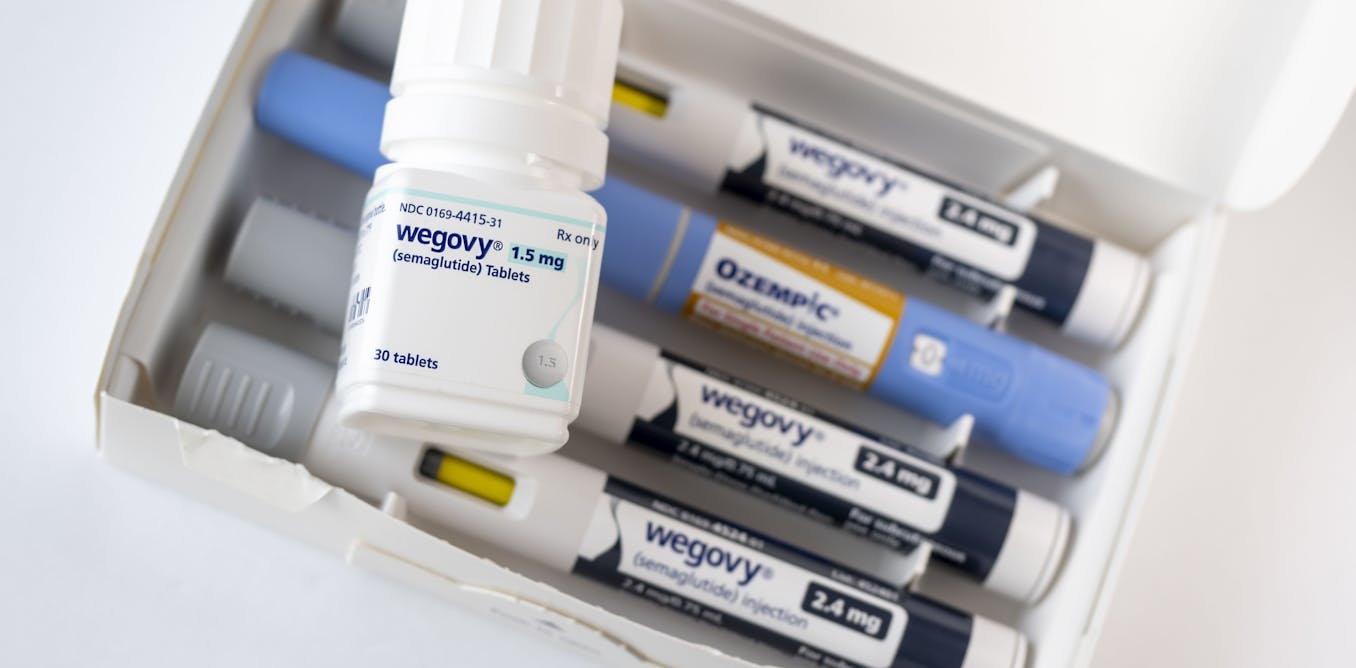
Could Drugs for Diabetes and Obesity Hold the Key to Overcoming Addiction?
A groundbreaking shift in addiction treatment may be on the horizon, stemming from an unexpected source: medications originally designed to manage type 2 diabetes and obesity. Emerging evidence suggests that GLP-1 drugs, like semaglutide and tirzepatide, could significantly reduce cravings across a wide range of addictive substances, offering a potential breakthrough for millions struggling with substance use disorders.
The story began with individual patient experiences. A veteran, after decades of unsuccessful attempts, found his cigarette cravings vanished shortly after starting a GLP-1 drug for diabetes. Another patient, struggling with alcohol dependence, reported a similar loss of desire after beginning the medication for weight management. These anecdotal reports quickly multiplied, with individuals sharing stories of diminished cravings for opioids, cocaine, and other substances – all without intentionally seeking addiction treatment.
The Science Behind Curbing Cravings
These medications, initially developed to regulate blood sugar and promote weight loss, work by mimicking a naturally occurring hormone called glucagon-like peptide-1 (GLP-1). But GLP-1’s influence extends beyond metabolism. It also plays a crucial role in brain regions governing reward, motivation, and stress – the very circuits hijacked by addiction. At therapeutic doses, GLP-1 drugs cross the blood-brain barrier, modulating dopamine signaling in the brain’s reward center and effectively reducing the pleasurable sensation associated with addictive substances.
Animal studies further support this theory. Research has shown that rodents administered GLP-1 drugs exhibit decreased alcohol consumption, reduced cocaine self-administration, and diminished interest in nicotine. Experiments with green vervet monkeys, known to voluntarily consume alcohol, demonstrated a similar reduction in drinking without any signs of discomfort, suggesting the drugs lessen the reward value of alcohol rather than inducing aversion.
