The landscape of psoriasis treatment is shifting, with emerging data suggesting a path towards not just symptom management, but potential long-term disease modification. New analyses of bimekizumab, a relatively recent entrant into the IL-17 inhibitor class, demonstrate sustained skin clearance for up to four years in a significant proportion of patients – a finding that addresses a critical unmet need in chronic psoriasis care. This isn’t simply about better symptom control; it’s about understanding *how* the drug is impacting the underlying immune mechanisms driving the disease, and what that means for the future of treatment strategies.
- Unprecedented Durability: 73.0% of patients achieving complete skin clearance with bimekizumab maintained that response at Year 4.
- Targeting Immune Memory: Research identifies and normalizes pathogenic tissue-resident memory T (TRM) cells, suggesting a deeper mechanism than simple inflammation suppression.
- Shifting Treatment Paradigm: The data supports a move towards disease modification, offering hope for sustained remission and potentially reducing the long-term burden of psoriasis.
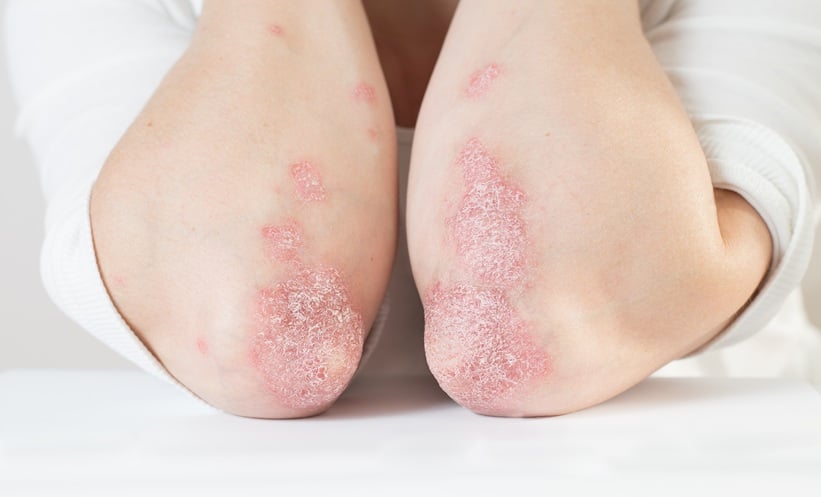
Psoriasis affects approximately 2-3% of the global adult population, manifesting as chronic, inflammatory skin lesions. While existing biologic therapies targeting the IL-17 pathway have dramatically improved short-term control, the question of long-term durability has remained a significant challenge. Many patients experience a waning of response over time, necessitating treatment adjustments or switches. The current standard of care often involves a cycle of escalation and adaptation, highlighting the need for therapies that can provide sustained benefit. Bimekizumab distinguishes itself by simultaneously inhibiting both IL-17A and IL-17F, a dual-targeting approach designed to achieve more comprehensive immune modulation. Previous IL-17A inhibitors showed promise, but the persistence of disease in some patients hinted at the involvement of IL-17F, prompting the development of agents like bimekizumab.
The key breakthrough revealed in this research isn’t just the extended period of skin clearance, but the mechanistic insight into *why* it’s happening. Researchers identified a specific population of tissue-resident memory T (TRM) cells within psoriatic lesions, expressing IL-17A and/or IL-17F, and crucially, exhibiting pro-survival factors. These cells essentially act as a reservoir of inflammation, contributing to disease relapse. Bimekizumab appears to not only suppress inflammation but also to reverse the expression of these pro-survival genes within these TRM cells, effectively normalizing their function. This suggests a more fundamental alteration of the immune response, rather than a temporary suppression of symptoms.
The Forward Look
This research positions bimekizumab as a potential frontrunner in the next generation of psoriasis treatments. However, several key areas require further investigation. The current data relies on patients who achieved early clearance and continued therapy, raising questions about efficacy in broader, more diverse populations, including those with more severe disease or those who haven’t responded to previous treatments. Future studies will need to explore the drug’s effectiveness in these challenging patient groups. Furthermore, identifying other cell types expressing IL-17A and IL-17F will be crucial for a more complete understanding of the drug’s mechanism of action and potential for broader application in other IL-17 driven inflammatory conditions. We can anticipate a surge in research focused on TRM cells and their role in chronic inflammatory diseases, potentially opening up new therapeutic avenues beyond psoriasis. Clinically, expect to see increased utilization of bimekizumab, particularly in patients seeking long-term disease control, and a shift in patient-physician conversations towards the possibility of sustained remission rather than simply managing flares. The publication of the full data in the Journal of Allergy and Clinical Immunology (DOI:10.1016/j.jaci.2025.12.1013) will undoubtedly fuel further scrutiny and discussion within the dermatology community.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.