Nearly 1 in 5 colorectal cancer diagnoses now occur in individuals under the age of 50 – a statistic that’s rewriting the rules of preventative care. For decades, screening guidelines focused on those over 50, but this demographic shift demands a radical reassessment. **Colorectal cancer** isn’t just an ‘older person’s disease’ anymore, and ignoring this reality has devastating consequences.
The Shifting Landscape of Colorectal Cancer
Traditionally, colorectal cancer developed slowly, allowing years for pre-cancerous polyps to grow. However, we’re now seeing more aggressive, fast-growing tumors in younger individuals. Several factors are converging to fuel this alarming trend. Dietary changes – specifically, the rise of ultra-processed foods and a decline in fiber intake – are strongly implicated. The gut microbiome, increasingly recognized as a critical regulator of health, is also under scrutiny. Disruptions to this delicate ecosystem, caused by diet, antibiotics, and lifestyle factors, may be contributing to increased inflammation and cancer risk.
Beyond Diet: Unraveling the Complex Web of Causes
While diet is a significant piece of the puzzle, it’s far from the whole story. Increasing rates of obesity, sedentary lifestyles, and chronic stress are all contributing factors. Emerging research also suggests a potential link between early-life gut microbiome development and long-term colorectal cancer risk. Furthermore, the rise in inflammatory bowel disease (IBD) – Crohn’s disease and ulcerative colitis – significantly elevates the risk of developing colorectal cancer, even at younger ages. This highlights the importance of addressing underlying inflammatory conditions.
The Future of Screening: Personalized and Proactive
The current ‘one-size-fits-all’ screening approach is clearly failing to address the needs of younger populations. The standard colonoscopy, typically recommended starting at age 45 (recently lowered by the US Preventive Services Task Force), may be too late for many. The future of colorectal cancer screening lies in personalized risk assessment and more frequent, targeted interventions. This includes:
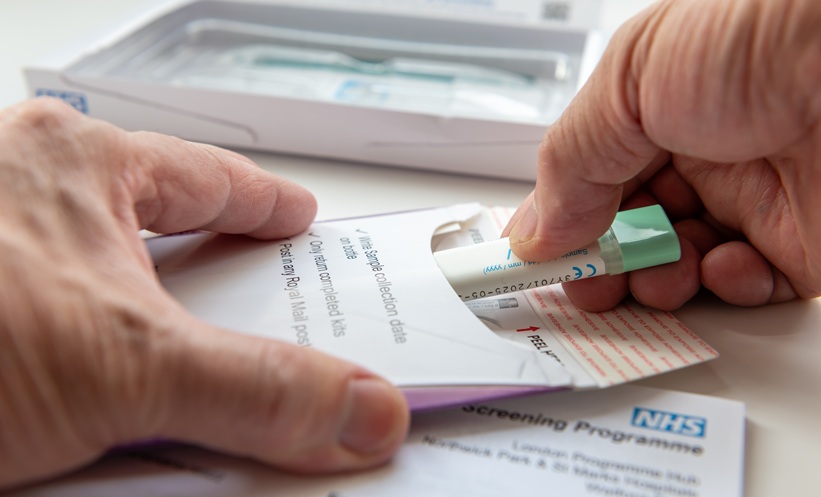
- Advanced Biomarkers: Research is focused on identifying biomarkers in blood or stool that can detect early signs of cancer or pre-cancerous changes. Liquid biopsies, analyzing circulating tumor DNA, hold immense promise for non-invasive early detection.
- Gut Microbiome Analysis: Profiling an individual’s gut microbiome could help identify those at higher risk and guide personalized dietary or probiotic interventions.
- Genetic Predisposition Testing: For individuals with a family history of colorectal cancer, genetic testing can identify inherited mutations that significantly increase their risk.
- Capsule Endoscopy: This non-invasive procedure uses a small camera in a capsule to visualize the entire colon, offering a potentially more comfortable alternative to traditional colonoscopy.
The Role of Artificial Intelligence
Artificial intelligence (AI) is poised to revolutionize colorectal cancer screening. AI-powered algorithms can analyze colonoscopy videos in real-time, identifying subtle polyps that might be missed by the human eye. This technology can improve the accuracy of screening and reduce the risk of interval cancers – cancers that develop between scheduled screenings. AI can also analyze patient data to predict individual risk and personalize screening recommendations.
| Screening Method | Current Status | Future Potential |
|---|---|---|
| Colonoscopy | Standard of care, recommended starting at 45 | AI-assisted polyp detection, improved accuracy |
| FIT (Fecal Immunochemical Test) | Commonly used for annual screening | Integration with microbiome analysis for risk stratification |
| Liquid Biopsy | Research phase | Non-invasive early detection of cancer and pre-cancerous changes |
Navigating the New Reality
The rise in early-onset colorectal cancer is a wake-up call. It’s a stark reminder that preventative care needs to evolve to meet the changing health landscape. Don’t wait for guidelines to catch up. If you experience persistent changes in bowel habits, rectal bleeding, abdominal pain, or unexplained weight loss, consult your doctor immediately. Advocate for your health and demand proactive screening, even if you’re under 50. The future of colorectal cancer prevention depends on it.
Frequently Asked Questions About Early-Onset Colorectal Cancer
- What are the key symptoms of colorectal cancer in younger adults?
- Symptoms can be subtle but include changes in bowel habits (diarrhea, constipation, or narrowing of the stool), rectal bleeding, abdominal pain, bloating, unexplained weight loss, and fatigue. It’s crucial to report any persistent changes to your doctor.
- Should I get a colonoscopy even if I don’t have symptoms?
- If you have a family history of colorectal cancer or other risk factors (like IBD), discuss early screening with your doctor. Even without known risk factors, if you’re concerned, it’s better to be proactive.
- How can I reduce my risk of developing colorectal cancer?
- Adopting a healthy lifestyle is key. This includes eating a high-fiber diet rich in fruits, vegetables, and whole grains, maintaining a healthy weight, exercising regularly, limiting processed foods and red meat, and avoiding smoking.
What are your predictions for the future of colorectal cancer screening and prevention? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.