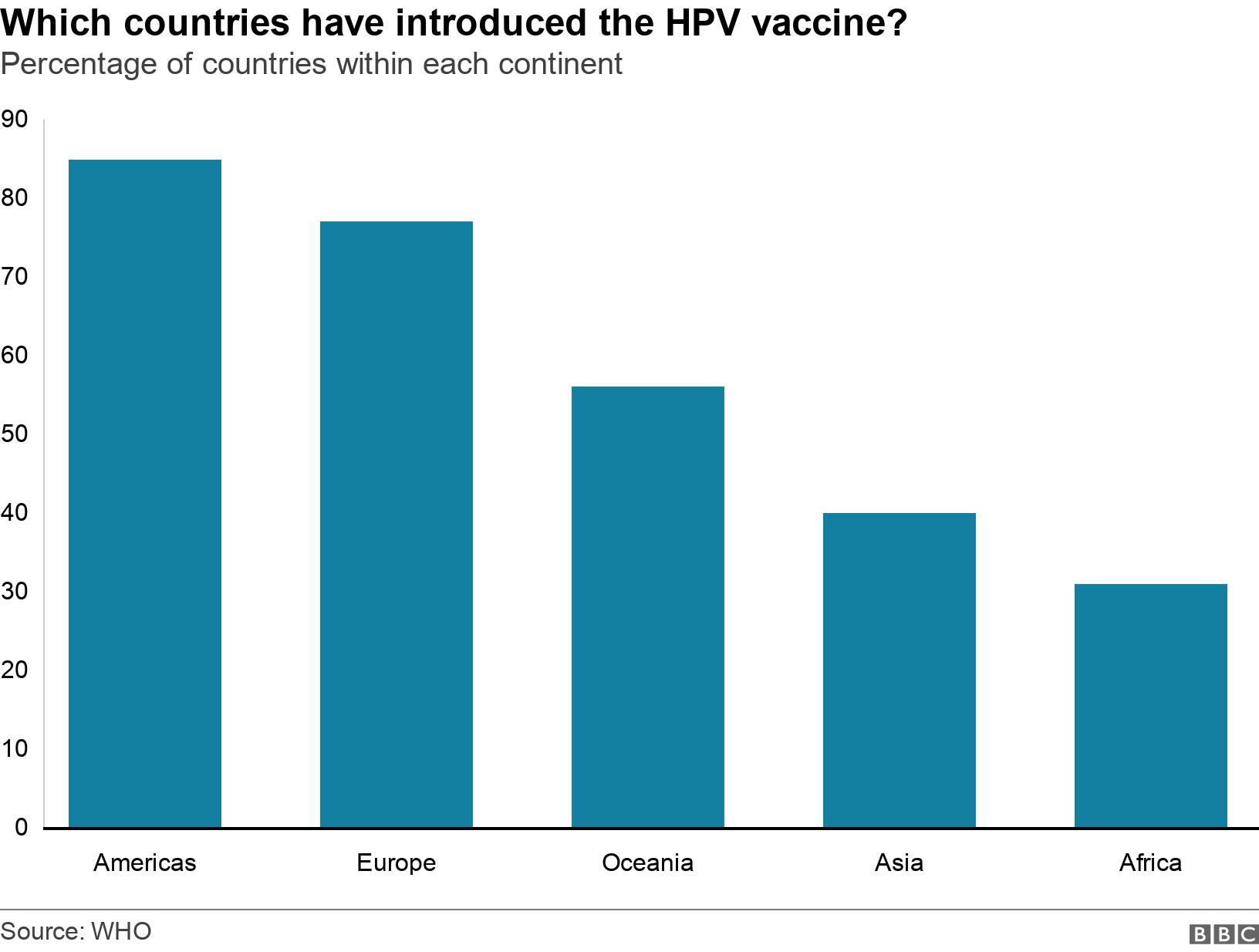
The HPV Vaccine’s Ripple Effect: Predicting a Future Free From Cervical Cancer’s Shadow
Nearly 90% reduction in precancerous cervical lesions in young Dutch women – a figure once considered a distant dream – is now a reality thanks to widespread HPV vaccination. But this isn’t just a Dutch success story; it’s a harbinger of a global shift in preventative healthcare, and a catalyst for re-evaluating how we incentivize public health measures. The question isn’t simply whether vaccination works, but how we can maximize its impact and build a future where cervical cancer is a rarity, not a threat.
Beyond Cervical Cancer: The Expanding Scope of HPV Prevention
The success with cervical cancer prevention is fueling research into HPV’s role in other cancers, including anal, penile, vaginal, vulvar, and oropharyngeal cancers. As our understanding of the virus deepens, we can anticipate broader vaccination recommendations and potentially even therapeutic interventions. This expansion will require significant investment in research and public health infrastructure, but the potential return – a dramatic reduction in the incidence of multiple cancers – is immense. The current focus is largely on young women, but extending vaccination programs to include boys is gaining momentum, offering protection against HPV-related cancers in men and contributing to herd immunity.
The Incentive Debate: Should Rewards Accompany Responsibility?
The debate surrounding financial incentives for parents who vaccinate their children, as discussed in Dutch media, is a crucial one. While the Netherlands currently offers only the vaccine itself, the idea of a healthcare premium discount is gaining traction. This raises complex ethical and economic questions. Is it appropriate to financially reward parents for making choices that benefit public health? Could such incentives create inequities, disproportionately benefiting wealthier families? Or could they be a powerful tool to overcome vaccine hesitancy and achieve higher vaccination rates, ultimately reducing healthcare costs in the long run? The key lies in designing incentive programs that are equitable, transparent, and evidence-based.
Personalized Prevention: The Rise of Risk-Based Screening
As HPV vaccination rates increase, the focus of cervical cancer screening is likely to shift towards more personalized approaches. Traditional Pap smears may be supplemented – or even replaced – by more sophisticated tests that identify high-risk HPV strains and assess individual risk factors. This could lead to more targeted screening intervals, reducing unnecessary anxiety and healthcare costs. Furthermore, advancements in artificial intelligence and machine learning could help analyze screening data more effectively, identifying women who are at higher risk of developing cervical cancer and requiring more frequent monitoring.
The Role of At-Home HPV Testing
The future of cervical cancer screening may also include at-home HPV testing kits. These kits offer convenience and accessibility, potentially increasing screening rates among women who are reluctant to visit a clinic. However, ensuring the accuracy and reliability of these tests, as well as providing appropriate follow-up care for women who test positive, will be critical. Telemedicine and remote monitoring technologies will play an increasingly important role in delivering this care.
Navigating Vaccine Hesitancy in a Post-Success Landscape
Even with compelling evidence of the HPV vaccine’s effectiveness, vaccine hesitancy remains a significant challenge. Misinformation and unfounded fears continue to circulate online and in communities. Combating this requires a multi-pronged approach, including clear and accurate communication from healthcare professionals, targeted public health campaigns, and proactive engagement with communities to address their concerns. The Dutch success story provides a powerful narrative that can be used to counter misinformation and build trust in the vaccine. However, complacency is a danger; continued vigilance and proactive communication are essential to maintain high vaccination rates.
The dramatic decline in precancerous cervical lesions in young Dutch women is a testament to the power of preventative medicine. But it’s also a call to action – a reminder that we must continue to innovate, invest, and advocate for policies that prioritize public health and protect future generations from the devastating impact of HPV-related cancers.
What are your predictions for the future of HPV vaccination and cervical cancer prevention? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.