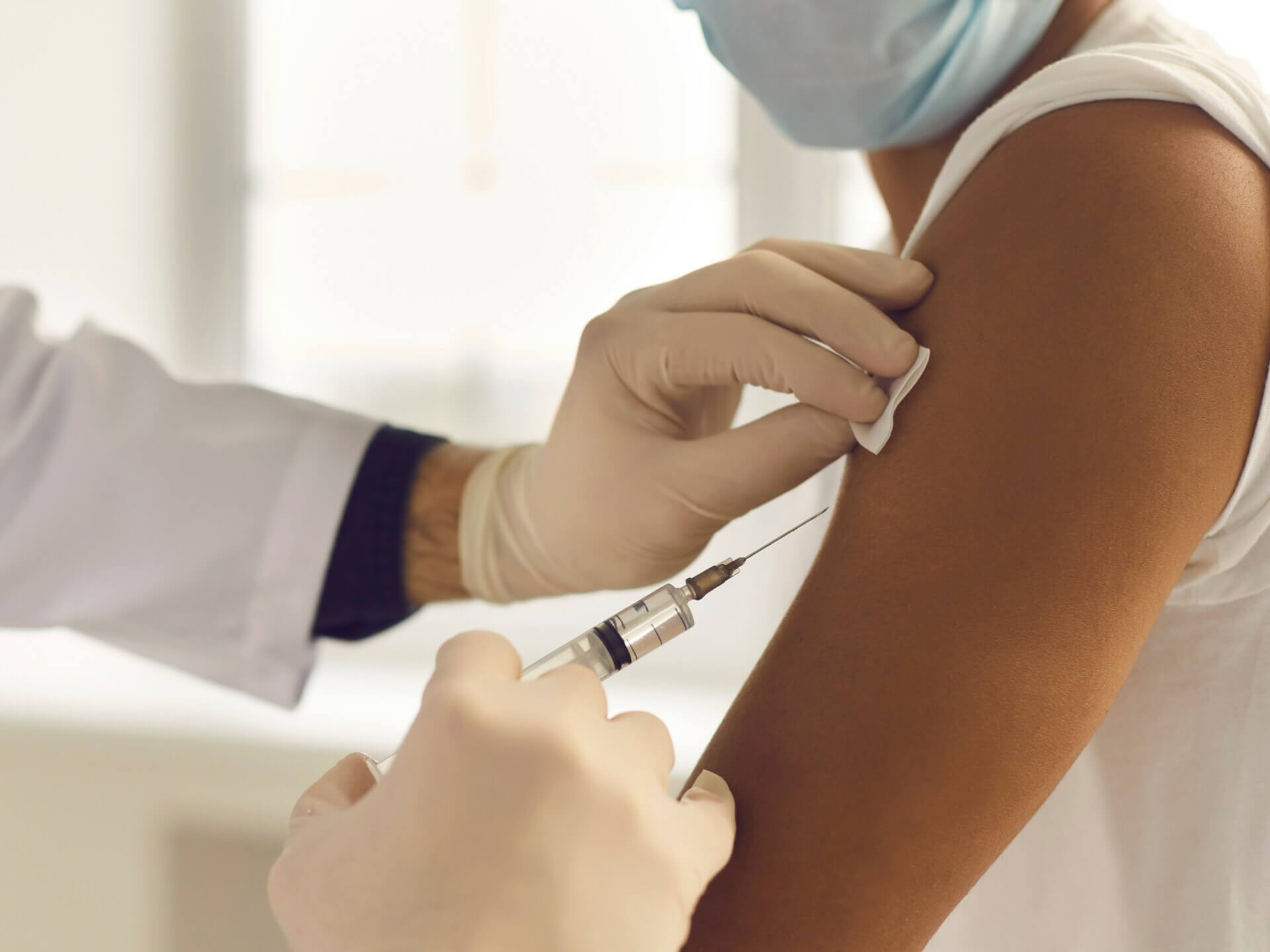
Beyond the Outbreak: What the Return of Diphtheria Reveals About Australia’s Public Health Future
For decades, the medical community viewed diphtheria as a ghost of the early 20th century—a terrifying respiratory killer that had been effectively silenced by the triumph of mass immunization. However, the recent and rapid Diphtheria outbreak Australia is currently witnessing, particularly with cases quadrupling in the Northern Territory within a single month and emerging clusters in Western Australia, signals a dangerous shift. We are entering an era where the very success of vaccines has created a “complacency loop,” leaving populations vulnerable to diseases we mistakenly believed were gone for good.
