Nearly 6 million Americans are living with Alzheimer’s disease, and that number is projected to more than double by 2050. But what if the battle against this devastating illness isn’t solely fought in the brain? A growing body of evidence suggests that the origins of Alzheimer’s, and other forms of cognitive decline, may lie much further south – in the complex ecosystem of the human gut.
The Inflammatory Cascade: From Gut to Brain
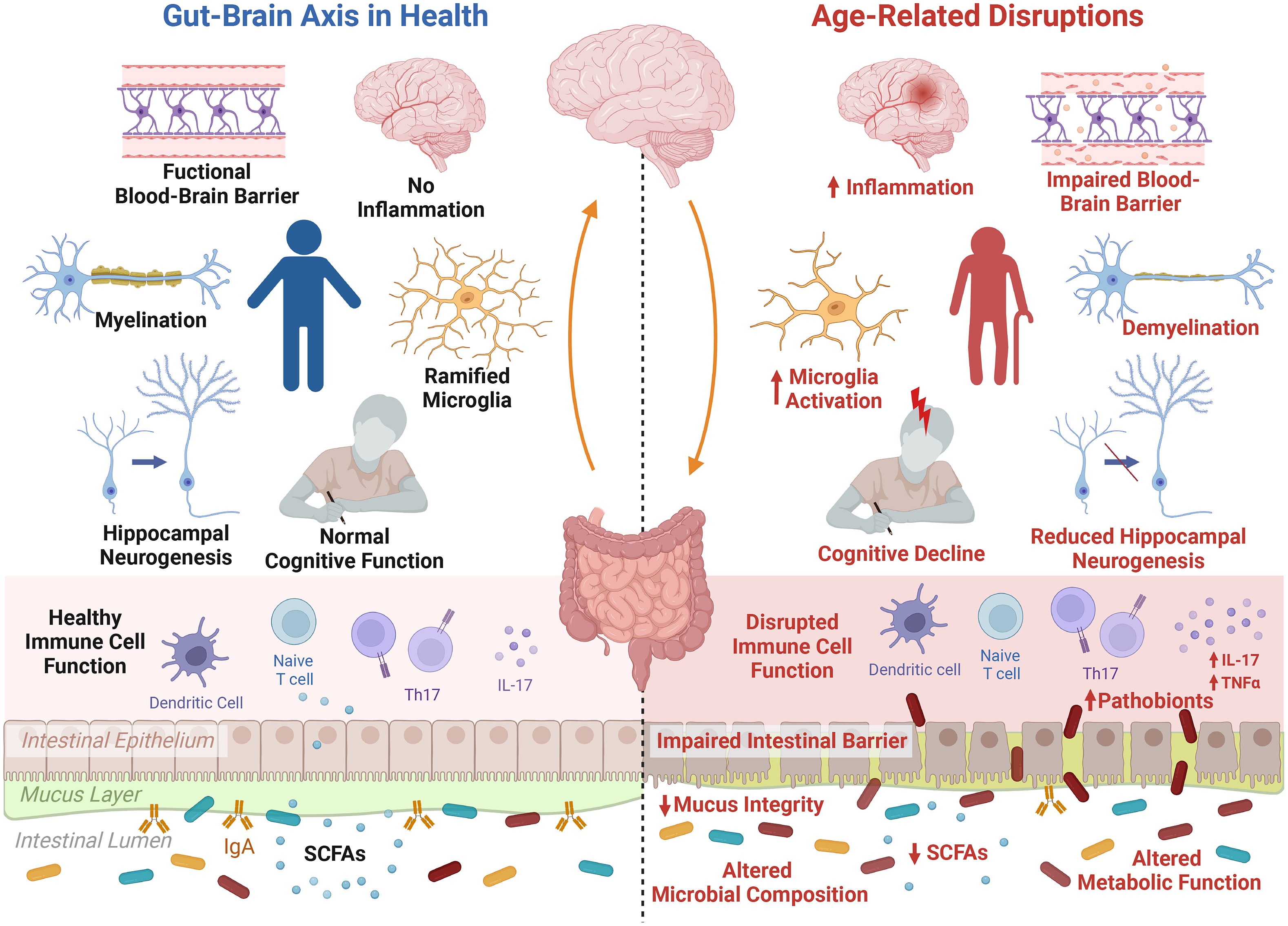
For decades, the focus on Alzheimer’s disease has centered around amyloid plaques and tau tangles in the brain. However, recent research increasingly points to inflammation as a critical driver of neurodegeneration. But where does this inflammation originate? Studies are revealing a surprising connection: a compromised gut barrier, often referred to as “leaky gut,” allows bacterial byproducts to enter the bloodstream, triggering a systemic inflammatory response. This inflammation doesn’t just stay in the periphery; it travels to the brain, contributing to neuronal damage and cognitive impairment.
