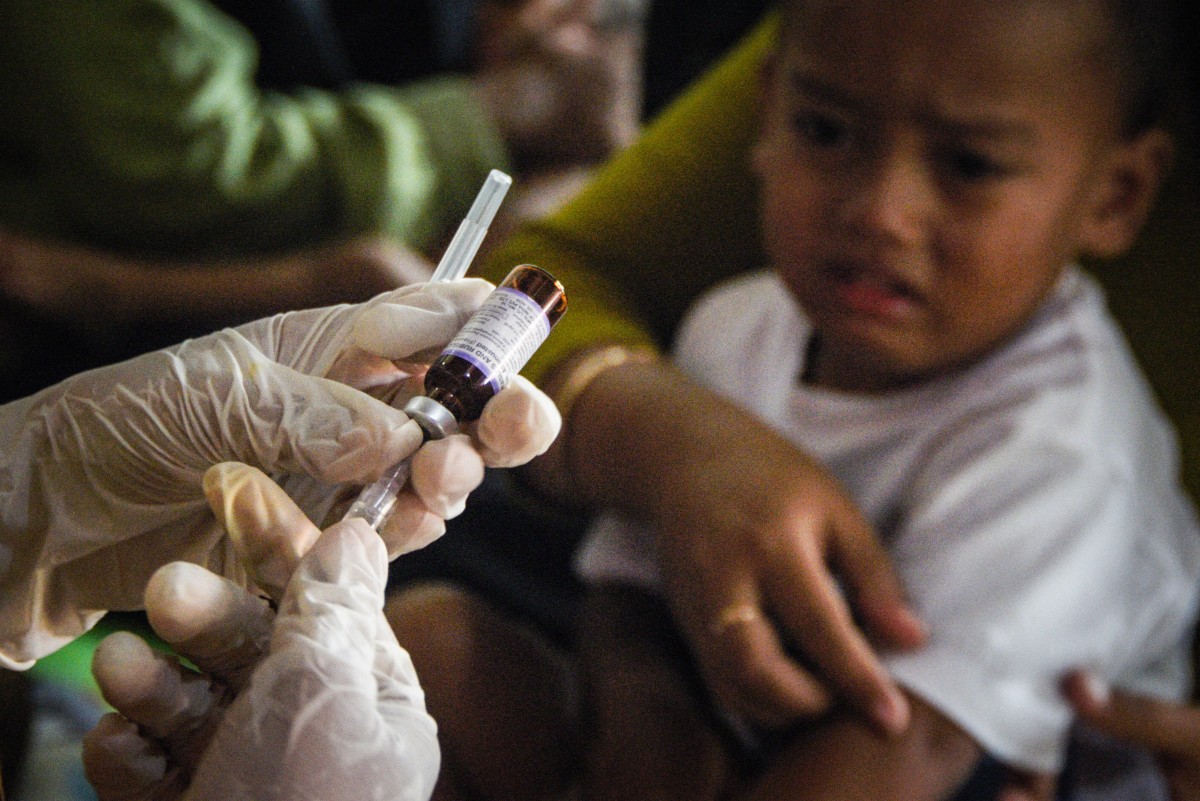
The Trust Deficit: How Vaccine Hesitancy in Indonesia Signals a Global Public Health Shift
We are currently witnessing a dangerous paradox: as medical technology reaches its zenith, the willingness to utilize it is plummeting. The recent surge in vaccine hesitancy in Indonesia is not merely a local health glitch; it is a loud alarm bell signaling a systemic collapse of trust in institutional authority that threatens to undo decades of progress in global childhood immunization.
The Return of the Preventable: The Measles Warning
The current warnings of a highly contagious measles outbreak in Indonesia serve as a visceral reminder that “eradicated” diseases are never truly gone—they simply wait for a gap in the armor of herd immunity. When vaccination rates dip below the critical threshold, the result is an inevitable resurgence of pathogens that the world had largely forgotten.
Measles is a sentinel species for public health. Because it is so incredibly contagious, it is often the first disease to return when immunization efforts falter. This outbreak is a symptom of a deeper pathology: the erosion of the social contract between the citizen and the state’s healthcare apparatus.
The Anatomy of Mistrust: Why Now?
The rise of anti-vaccination sentiment is rarely about the science of the vaccine itself; it is about the source of the information. In an era of algorithmic echo chambers, misinformation travels faster than any virus. For many, the suspicion directed toward vaccines is a proxy for a broader distrust of government efficiency and transparency.
When public trust is fractured, a simple health recommendation is no longer seen as medical advice—it is viewed as a mandate from an untrusted entity. This psychological shift transforms a routine pediatric visit into a political statement, leaving millions of children vulnerable to preventable tragedies.
Bridging the Gap: From Mandates to Meaning
The call from the MPR Deputy Speaker for the government to boost public trust is a necessary first step, but traditional “top-down” communication is no longer sufficient. The era of the government expert speaking from a podium to a passive audience is over. To combat vaccine hesitancy in Indonesia, the strategy must shift toward hyper-local advocacy.
Future success lies in the “last mile” of communication. This means empowering community leaders, religious figures, and local healers—the people parents actually trust—to become the primary conduits of scientific truth. Trust is not built through brochures; it is built through existing relationships.
Comparative Strategy: The Evolution of Public Health Outreach
| Feature | Traditional Approach (Failing) | Future Approach (Necessary) |
|---|---|---|
| Communication Flow | Top-Down / Centralized | Peer-to-Peer / Decentralized |
| Primary Driver | Authority & Mandates | Empathy & Community Trust |
| Information Channel | Mass Media / Government Ads | Micro-Influencers / Local Leaders |
| Goal | Compliance | Confidence |
The Ripple Effect: What Comes Next?
If this trend is not reversed, we are looking at more than just a measles spike. We are looking at a “syndemic” where vaccine-preventable diseases overlap with existing health crises, straining an already burdened healthcare infrastructure. The risk extends beyond Indonesia; this blueprint of hesitancy is being mirrored in other emerging economies, creating a global patchwork of vulnerability.
However, there is an opportunity here to redefine public health. By treating vaccine hesitancy as a sociological challenge rather than a medical one, governments can rebuild a more resilient, transparent, and inclusive healthcare system. The goal is not just to increase vaccination numbers, but to restore the fundamental belief that the system cares for the individual.
The fight against infectious diseases is no longer just a battle of biology and chemistry; it is a battle of narratives. The winners will not be those with the best vaccines, but those who can most effectively restore the human connection between the provider and the patient.
Frequently Asked Questions About Vaccine Hesitancy in Indonesia
What is driving the rise of vaccine hesitancy in Indonesia?
It is a complex mix of health misinformation spread via social media, cultural suspicions, and a broader decline in trust toward government institutions.
How does a measles outbreak relate to vaccination rates?
Measles requires a very high percentage of the population (roughly 95%) to be immune to prevent outbreaks. When hesitancy causes rates to drop, the virus quickly finds gaps in the population to spread rapidly.
Can government mandates solve the problem of vaccine distrust?
While mandates can increase short-term numbers, they often deepen long-term distrust. The most sustainable solution is building community-led confidence and improving transparent communication.
What are the long-term risks of declining childhood immunization?
Beyond immediate outbreaks, declining rates can lead to the return of diseases like polio or rubella, causing permanent disability or death in children and increasing overall healthcare costs for the state.
What are your predictions for the future of global public health trust? Do you believe community-led advocacy can outweigh the influence of digital misinformation? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.