Beyond Weight Loss: Could GLP-1 Drugs Revolutionize Addiction Treatment?
Nearly 30 million Americans are currently struggling with substance use disorder, a crisis that costs the nation over $740 billion annually. But what if a solution wasn’t found in traditional addiction therapies, but in a class of drugs initially designed to treat type 2 diabetes and obesity? Emerging research, including a groundbreaking study analyzing data from over 600,000 individuals, suggests that **GLP-1 receptor agonists** – medications like Ozempic and Mounjaro – may offer a surprising new avenue for preventing and treating addiction across a wide spectrum of substances.
The Unexpected Link: How GLP-1s Impact the Brain
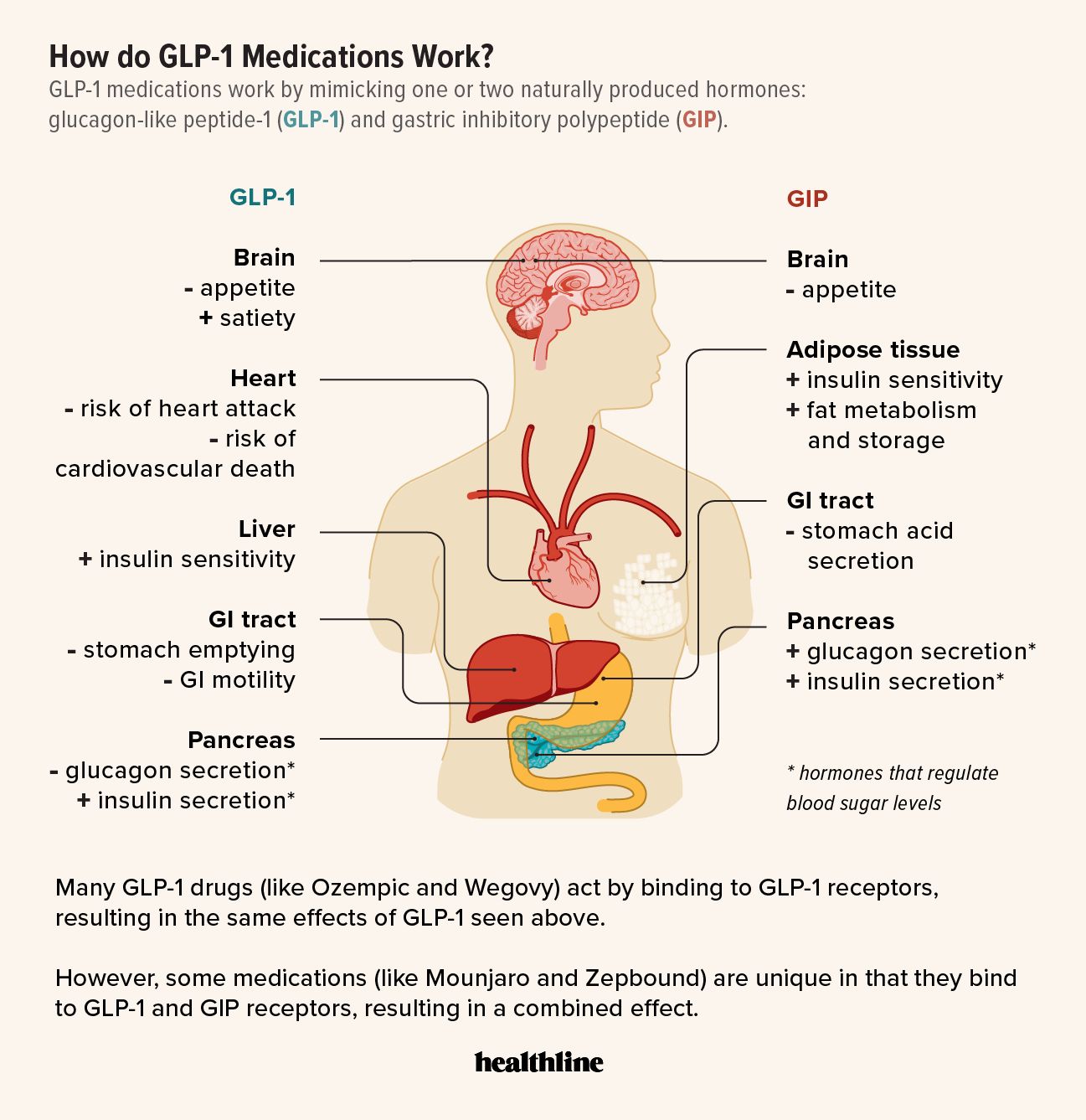
GLP-1 (glucagon-like peptide-1) drugs work by mimicking a naturally occurring hormone that regulates blood sugar, increases insulin release, and slows gastric emptying. However, the impact extends far beyond metabolism. These drugs act on the brain’s reward system, specifically influencing dopamine pathways. Traditionally, addiction has been understood as a hijacking of this reward system, where substances trigger an excessive dopamine release, leading to compulsive behavior. GLP-1 agonists appear to modulate this system, potentially reducing cravings and the reinforcing effects of addictive substances.
