Shingles Vaccine: A Potential Shield Against Future Dementia Risk?
Nearly 6 million Americans are living with Alzheimer’s disease, a number projected to more than double by 2050. But what if a preventative measure, already widely available, could significantly reduce that risk? Emerging research suggests a surprising link between the shingles vaccine and a decreased incidence of dementia, prompting a re-evaluation of preventative healthcare strategies and opening new avenues for neurological protection.
The Unexpected Connection: Herpes Zoster and Cognitive Decline
For years, the focus on dementia prevention has centered around lifestyle factors – diet, exercise, cognitive stimulation. However, a growing body of evidence points to the role of inflammation and viral reactivation in the development of neurodegenerative diseases. The varicella-zoster virus (VZV), which causes chickenpox in childhood, remains dormant in nerve cells and can reactivate later in life as shingles (herpes zoster). Recent studies indicate that this reactivation, and the resulting inflammation, may contribute to cognitive decline and increase the risk of dementia.
How the Shingles Vaccine Offers Protection
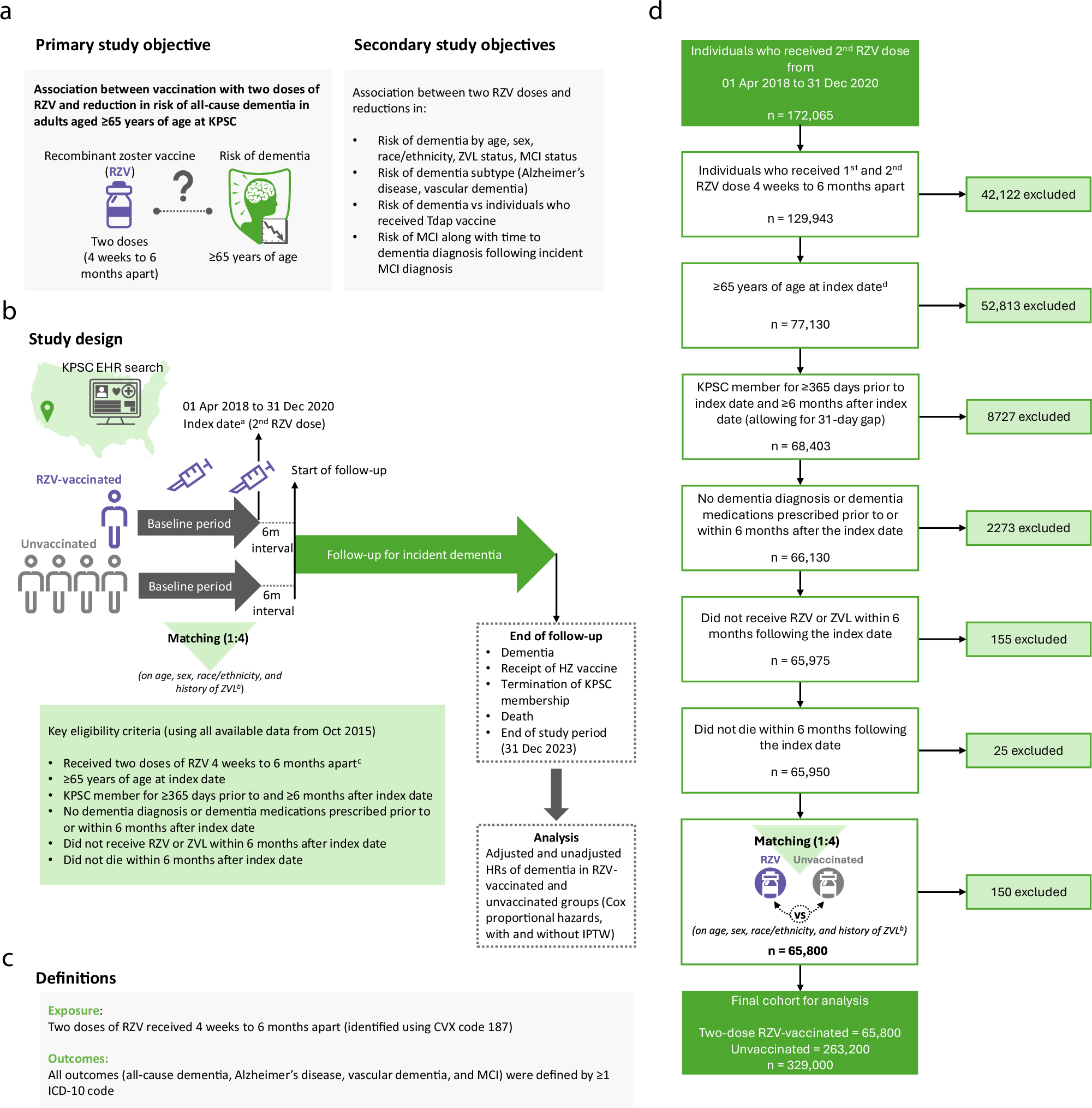
The shingles vaccine, specifically the recombinant zoster vaccine (RZV), boosts immunity to VZV, reducing the likelihood of shingles outbreaks and, crucially, minimizing the chronic inflammation associated with the virus. Several studies, including research from Germany and analyses published in Gelbe Liste, have demonstrated a correlation between shingles vaccination and a reduced risk of dementia – with some reporting a decrease of up to 20%. The mechanism isn’t fully understood, but it’s believed the vaccine’s impact on reducing neuroinflammation plays a key role.
