Cervical cancer screening is on the cusp of a significant accessibility upgrade, potentially saving lives and addressing long-standing health inequities. A new study from the University of Sheffield reveals strong patient preference for at-home HPV self-sampling kits, particularly among physically disabled women who face disproportionate barriers to traditional screenings. This isn’t simply about convenience; it’s about dismantling systemic obstacles to healthcare access and recognizing patient autonomy.
- Key Finding: 63% of physically disabled women surveyed could perform the self-test, and over half would *prefer* it to an in-person screening.
- Critical Need: Over 70% expressed concerns about performing the test correctly, highlighting the need for clear, tailored instructions.
- NHS Context: The study coincides with the NHS’s planned expansion of at-home HPV testing, though current plans don’t specifically target disabled women.
Addressing a Long-Ignored Gap in Healthcare
Cervical cancer, largely preventable through screening, remains a significant health concern. The standard “smear test” – while effective – inherently presents challenges for individuals with physical disabilities. These range from logistical hurdles like transportation and accessible facilities to the physical difficulty of positioning for the procedure. The study underscores that these aren’t minor inconveniences; they represent substantial barriers that contribute to lower screening rates and, consequently, poorer health outcomes. This research arrives at a crucial moment, as healthcare systems globally are increasingly focused on equitable access and patient-centered care. The rise of self-sampling technologies, initially driven by pandemic-related disruptions to healthcare, is now proving to be a powerful tool for addressing pre-existing inequalities.
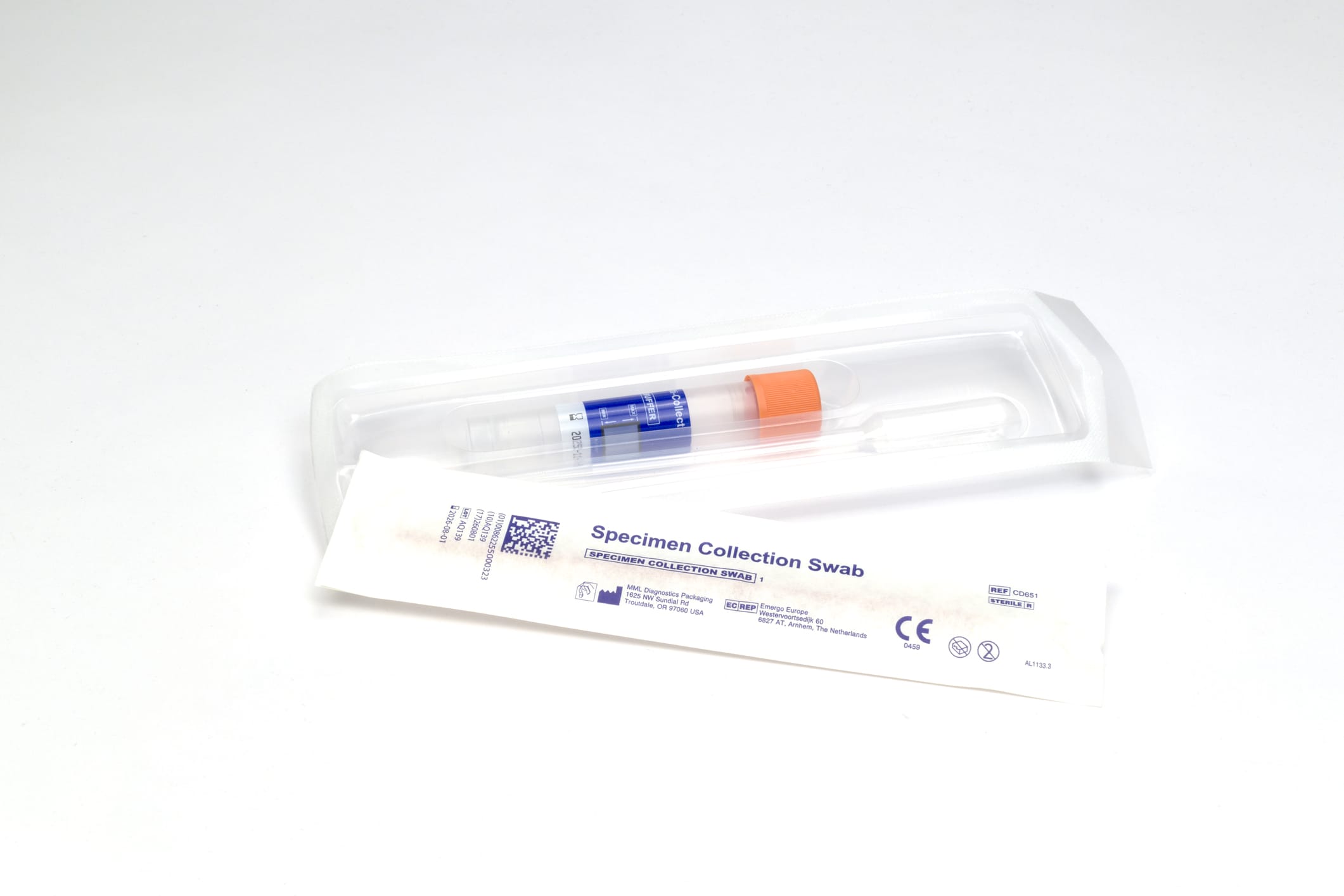
The simplicity of the vaginal swab used in these kits – described as similar to a cotton bud – is key. It removes the need for a clinician to administer the test, bypassing many of the structural obstacles disabled women routinely encounter. However, the study’s finding that over 70% of respondents had concerns about correct test administration is a critical point. This isn’t a reason to dismiss self-sampling, but rather a clear signal that implementation *must* prioritize comprehensive, accessible educational materials and clinician support.
The Forward Look: Beyond Pilot Programs – Towards Systemic Change
The NHS rollout of at-home HPV testing is a positive step, but the current lack of specific provisions for physically disabled women represents a missed opportunity. The data from the University of Sheffield study provides a compelling argument for extending the program to proactively offer self-sampling kits to this population. However, simply making the kits available isn’t enough.
What to watch for: Expect increased advocacy from patient groups and disability rights organizations pushing for targeted outreach and tailored support. Clinician training will be paramount. Healthcare providers need to be equipped to address patient concerns, provide clear instructions (potentially in multiple formats – video, large print, etc.), and offer assistance where needed. Furthermore, the success of this initiative will likely fuel broader discussions about expanding self-sampling options for other underserved populations facing barriers to traditional screenings, such as those in rural areas or with limited mobility. The future of cervical cancer screening isn’t just about new technology; it’s about a fundamental shift towards a more inclusive and equitable healthcare system.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.