The 600,000-Person Study: A Broad Spectrum of Protection
The recent study, published in several leading medical journals, revealed a consistent pattern: individuals taking GLP-1 receptor agonists exhibited a significantly lower risk of developing new substance use disorders, including alcohol, opioids, cannabis, and stimulants. The reduction in risk varied depending on the substance, but the overall trend was remarkably consistent. This isn’t limited to preventing *new* addictions; the data also suggests a protective effect against the worsening of existing addictive behaviors.
Beyond Correlation: Unraveling the Mechanisms
While the study demonstrates a strong correlation, the precise mechanisms behind this protective effect are still being investigated. Researchers hypothesize several contributing factors. Beyond dopamine modulation, GLP-1 agonists may reduce impulsive behavior, improve self-control, and address underlying metabolic imbalances often associated with addiction. Furthermore, the weight loss often achieved with these medications could indirectly reduce the appeal of substances used for appetite suppression or emotional coping.
The Future of Addiction Treatment: A Paradigm Shift?
The implications of this research are profound. Currently, addiction treatment relies heavily on behavioral therapies, support groups, and medications targeting specific neurotransmitter systems. While effective for some, these approaches often have limited success rates and high relapse rates. GLP-1 agonists offer a potentially novel approach, addressing the underlying neurobiological vulnerabilities that contribute to addiction. However, it’s crucial to avoid oversimplification.
Challenges and Considerations
Several challenges remain. GLP-1 agonists are not without side effects, including nausea, vomiting, and potential risks for pancreatitis. Long-term effects on the brain and the potential for dependence on the medication itself require further investigation. Moreover, access to these drugs is currently limited by cost and supply chain issues. Ethical considerations surrounding the use of a medication primarily intended for metabolic disorders to treat addiction also need careful consideration.
However, the potential benefits are too significant to ignore. We may see a future where GLP-1 agonists are used as a preventative measure for individuals at high risk of developing addiction – those with a family history of substance use disorder, or those struggling with obesity and metabolic syndrome. Combination therapies, integrating GLP-1 agonists with traditional addiction treatments, could also prove highly effective.
The Convergence of Metabolic and Mental Health
This research underscores a growing understanding of the intricate connection between metabolic health and mental health. Obesity, diabetes, and addiction often co-occur, sharing common neurobiological pathways. The success of GLP-1 agonists in addressing both metabolic and addictive behaviors highlights the need for a more holistic approach to healthcare, one that recognizes the interconnectedness of these conditions.
The coming years will be critical for further research, clinical trials, and the development of targeted therapies. The potential to repurpose existing medications like Ozempic and Mounjaro to combat the addiction crisis represents a beacon of hope, offering a new path towards recovery and a healthier future.
Frequently Asked Questions About GLP-1s and Addiction
Will GLP-1 drugs replace traditional addiction treatments?
It’s unlikely GLP-1s will completely replace existing treatments. Instead, they are likely to become a valuable addition to the toolkit, particularly for individuals who haven’t responded well to traditional therapies or are at high risk of relapse. A combination approach is most probable.
Are GLP-1 drugs safe for long-term use in addiction treatment?
Long-term safety data is still being collected. While generally considered safe for metabolic conditions, the effects of prolonged use specifically for addiction require further study. Potential side effects and the risk of dependence need to be carefully monitored.
Who is most likely to benefit from GLP-1 treatment for addiction?
Individuals with obesity, metabolic syndrome, or a family history of addiction may be particularly likely to benefit. Those struggling with multiple substance use disorders or who have experienced repeated relapses could also be strong candidates.
What are your predictions for the role of GLP-1 drugs in addiction treatment? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.