The Silent Heart Risk: How Ancestry-Specific Genetics are Rewriting Cardiovascular Care
Nearly 40% of African Americans have high blood pressure, a leading risk factor for heart disease – a statistic that has long puzzled researchers. Now, a groundbreaking study reveals a critical piece of the puzzle: a common genetic variant, specific to people of African ancestry, significantly elevates the risk of dilated cardiomyopathy, a dangerous weakening of the heart muscle. This isn’t simply about identifying a risk factor; it’s about recognizing that decades of cardiovascular research, largely based on populations of European descent, have overlooked crucial genetic nuances, leaving a vulnerable population at a disproportionate disadvantage.
Unpacking the CD36 Variant and its Impact
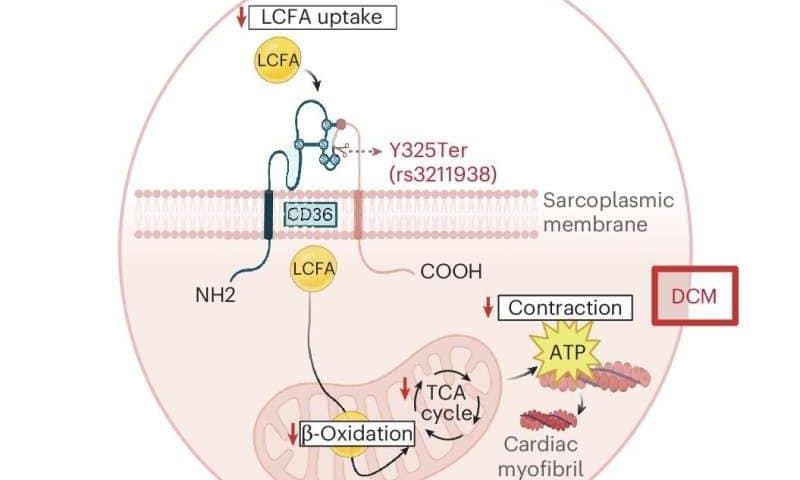
The research, published in Nature, focuses on a “nonsense variant” within the CD36 gene. This variant leads to a truncated, non-functional protein, disrupting the gene’s role in fatty acid metabolism and inflammation. While CD36 has been linked to cardiovascular health before, this study is the first to pinpoint a specific variant strongly associated with dilated cardiomyopathy *and* prevalent within African ancestry populations. This is a critical distinction. It’s not that CD36 is universally problematic, but rather that this specific alteration carries a heightened risk for a defined group.
Dilated Cardiomyopathy: A Silent Threat
Dilated cardiomyopathy often progresses without noticeable symptoms in its early stages. As the heart muscle weakens and enlarges, it struggles to pump blood effectively, leading to shortness of breath, fatigue, and swelling in the legs and feet. Left untreated, it can lead to heart failure, arrhythmias, and even sudden cardiac death. Early detection is paramount, but historically, diagnostic criteria and risk assessments haven’t adequately accounted for the genetic predispositions of diverse populations.
The Rise of Precision Cardiology: A Future Tailored to Your Genes
This discovery isn’t an isolated incident. It’s a powerful example of the growing need for precision cardiology – an approach that moves beyond “one-size-fits-all” treatments and considers an individual’s genetic makeup, lifestyle, and environmental factors. The era of genomic medicine is upon us, and it’s poised to revolutionize how we prevent, diagnose, and treat heart disease.
Beyond CD36: The Search for Ancestry-Specific Risk Factors
The CD36 variant is likely just the tip of the iceberg. Researchers are now actively investigating other genetic variations that may disproportionately affect specific ethnic groups. Expect to see a surge in studies focusing on pharmacogenomics – how genes influence a person’s response to medications – to ensure that treatments are both effective and safe for all patients. This includes re-evaluating existing drug dosages and exploring novel therapies tailored to unique genetic profiles.
The Role of AI and Machine Learning in Genetic Risk Assessment
Analyzing the vast amounts of genomic data required for precision cardiology is a monumental task. Artificial intelligence (AI) and machine learning (ML) are emerging as essential tools, capable of identifying complex patterns and predicting individual risk with increasing accuracy. AI algorithms can sift through genomic data, clinical records, and lifestyle information to create personalized risk scores, enabling proactive interventions and preventative care. Imagine a future where a simple genetic test, analyzed by AI, provides a detailed cardiovascular health forecast, allowing individuals to make informed decisions about their health.
| Metric | Current Status | Projected by 2030 |
|---|---|---|
| Genetic Testing for Cardiovascular Risk | ~5% of at-risk individuals | >30% of at-risk individuals |
| AI-Driven Risk Prediction Accuracy | 70% | 90% |
| Personalized Cardiovascular Treatment Plans | Limited | Widespread |
Addressing Health Disparities: A Call for Inclusive Research
The CD36 discovery underscores a critical ethical imperative: the need for greater diversity in biomedical research. Historically, underrepresentation of minority groups in clinical trials and genetic studies has led to biased results and perpetuated health disparities. Investing in inclusive research initiatives is not just a matter of fairness; it’s essential for advancing scientific knowledge and improving health outcomes for *all* populations. This requires building trust within communities, addressing systemic barriers to participation, and ensuring that research findings are translated into equitable healthcare practices.
Frequently Asked Questions About Ancestry-Specific Heart Disease Risk:
Frequently Asked Questions About Ancestry-Specific Heart Disease Risk
Q: What does it mean to have a “nonsense variant” in a gene?
A: A nonsense variant introduces a premature “stop” signal during protein production, resulting in a truncated, non-functional protein. This can disrupt the gene’s normal function and lead to disease.
Q: Is genetic testing for CD36 available now?
A: While not yet standard practice, genetic testing for the CD36 variant is becoming increasingly available through specialized laboratories and research studies. Talk to your doctor to see if testing is appropriate for you.
Q: What can I do to reduce my risk of heart disease if I have African ancestry?
A: Maintain a healthy lifestyle, including a balanced diet, regular exercise, and stress management. Be aware of your family history and discuss your risk factors with your doctor. Early detection and preventative care are crucial.
The identification of the CD36 variant is a pivotal moment in cardiovascular medicine. It’s a reminder that genetics are not destiny, but understanding our genetic predispositions empowers us to take proactive steps towards a healthier future. As we move towards a more personalized and inclusive approach to healthcare, we can finally begin to close the gap in cardiovascular health disparities and ensure that everyone has the opportunity to live a long and healthy life.
What are your predictions for the future of precision cardiology and its impact on diverse populations? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.