Beyond the Brain: Peripheral Inflammation as an Early Indicator
The traditional view of Alzheimer’s as a purely brain-centric disease is rapidly evolving. Emerging data suggests that inflammation may begin not in the brain itself, but in peripheral tissues like the skin, lungs, and – crucially – the gut. This means that early detection of systemic inflammation, potentially through simple blood tests analyzing inflammatory markers, could offer a window of opportunity for preventative intervention. The Fisher Center for Alzheimer’s Research Foundation is actively investigating these peripheral biomarkers as potential early warning signals.
The Microbiome’s Role: A Delicate Ecosystem
The gut microbiome – the trillions of bacteria, fungi, viruses, and other microorganisms residing in our digestive tract – plays a pivotal role in regulating inflammation and immune function. An imbalanced microbiome, known as dysbiosis, can exacerbate inflammation and contribute to a leaky gut. Specific bacterial species have been linked to both increased and decreased risk of cognitive decline. For example, certain strains of Bifidobacterium and Lactobacillus appear to have neuroprotective effects, while an overabundance of pro-inflammatory bacteria can accelerate neurodegeneration.
Supplements and Dietary Interventions: Promising Avenues
While research is still ongoing, several readily available interventions show promise in modulating the gut microbiome and mitigating inflammation. Studies have highlighted the potential benefits of specific supplements, including curcumin (found in turmeric) and omega-3 fatty acids, in improving cognitive function and reducing neuroinflammation. Earth.com recently reported on a common, inexpensive supplement showing rapid memory improvements and dementia prevention, though further research is needed to confirm these findings and identify the specific mechanisms involved. However, it’s crucial to remember that supplements are not a magic bullet; a holistic approach to gut health, including a diverse, fiber-rich diet, is paramount.
The Future of Cognitive Health: Personalized Microbiome Therapies
Looking ahead, the future of cognitive health likely lies in personalized microbiome therapies. Advances in metagenomic sequencing allow for detailed analysis of an individual’s gut microbiome composition. This information can be used to tailor dietary recommendations, probiotic formulations, and even fecal microbiota transplantation (FMT) to restore microbial balance and reduce inflammation. Imagine a future where a simple stool test can predict your risk of cognitive decline and guide personalized interventions to protect your brain.
Furthermore, the development of “psychobiotics” – probiotics specifically selected for their positive effects on mental health – is gaining momentum. These targeted probiotics could potentially address the gut-brain axis directly, improving mood, reducing anxiety, and enhancing cognitive function. The convergence of microbiome research, immunology, and neuroscience is poised to revolutionize our understanding and treatment of age-related cognitive decline.
The link between gut health and brain health is no longer a fringe theory; it’s a rapidly evolving field with profound implications for preventative medicine. By prioritizing gut microbiome modulation, we may unlock a powerful new strategy for preserving cognitive function and combating the growing global burden of Alzheimer’s disease and dementia.
Frequently Asked Questions About the Gut-Brain Connection
What is the gut-brain axis?
The gut-brain axis is a bidirectional communication network between the gut microbiome and the brain. This communication occurs through various pathways, including the vagus nerve, the immune system, and the production of neurotransmitters.
Can I improve my gut health through diet?
Absolutely. A diet rich in fiber, fruits, vegetables, and fermented foods promotes a diverse and healthy gut microbiome. Limiting processed foods, sugar, and unhealthy fats is also crucial.
Is fecal microbiota transplantation (FMT) a viable treatment for cognitive decline?
FMT is still an experimental treatment for cognitive decline, but early studies are showing promising results. More research is needed to determine its long-term efficacy and safety.
What role does inflammation play in Alzheimer’s disease?
Chronic inflammation is now recognized as a major contributor to the development and progression of Alzheimer’s disease. It damages neurons, disrupts brain function, and accelerates cognitive decline.
What are your predictions for the future of gut-based therapies for cognitive health? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.