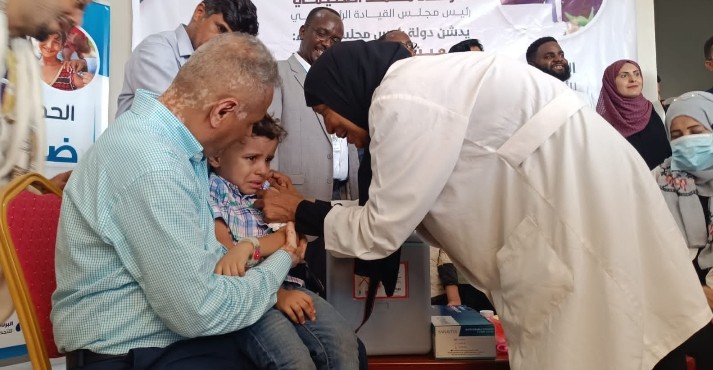
Beyond the Crisis: The Deadly Surge of the Measles Outbreak in Yemen and the Global Warning it Sends
Over 5,600 infections and 21 recorded deaths since the start of the year—these are not just statistics; they are a stark indictment of a collapsing preventive healthcare system. The current Measles Outbreak in Yemen is not a random biological event, but a predictable consequence of systemic failure in one of the world’s most volatile conflict zones. While the immediate focus is on the tragedy unfolding in Marib and the coast of Hadramout, the broader implication is far more sinister: the creation of “immunization gaps” that could turn fragile regions into permanent reservoirs for vaccine-preventable diseases.
The Geography of a Health Emergency
The current surge is not uniform but concentrated in areas where instability is highest. In the coastal regions of Hadramout, health officials are grappling with approximately 1,700 suspected cases, while Marib continues to report fatalities that underscore the lethality of the virus when met with inadequate medical intervention.
Measles is one of the most contagious diseases known to man. In a stable environment, it is entirely preventable. In Yemen, however, the virus is exploiting the ruins of a healthcare infrastructure decimated by years of war, leaving thousands of children vulnerable to a disease that should have been eradicated decades ago.
| Region/Scope | Impact Status | Key Data Point |
|---|---|---|
| Nationwide (Yemen) | Critical Surge | 5,600+ Cases / 21 Deaths |
| Coastal Hadramout | Alarming Spread | ~1,700 Suspected Cases |
| Marib | High Mortality | Confirmed Fatalities |
The “Immunization Gap”: A Forward-Looking Threat
What does this outbreak tell us about the future of global health security? The Measles Outbreak in Yemen serves as a canary in the coal mine for the “Immunization Gap.” This occurs when a significant percentage of a population misses primary vaccination series due to displacement or systemic collapse.
When these gaps persist, we move from sporadic outbreaks to endemic instability. The danger is that these regions become breeding grounds for viral mutations or portals through which eradicated diseases can re-enter the global travel stream. If the international community views this merely as a local tragedy rather than a systemic failure, we risk seeing similar patterns in other fragile states.
The compounding effect of malnutrition
The lethality of measles in Yemen is amplified by a secondary crisis: chronic malnutrition. A child with vitamin A deficiency is significantly more likely to succumb to measles complications, such as pneumonia or encephalitis. This synergy between hunger and disease creates a death spiral that simple vaccination drives cannot fix in isolation.
The challenge of vaccine hesitancy in conflict zones
Beyond physical access, there is the psychological barrier. In areas of extreme instability, trust in institutional health mandates often erodes. When health authorities in Wadi Hadramout urge parents to vaccinate their children, they are fighting not just a virus, but a profound lack of trust in the systems meant to protect the population.
Architecting a Resilient Response
To stop the current trajectory, the approach must shift from reactive “firefighting” to a resilient health architecture. This involves moving beyond temporary clinics toward community-led immunization networks that can operate independently of central government stability.
The integration of digital health tracking—even via basic mobile networks—could allow health workers to identify “zero-dose children” in real-time, ensuring that displacement doesn’t lead to the loss of a child’s medical history. The goal is to build a decentralized shield of immunity that can withstand the shocks of political instability.
Frequently Asked Questions About the Measles Outbreak in Yemen
Why is measles so deadly in Yemen compared to other regions?
The high mortality rate is driven by a combination of low vaccination coverage, severe widespread malnutrition (especially vitamin A deficiency), and the total collapse of pediatric intensive care units in conflict-affected cities.
Can the current outbreak spread beyond Yemen’s borders?
Yes. Because measles is highly airborne and contagious, any movement of displaced populations or regional travel can carry the virus across borders, posing a risk to neighboring countries with similar gaps in immunization coverage.
What is the most effective way to stop the surge?
The immediate solution is mass “catch-up” vaccination campaigns targeting children who missed their primary doses, coupled with nutritional support to strengthen the immune systems of affected children.
The tragedy in Yemen is a reminder that health is the first casualty of war and the hardest to rebuild. The Measles Outbreak in Yemen is a call to action for a new model of humanitarian health: one that prioritizes permanent, community-based preventive care over temporary emergency aid. If we fail to bridge the immunization gap now, we are simply waiting for the next, perhaps more lethal, pathogen to find an open door.
What are your predictions for the future of global health security in conflict zones? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.