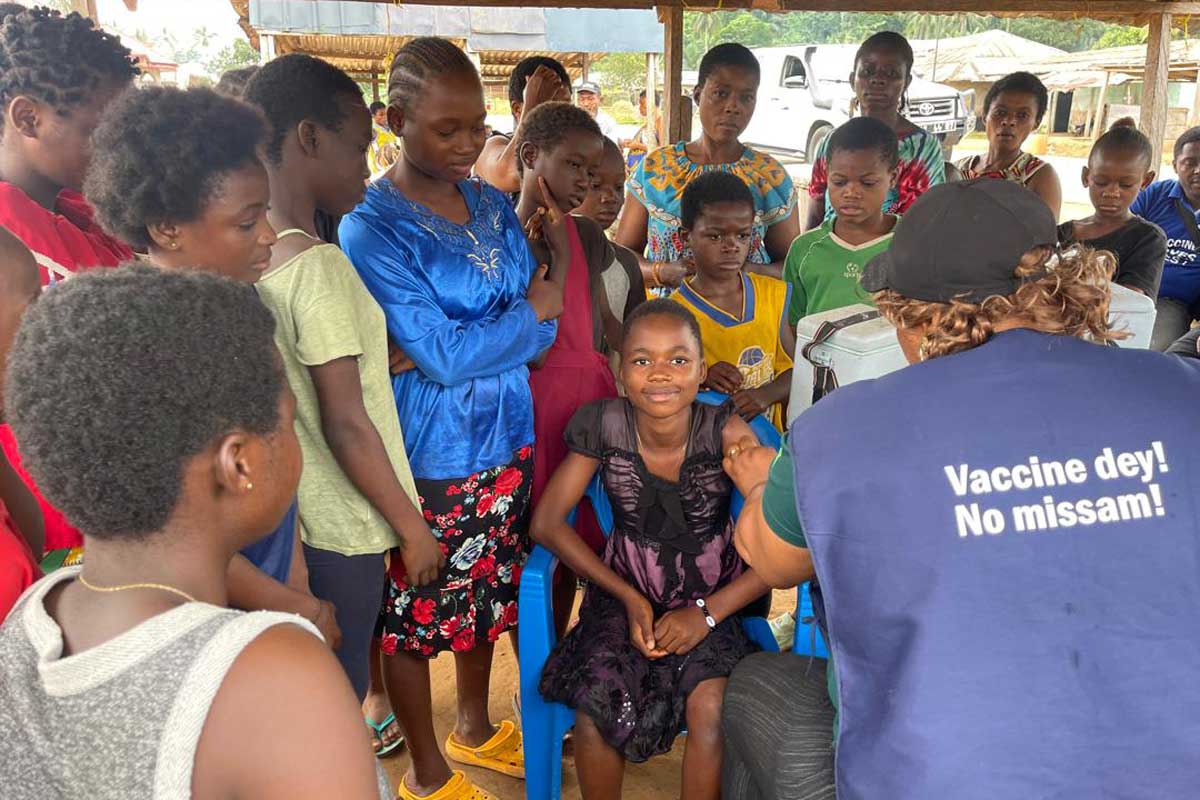
The simple act of a rain shower in Cameroon is a metaphor for a growing success story in public health: a preventable tragedy averted, one vaccination at a time. The story of Victorine, a mother in Nguti, Southwest Region, isn’t just about securing HPV vaccines for her children; it’s a powerful illustration of how personal loss, coupled with targeted outreach, can overcome deeply entrenched vaccine hesitancy and systemic barriers to healthcare access. This isn’t merely a local victory; it’s a microcosm of a larger, ongoing battle to eliminate cervical cancer globally, and a testament to the power of integrated healthcare strategies.
- Personal Tragedy Drives Action: The loss of Victorine’s sister to cervical cancer was a pivotal moment, transforming her from vaccine-hesitant to a proactive advocate for her children’s health.
- Integrated Outreach is Key: The Cameroon Baptist Convention Health Services (CBCHS) model – bundling multiple vaccines and services into a single outreach – is proving far more effective than traditional, siloed approaches.
- Gavi’s Multi-Pronged Support: Significant funding from Gavi, the Vaccine Alliance, is enabling CBCHS to expand its reach and impact in vulnerable communities.
The Weight of Preventable Loss
Cervical cancer is a devastating disease, particularly in low- and middle-income countries where access to screening and treatment is limited. Cameroon faces a particularly acute burden, with alarmingly high rates of diagnosis and mortality. The introduction of the HPV vaccine in 2020, initially for girls aged 9-14 and later extended to boys, represented a critical step forward. However, simply making the vaccine available isn’t enough. Historical distrust of medical interventions, misinformation, and logistical challenges in reaching remote communities have all contributed to vaccine hesitancy. The story highlights a crucial point: data on vaccine efficacy is insufficient without addressing the underlying social and emotional factors that influence health-seeking behaviors.
Beyond Zero-Dose: An Integrated Approach
The CBCHS program’s success lies in its holistic approach. By combining HPV vaccination with routine childhood immunizations and other essential health services, they’re not only reaching children who would otherwise fall through the cracks (“zero-dose” children) but also normalizing vaccination within the broader context of family healthcare. This integration addresses multiple needs with a single visit, reducing the burden on families and maximizing the impact of limited resources. This strategy is particularly vital in regions like Northwest and Southwest Cameroon, which are grappling with humanitarian crises and limited infrastructure. The initial resistance rooted in misinformation – falsely linking the vaccine to population control – underscores the importance of community engagement and culturally sensitive communication.
The Forward Look: Scaling Success and Addressing Equity
Victorine’s story is inspiring, but it also reveals a critical gap: access to the HPV vaccine for those outside the 9-14 age range. Her inability to afford the vaccine for her 18-year-old daughter highlights the need for expanded vaccination programs and financial assistance to ensure equitable access for all. The next phase of this initiative must focus on several key areas:
- Age Expansion: Advocacy for extending the HPV vaccination program to include older adolescents and young adults, particularly those who missed the initial rollout.
- Supply Chain Strengthening: Ensuring a consistent and reliable supply of vaccines at the local level, addressing the issue Victorine faced when the vaccine was unavailable at her primary health care unit.
- Community-Led Monitoring & Evaluation: Investing in systems that allow communities to track vaccination coverage and identify areas where outreach needs to be intensified.
- Addressing the Root Causes of Hesitancy: Continued investment in culturally appropriate health education campaigns to dispel myths and build trust in vaccines.
The CBCHS model, supported by Gavi, provides a blueprint for success. However, scaling this model requires sustained funding, strong partnerships, and a commitment to addressing the systemic inequities that prevent vulnerable populations from accessing life-saving healthcare. The promise of a better, safer future, like the sprouting crops Victorine observed, is within reach – but only through intentional, equitable action.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.