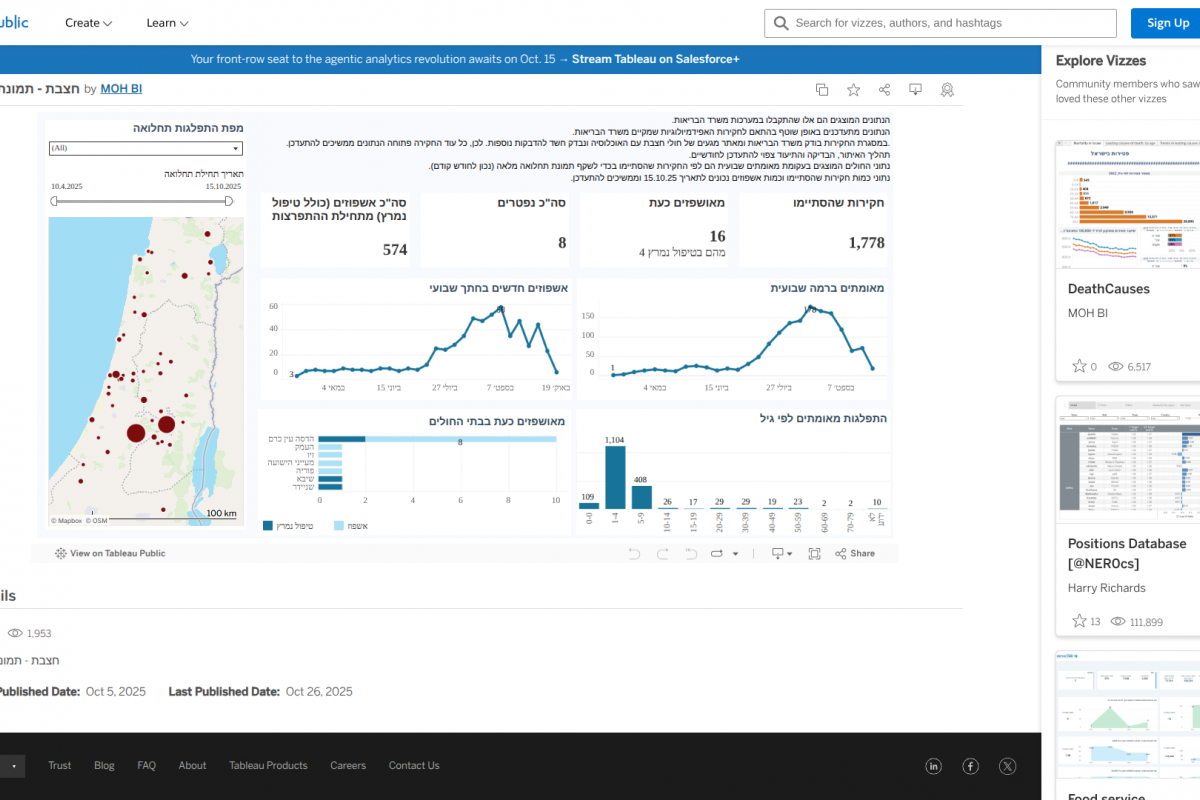
A chilling statistic: eight infants in Israel have succumbed to measles in the first half of 2025. This isn’t an isolated incident; it’s a stark warning. Beyond the immediate tragedy, this outbreak, coupled with 17 hospitalizations and five patients in intensive care, foreshadows a potentially widespread erosion of herd immunity and a future where preventable diseases make a devastating comeback. The situation demands a critical examination of not just vaccination rates, but the systemic vulnerabilities that allow these outbreaks to flourish.
The Anatomy of a Resurgence: What’s Driving the Rise in Measles?
The current outbreak in Israel isn’t simply a matter of isolated cases. It’s a complex interplay of factors, including declining vaccination rates, particularly within specific communities. While official figures are still being compiled, anecdotal evidence suggests vaccine hesitancy, fueled by misinformation and distrust in public health institutions, is a significant contributor. However, focusing solely on hesitancy overlooks crucial systemic issues. Access to healthcare, particularly in underserved populations, and the logistical challenges of maintaining consistent vaccination schedules also play a role.
Beyond Israel: A Global Pattern Emerges
Israel’s experience is mirroring trends observed globally. The World Health Organization (WHO) has repeatedly warned of a resurgence in measles cases worldwide, with several European countries and parts of Africa experiencing significant outbreaks. This isn’t a coincidence. A confluence of factors – pandemic-related disruptions to routine immunization programs, increasing anti-vaccine sentiment amplified by social media, and geopolitical instability hindering access to healthcare – are creating a perfect storm for the re-emergence of this highly contagious disease. The term **measles resurgence** is no longer a hypothetical threat; it’s a present reality.
The Future of Immunization: Proactive Strategies for a Changing World
Addressing this challenge requires a paradigm shift in how we approach immunization. Reactive measures – responding to outbreaks after they occur – are no longer sufficient. We need proactive, multi-faceted strategies that address the root causes of declining vaccination rates and build more resilient public health systems.
Leveraging Technology for Enhanced Vaccine Delivery
One promising avenue is the use of technology to improve vaccine delivery and tracking. Digital immunization records, accessible via smartphones, can streamline the vaccination process and ensure individuals are up-to-date on their immunizations. Artificial intelligence (AI) can be used to identify communities at high risk of outbreaks and target vaccination campaigns accordingly. Furthermore, telehealth platforms can provide remote consultations and address vaccine hesitancy by offering personalized information and addressing individual concerns.
Combating Misinformation: A Public Health Imperative
The spread of misinformation about vaccines is a major obstacle to achieving herd immunity. Combating this requires a coordinated effort from public health agencies, social media platforms, and trusted community leaders. Fact-checking initiatives, educational campaigns, and transparent communication about vaccine safety and efficacy are crucial. However, simply debunking myths isn’t enough. We need to understand the underlying reasons why people are hesitant to vaccinate and address their concerns with empathy and respect.
The Role of Personalized Immunization Schedules
The traditional “one-size-fits-all” approach to immunization may not be optimal for everyone. Emerging research suggests that individual immune responses to vaccines can vary based on factors such as age, genetics, and underlying health conditions. In the future, we may see the development of personalized immunization schedules tailored to an individual’s specific needs, maximizing vaccine efficacy and minimizing the risk of adverse events.
The measles outbreak in Israel serves as a critical wake-up call. It’s a reminder that the gains made in controlling infectious diseases are not guaranteed and that complacency can have devastating consequences. The future of immunization hinges on our ability to adapt to a changing world, embrace innovative technologies, and build trust in public health institutions.
Frequently Asked Questions About Measles and Immunization
What is herd immunity and why is it important?
Herd immunity occurs when a large percentage of a population is immune to a disease, either through vaccination or prior infection. This protects those who are unable to be vaccinated, such as infants or individuals with compromised immune systems. When vaccination rates decline, herd immunity is compromised, increasing the risk of outbreaks.
How effective is the measles vaccine?
The measles, mumps, and rubella (MMR) vaccine is highly effective. Two doses of the MMR vaccine provide approximately 97% protection against measles. However, even with high vaccination rates, outbreaks can still occur in communities with pockets of unvaccinated individuals.
What can I do to protect myself and my family from measles?
The most effective way to protect yourself and your family from measles is to get vaccinated with the MMR vaccine. Ensure that you and your children are up-to-date on your immunizations. If you are traveling to an area with a measles outbreak, consult with your doctor about getting vaccinated or receiving a booster dose.
What are your predictions for the future of measles prevention? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.