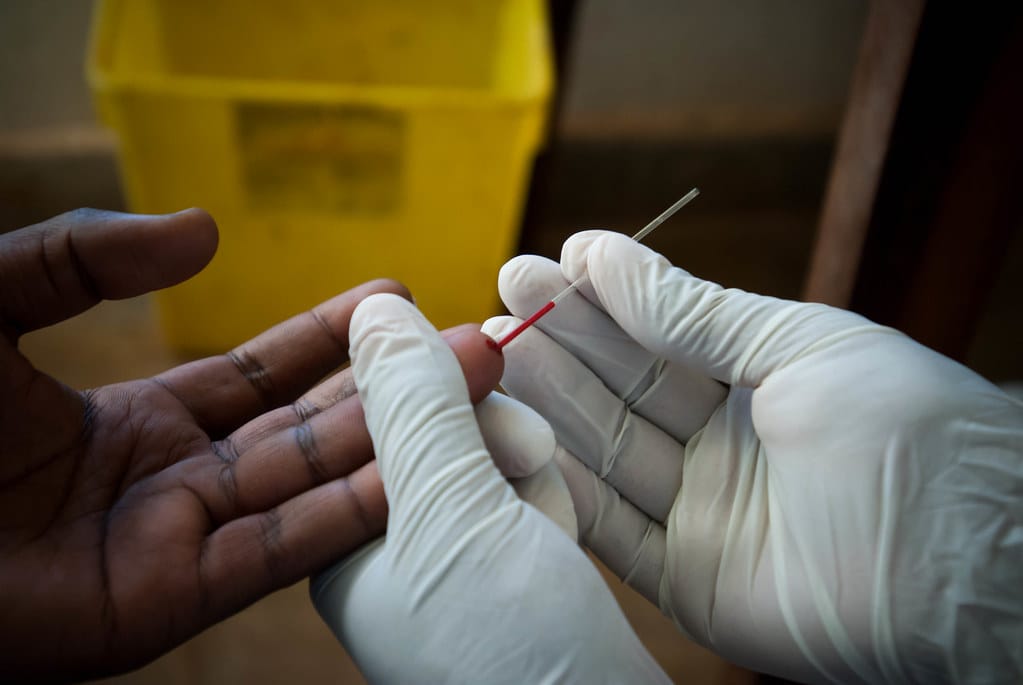
The fight against HIV in eastern and southern Africa faces a critical, and widening, gender gap. New data presented at CROI 2026 reveals that one in seven men living with HIV in the region are unaware of their status – a significantly higher rate than women. This isn’t simply a matter of numbers; it represents a substantial obstacle to achieving global HIV eradication goals and underscores a systemic failure to engage men in prevention and treatment efforts.
- The Gender Disparity: Men are falling behind in HIV awareness, treatment initiation, and viral suppression compared to women in eastern and southern Africa.
- Mobility & Age as Key Factors: Younger men and those with more mobile lifestyles are particularly vulnerable to undiagnosed infection.
- 95-95-95 at Risk: Failure to address these gaps threatens the UNAIDS’ ambitious targets for ending the HIV epidemic.
This data isn’t appearing in a vacuum. For years, HIV prevention and treatment programs have rightly focused on women, who historically bear a disproportionate burden of infection and face greater societal barriers to healthcare access. While this focus has yielded significant progress – evidenced by the 83% viral suppression rate among women on treatment – it has inadvertently created a blind spot regarding men’s health. The research highlights that men not only start the HIV care continuum at a lower point but also experience larger drop-offs at each stage, from testing to treatment to sustained viral suppression. This suggests that existing interventions are not effectively reaching or retaining men.
The study’s focus on overlapping vulnerabilities – age, mobility, and sexual behaviors – is particularly insightful. Mobility, often linked to economic opportunities or migration, disrupts consistent access to healthcare. Younger men may be less likely to perceive themselves at risk or engage with traditional healthcare systems. Understanding these intersections is crucial for designing targeted interventions.
The Forward Look: The next 12-18 months will be pivotal. We can expect to see a shift in funding and program design towards more gender-responsive HIV strategies. Specifically, look for:
- Community-Based Testing: Increased investment in mobile testing units and outreach programs tailored to reach men in non-traditional healthcare settings (workplaces, bars, community events).
- Male-Focused Messaging: Public health campaigns that directly address men’s concerns and challenge harmful gender norms surrounding HIV and healthcare seeking. This will require moving beyond simply adapting women-focused messaging.
- Integration with Existing Services: Leveraging existing male-focused health programs (e.g., those addressing prostate cancer or occupational health) to integrate HIV testing and prevention services.
- Further Research: Deeper qualitative research to understand the specific barriers men face in accessing HIV care, and to co-design solutions with the communities most affected.
The UNAIDS 95:95:95 targets are ambitious, but achievable. However, achieving them requires a fundamental re-evaluation of how we approach HIV prevention and treatment, and a renewed commitment to engaging men as equal partners in the fight against this epidemic.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.