Beyond Correlation: Unraveling the Biological Mechanisms
While the observed correlation is compelling, researchers are now focused on understanding the underlying biological mechanisms. Is it simply the reduction in shingles outbreaks that’s protective, or does the vaccine have a more direct impact on brain health? Investigations are exploring whether the vaccine modulates the immune system in a way that benefits neuronal function and resilience. Furthermore, studies are examining whether early vaccination – before the onset of VZV reactivation – offers greater protection than vaccination after a shingles episode.
The Role of Neuroinflammation in Dementia
Chronic neuroinflammation is increasingly recognized as a central driver of many forms of dementia, including Alzheimer’s disease. Inflammation damages neurons, disrupts synaptic connections, and impairs cognitive function. By controlling VZV reactivation and reducing inflammation, the shingles vaccine may be interrupting a key pathway in the development of dementia. This highlights the potential for leveraging vaccines not just against infectious diseases, but also against chronic, age-related conditions.
The Future of Vaccine-Based Dementia Prevention
The shingles vaccine findings are sparking a broader investigation into the potential of vaccines to prevent or delay dementia. Researchers are exploring the role of other viruses – such as Epstein-Barr virus and cytomegalovirus – in neurodegenerative processes. Could vaccines targeting these viruses also offer cognitive protection? The development of personalized vaccines, tailored to an individual’s viral load and immune profile, is another exciting possibility. We may be on the cusp of a new era in dementia prevention, one that harnesses the power of the immune system to safeguard brain health.
The potential for a vaccine-driven approach to dementia prevention also raises important questions about public health policy. Should shingles vaccination be universally recommended, regardless of shingles history, as a preventative measure against cognitive decline? Further research and cost-benefit analyses will be crucial in informing these decisions.
| Study | Reported Dementia Risk Reduction |
|---|---|
| Nau | Up to 20% |
| Apotheke Adhoc | Significant reduction observed |
| Gelbe Liste | Demonstrated slowed progression |
Frequently Asked Questions About Shingles Vaccine and Dementia
Will the shingles vaccine completely prevent dementia?
No, the shingles vaccine is not a guaranteed prevention for dementia. However, research suggests it may significantly reduce the risk, particularly when administered proactively. It’s best viewed as one component of a comprehensive dementia prevention strategy.
Who should consider getting the shingles vaccine?
The CDC recommends the shingles vaccine for healthy adults 50 years and older, even if they’ve had shingles before. Given the emerging evidence regarding dementia risk, discussing vaccination with your doctor is advisable, even if you are younger than 50 and have risk factors for shingles.
Are there any side effects of the shingles vaccine?
The most common side effects are mild and temporary, such as pain, redness, or swelling at the injection site. More serious side effects are rare. Your doctor can provide a complete list of potential side effects and help you determine if the vaccine is right for you.
Could other vaccines offer similar protection against dementia?
Research is ongoing to investigate the potential of vaccines targeting other viruses, such as Epstein-Barr virus and cytomegalovirus, to prevent or delay dementia. This is a rapidly evolving field, and more information will become available as studies progress.
The link between the shingles vaccine and reduced dementia risk is a compelling development, offering a glimmer of hope in the fight against this devastating disease. As research continues to unravel the complex interplay between viruses, inflammation, and brain health, we may unlock even more powerful preventative strategies for safeguarding cognitive function in the years to come. What are your predictions for the future of vaccine-based dementia prevention? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.