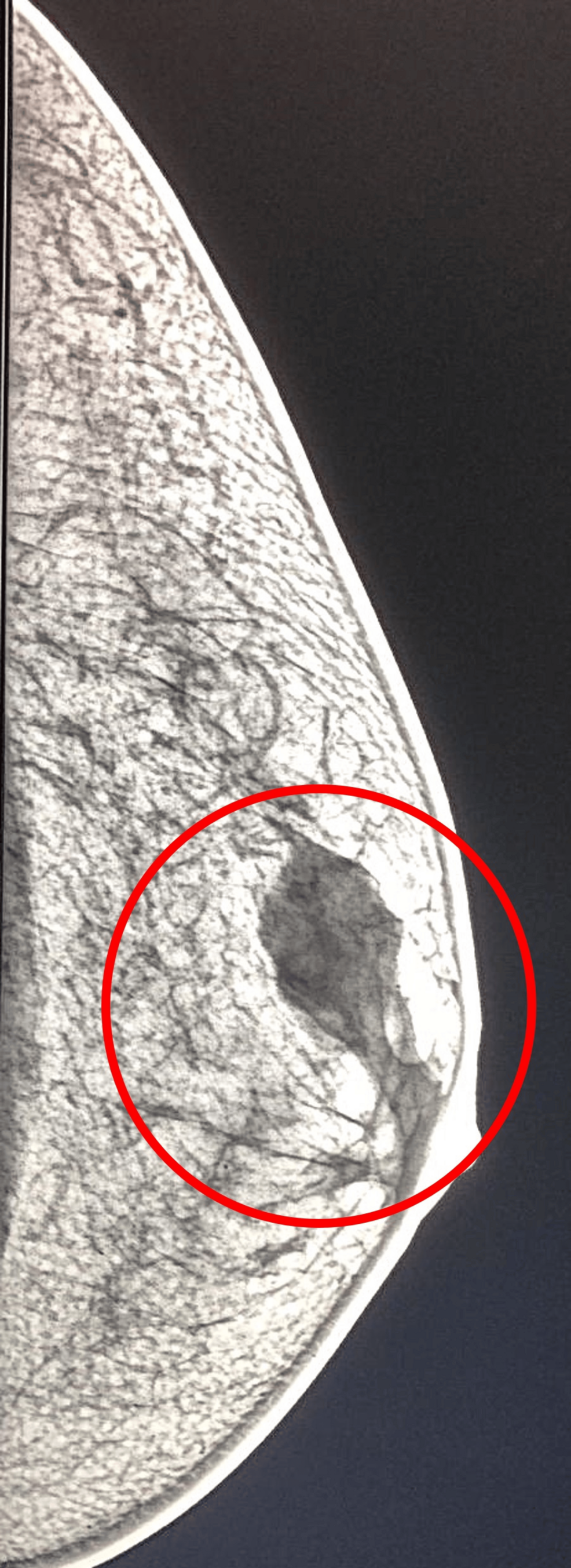
Less than 1% of all breast cancer cases occur in men, yet that statistic masks a critical reality: when diagnosed at later stages, male breast cancer carries a significantly worse prognosis than in women. For decades, awareness campaigns have focused primarily on female populations, leaving men in the dark about their own risk and potential symptoms. But a shift is underway, driven by advancements in genetic screening, liquid biopsies, and a growing understanding of the unique biological factors influencing the disease in men. Male breast cancer is no longer a neglected corner of oncology; it’s entering an era of precision medicine.
The Diagnostic Gap: Why Early Detection Matters
The sources highlight a consistent theme: delayed diagnosis. Men often dismiss symptoms like a lump, nipple retraction, or skin changes as insignificant, or simply aren’t aware that these can be indicators of breast cancer. This delay is compounded by a lack of routine screening for men, unlike the mammograms routinely offered to women. The Cureus case report underscores this point, detailing a patient whose diagnosis was significantly delayed due to a lack of suspicion. This isn’t simply a matter of individual awareness; it’s a systemic issue requiring a proactive approach to male health education.