Real-World Data Reveals Striking Results
To investigate these effects in humans, researchers analyzed the electronic health records of over 600,000 patients with type 2 diabetes within the U.S. Department of Veterans Affairs healthcare system. Employing a rigorous, quasi-experimental design that mirrored the standards of randomized controlled trials, they compared outcomes between patients who initiated GLP-1 therapy and those who did not, adjusting for a wide range of demographic and clinical factors.
The findings were compelling. Among individuals already struggling with addiction, GLP-1 drug use was associated with a remarkable 50% reduction in deaths related to substance use. Furthermore, the study revealed a 39% decrease in overdoses, a 26% reduction in drug-related hospitalizations, and a 25% drop in suicide attempts. Over a three-year period, this translated to roughly 12 fewer serious events per 1,000 individuals using GLP-1 drugs, including two fewer deaths.
Perhaps even more significant, the drugs appeared to prevent addiction from taking hold in the first place. Individuals without a prior history of substance use disorder who were prescribed GLP-1 medications demonstrated an 18% lower risk of developing alcohol use disorder, a 25% lower risk of opioid use disorder, and approximately a 20% lower risk of cocaine and nicotine dependence. This suggests a preventative effect, potentially shielding vulnerable individuals from the grip of addiction.
These results align with a growing body of observational studies. A Swedish nationwide study of over 227,000 individuals with alcohol use disorder found a 36% lower risk of alcohol-related hospitalizations among those taking GLP-1 drugs – a more substantial reduction than observed with naltrexone, a traditionally prescribed medication for alcohol dependence. Further research has linked GLP-1 drugs to reduced rates of new and recurring alcohol use disorder, cannabis use disorder, nicotine dependence, and opioid overdose.
Ongoing randomized controlled trials are providing even more direct evidence. Studies have shown that semaglutide reduces both craving and alcohol consumption in individuals with alcohol use disorder, while dulaglutide has demonstrated a reduction in drinking behavior. Dozens of additional trials are currently underway, promising a more comprehensive understanding of these drugs’ potential in addiction treatment.
What if the key to unlocking widespread recovery from addiction wasn’t a specialized treatment center, but a medication already being prescribed to millions? Could this be the paradigm shift addiction medicine has been waiting for?
Did You Know?
Navigating the Unanswered Questions
While the evidence is promising, several questions remain. Many individuals discontinue GLP-1 drugs after achieving weight loss or managing their diabetes, often experiencing a return of appetite. It’s unclear whether a similar “rebound” effect would occur with addiction, and what the implications would be for individuals in recovery. Furthermore, the long-term effects of continuous GLP-1 use on brain function and motivation require further investigation.
Because GLP-1 drugs engage the brain’s reward circuitry, there’s a theoretical possibility of dampening overall motivational drive. Whether this could translate into real-world consequences, such as reduced initiative or performance, remains an open question.
GLP-1 drugs represent a novel approach to addiction treatment, potentially offering benefits across multiple substances simultaneously. Their widespread availability, coupled with the existing infrastructure for prescription and delivery, positions them as a uniquely accessible solution. However, further research is crucial to fully understand their long-term effects and optimize their use in combating the global addiction crisis.
Frequently Asked Questions About GLP-1 Drugs and Addiction
- Can GLP-1 drugs cure addiction? While promising, GLP-1 drugs are not a cure for addiction. Current research suggests they can significantly reduce cravings and the risk of relapse, but they are likely most effective when combined with other forms of support and therapy.
- Are GLP-1 medications safe for long-term use in addiction treatment? The long-term safety of GLP-1 drugs for addiction treatment is still being studied. Potential side effects and the possibility of rebound cravings require careful monitoring and further investigation.
- What types of addiction have shown a response to GLP-1 drugs? Studies have indicated potential benefits for alcohol, opioid, cocaine, nicotine, and cannabis use disorders. Research is ongoing to explore their effectiveness across a broader range of addictive behaviors.
- How do GLP-1 drugs differ from existing addiction medications? Unlike many existing addiction medications that target specific substances, GLP-1 drugs appear to address the underlying brain mechanisms driving cravings across multiple substances.
- Will GLP-1 drugs become a standard treatment for addiction? While not yet approved for addiction treatment, the growing body of evidence suggests that GLP-1 drugs could become an important part of a comprehensive addiction treatment plan in the future.
The potential of these medications to reshape the landscape of addiction treatment is undeniable. As research continues and our understanding deepens, GLP-1 drugs may offer a beacon of hope for millions seeking lasting recovery.
What are your thoughts on the potential of GLP-1 drugs to revolutionize addiction treatment? Do you know anyone who has experienced similar benefits while taking these medications?
Share this article with your network to spark a conversation and help raise awareness about this groundbreaking research!
Disclaimer: This article provides general information and should not be considered medical advice. Consult with a qualified healthcare professional for personalized guidance on addiction treatment and medication options.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.