The Anatomy of a Resurgence
Diphtheria is not a new threat, but its return is a modern warning. Caused by the bacterium Corynebacterium diphtheriae, the disease creates a thick membrane in the throat that can lead to breathing obstruction and heart failure. While once a leading cause of childhood mortality, it had dwindled to a rarity in developed nations.
The current surge in the Northern Territory and Western Australia isn’t merely a statistical anomaly; it is a localized failure of herd immunity. When vaccination rates dip below a critical threshold—even in small pockets of a population—the environment becomes a playground for dormant pathogens to regain a foothold.
The Regional Vulnerability Gap
The concentration of cases in regional and remote areas highlights a persistent disparity in healthcare delivery. Access to timely boosters and childhood immunization schedules often falters in the “last mile” of public health logistics.
Are these outbreaks isolated incidents, or are they indicators of a broader systemic fragility? The data suggests that when rural health infrastructure is stretched, the first casualty is often the preventative maintenance of vaccine schedules, turning remote communities into epicenters for preventable outbreaks.
| Metric | Historical Context (Pre-Vaccine) | Modern Trend (Current Outbreaks) |
|---|---|---|
| Mortality Rate | Hundreds of deaths annually | Low, but high risk for unvaccinated |
| Primary Driver | Lack of immunization | Vaccine complacency & access gaps |
| Spread Velocity | Steady endemic presence | Rapid spikes in regional clusters |
The “Complacency Loop” and Future Risks
The most significant risk facing Australia is not the bacterium itself, but the psychological effect of success. When a disease disappears from the public consciousness, the perceived risk of the illness drops below the perceived “hassle” of getting a booster shot.
This phenomenon is not limited to diphtheria. We are seeing a mirrored trend globally with measles and pertussis. The future of public health will likely be defined by a battle against informational decay—the loss of collective memory regarding why these vaccines were necessary in the first place.
Predicting the Next Wave
If the current trend persists, we can expect a shift in how health authorities approach immunization. We are moving toward a model of precision public health, where data analytics are used to identify “immunity deserts” in real-time before an outbreak occurs.
Instead of blanket national campaigns, the future will rely on hyper-local interventions. This means mobile vaccination clinics that trigger based on regional dip-rates and digital health passports that alert citizens to booster requirements based on their specific geographic risk profile.
Modernizing the Defensive Strategy
To prevent the Diphtheria outbreak Australia is facing from becoming a permanent fixture of the landscape, a shift in strategy is required. We must move from a reactive “outbreak response” mode to a proactive “immunity maintenance” mode.
This involves integrating vaccination records more seamlessly into primary care and utilizing AI-driven outreach to target individuals who have fallen through the cracks of the National Immunisation Program (NIP). The goal is to eliminate the “immunity gaps” that allow these bacteria to migrate from regional clusters to urban centers.
Frequently Asked Questions About the Return of Diphtheria
Is the current diphtheria outbreak a sign of vaccine failure?
No. The vaccines remain highly effective. The outbreaks are a result of vaccine failure at the population level (low uptake or missed boosters), not a failure of the medicine itself.
Who is most at risk during these regional spikes?
Unvaccinated individuals, children who have missed their primary series, and adults who have not received a booster dose in the last 10 years.
Could this lead to a nationwide epidemic?
While unlikely given Australia’s overall high vaccination rates, localized clusters can expand if herd immunity continues to erode in specific demographics or regions.
What is the long-term outlook for vaccine-preventable diseases (VPDs) in Australia?
The trend suggests a cyclical pattern where diseases reappear as public awareness fades. The long-term solution is a shift toward lifelong immunization education and modernized delivery systems.
The return of diphtheria is a stark reminder that medical victory is never permanent; it is a state of constant maintenance. As we look toward the future, the ability to sustain high levels of community immunity in the face of growing skepticism and logistical hurdles will be the true measure of our public health resilience. The cost of complacency is a return to a past we thought we had outgrown.
What are your predictions for the future of preventative healthcare in regional Australia? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.