Genetic Predisposition and the BRCA1/2 Connection
While most male breast cancers are sporadic, a significant proportion – estimated between 5-10% – are linked to inherited genetic mutations, most notably in the BRCA1 and BRCA2 genes. These genes, more commonly associated with ovarian and female breast cancer, play a crucial role in DNA repair. Mutations increase the risk not only of breast cancer but also of prostate, pancreatic, and melanoma. However, genetic testing for these mutations in men presenting with breast cancer, or those with a strong family history, remains underutilized. Future trends point towards broader genetic screening panels, incorporating not just BRCA1/2 but also other genes implicated in breast cancer development, like TP53 and PTEN.
Beyond the Lump: Emerging Diagnostic Technologies
Traditional diagnostic methods rely heavily on physical examination and imaging, such as mammograms and ultrasounds. While effective, these methods can sometimes miss subtle changes, particularly in men with dense chest tissue. The future of male breast cancer diagnosis lies in more sophisticated technologies:
- Liquid Biopsies: These blood tests detect circulating tumor cells (CTCs) or circulating tumor DNA (ctDNA) shed by cancer cells. Liquid biopsies offer a non-invasive way to detect cancer early, monitor treatment response, and identify genetic mutations driving the disease.
- Advanced Imaging: Techniques like contrast-enhanced mammography and breast MRI are becoming increasingly sensitive and specific, offering improved detection rates, especially in high-risk individuals.
- Artificial Intelligence (AI) Assisted Diagnosis: AI algorithms are being trained to analyze medical images with greater accuracy and speed than human radiologists, potentially reducing false positives and improving early detection.
Personalized Treatment Strategies: Tailoring Therapy to the Individual
Historically, treatment for male breast cancer has largely mirrored that for women, involving surgery, radiation therapy, and chemotherapy. However, emerging research suggests that male breast cancers often exhibit different molecular characteristics than those in women, necessitating a more personalized approach. For example, male breast cancers are more likely to be hormone receptor-positive (ER+/PR+) and HER2-negative. This means that hormone therapy, such as tamoxifen or aromatase inhibitors, may be particularly effective. Furthermore, the identification of specific genetic mutations can guide the use of targeted therapies, such as PARP inhibitors for BRCA-mutated cancers.
The Times of India article rightly emphasizes preventative measures, but prevention extends beyond self-examination. Maintaining a healthy weight, limiting alcohol consumption, and regular exercise are all important lifestyle factors that can reduce cancer risk. However, for men with a strong family history or known genetic mutations, proactive surveillance and preventative strategies, such as prophylactic mastectomy, may be considered.
| Diagnostic/Treatment Area | Current Standard | Future Projection (5-10 years) |
|---|---|---|
| Genetic Screening | BRCA1/2 testing for high-risk individuals | Expanded multi-gene panels; population-based screening for specific mutations |
| Early Detection | Physical exam, Ultrasound/Mammography | Widespread adoption of liquid biopsies; AI-assisted image analysis |
| Treatment | Surgery, Chemotherapy, Radiation, Hormone Therapy | Personalized therapies based on genomic profiling; targeted drug delivery systems |
The future of male breast cancer care isn’t just about earlier detection; it’s about a fundamental shift towards precision medicine, where treatment is tailored to the unique characteristics of each patient’s tumor. This requires a collaborative effort between clinicians, researchers, and patients, driven by a commitment to raising awareness and breaking down the stigma surrounding this often-overlooked disease.
Frequently Asked Questions About Male Breast Cancer
What are the biggest challenges in diagnosing male breast cancer?
The primary challenges are low awareness among both men and healthcare providers, leading to delayed presentation and diagnosis. Men may not recognize symptoms as potentially cancerous, and doctors may not consider breast cancer as a possibility in male patients.
How does genetic testing impact treatment decisions?
Identifying genetic mutations, such as in BRCA1/2, can guide the use of targeted therapies like PARP inhibitors. It also informs family screening and preventative measures for at-risk relatives.
What role will liquid biopsies play in the future of male breast cancer care?
Liquid biopsies offer a non-invasive way to detect cancer early, monitor treatment response, and identify genetic mutations. They have the potential to revolutionize surveillance and personalized treatment strategies.
Are there any lifestyle changes men can make to reduce their risk?
Maintaining a healthy weight, limiting alcohol consumption, engaging in regular exercise, and being aware of family history are all important steps men can take to reduce their risk of developing breast cancer.
What are your predictions for the future of male breast cancer diagnosis and treatment? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.