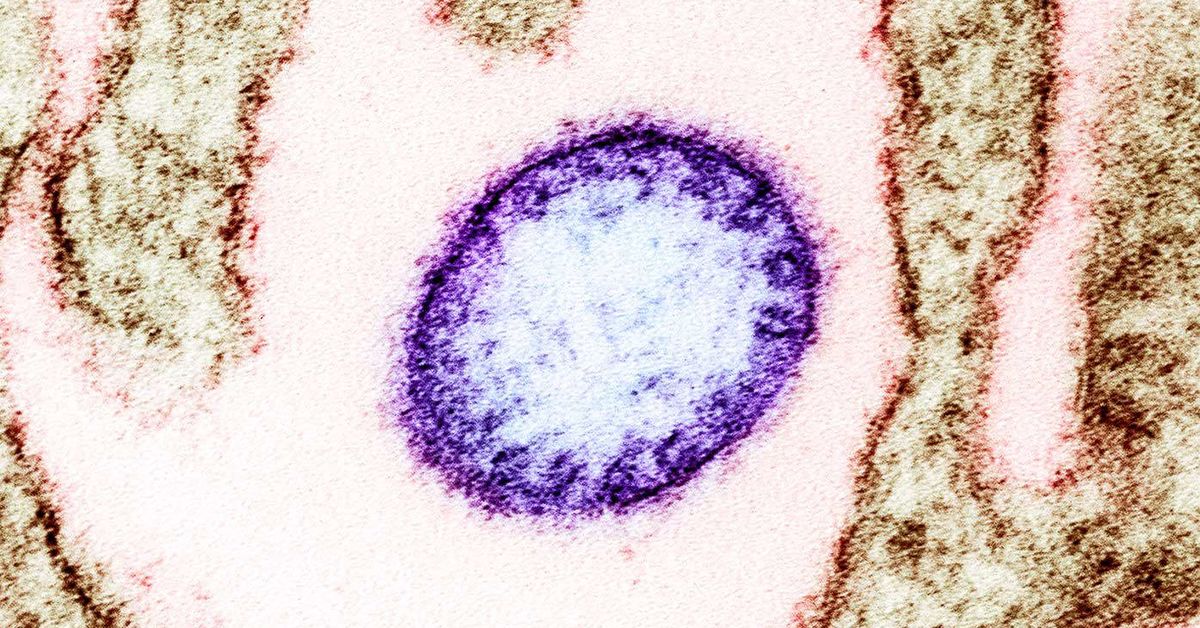
Nipah Virus: Beyond Outbreaks – The Looming Threat of Zoonotic Spillover and Pandemic Preparedness
A chilling statistic: over 60% of emerging infectious diseases originate in animals. The recent confirmation of Nipah virus cases in India, triggering airport screenings across Asia, isn’t an isolated incident. It’s a stark warning about the escalating threat of zoonotic spillover – the transmission of pathogens from animals to humans – and a critical test of global pandemic preparedness. While headlines focus on immediate containment, the long-term implications demand a far more proactive and systemic response.
The Nipah Virus: A Deep Dive into the Current Threat
Nipah virus (NiV) is a bat-borne virus that can also be transmitted through contaminated food, or direct contact with infected pigs or humans. First identified in Malaysia in 1998, it causes a range of symptoms, from respiratory illness and encephalitis (brain inflammation) to seizures and coma. The fatality rate is alarmingly high, ranging from 40% to 75%, depending on the outbreak and access to intensive care. Current cases in India, while limited in number, are a potent reminder of the virus’s potential for rapid spread, particularly in densely populated areas.
Understanding the Transmission Dynamics
The primary reservoir for NiV is fruit bats, specifically Pteropus species. However, the virus doesn’t directly jump from bats to humans frequently. Intermediate hosts, like pigs in the 1998 Malaysian outbreak, amplify the virus and increase the risk of human infection. In India, consumption of contaminated date palm sap is suspected as a key transmission route. This highlights the complex interplay between environmental factors, human behavior, and viral evolution.
The Future of Zoonotic Spillover: A Perfect Storm
The emergence of Nipah virus isn’t a random event. It’s a consequence of several converging trends. Deforestation and habitat loss are forcing wildlife into closer contact with human populations, increasing the opportunities for spillover. Climate change is altering species distributions, potentially bringing bats – and the viruses they carry – into new regions. Intensive farming practices and the wildlife trade further exacerbate the risk, creating ideal conditions for viral amplification and spread.
Consider this: the global wildlife trade is a multi-billion dollar industry, often operating with minimal regulation. This creates a network for the rapid dissemination of pathogens across borders. Furthermore, the increasing demand for bushmeat in some regions puts immense pressure on wildlife populations, driving them closer to human settlements.
Beyond Nipah: The Broader Landscape of Emerging Zoonoses
Nipah virus is just one piece of a much larger puzzle. Other zoonotic viruses, like Ebola, Zika, and SARS-CoV-2, have demonstrated the devastating potential of these events. The scientific community is increasingly focused on identifying “hotspots” – regions where the risk of spillover is particularly high – and developing predictive models to anticipate future outbreaks. However, prediction is only half the battle. Effective prevention requires a multi-faceted approach.
| Zoonotic Virus | Origin | Key Transmission Route | Estimated Fatality Rate |
|---|---|---|---|
| Nipah Virus | Bats | Contaminated food, animal contact | 40-75% |
| Ebola Virus | Bats | Direct contact with infected fluids | 25-90% |
| SARS-CoV-2 | Likely Bats (via intermediate host) | Respiratory droplets | ~3.4% (globally) |
Investing in Pandemic Preparedness: A Global Imperative
The COVID-19 pandemic exposed critical weaknesses in global pandemic preparedness. Insufficient investment in surveillance systems, inadequate diagnostic capacity, and a lack of coordinated international response hampered efforts to contain the virus. The lessons learned must be applied to address the threat of future zoonotic outbreaks. This includes:
- Strengthening Surveillance: Expanding wildlife surveillance programs to identify novel pathogens and track their spread.
- Investing in Diagnostics: Developing rapid and accurate diagnostic tests for emerging viruses.
- Building Healthcare Capacity: Improving healthcare infrastructure and training healthcare workers to respond to outbreaks.
- Promoting One Health: Adopting a “One Health” approach that recognizes the interconnectedness of human, animal, and environmental health.
- Addressing Environmental Drivers: Tackling deforestation, climate change, and the wildlife trade to reduce the risk of spillover.
Frequently Asked Questions About Nipah Virus and Zoonotic Diseases
What can individuals do to protect themselves from Nipah virus?
Avoid consuming raw date palm sap, especially in areas where outbreaks have been reported. Practice good hygiene, including frequent handwashing, and avoid close contact with sick animals or people.
Is a Nipah virus vaccine likely in the near future?
Research into a Nipah virus vaccine is ongoing, but a widely available vaccine is still several years away. Current treatment focuses on supportive care to manage symptoms.
How does climate change contribute to the risk of zoonotic diseases?
Climate change alters species distributions, forcing animals to migrate and increasing contact with humans. It also weakens animal immune systems, making them more susceptible to infection.
What is the “One Health” approach?
The “One Health” approach recognizes that the health of humans, animals, and the environment are interconnected. It emphasizes collaboration between different disciplines to address health challenges.
The Nipah virus outbreaks serve as a critical wake-up call. The threat of zoonotic spillover is not a distant possibility; it’s a present and growing danger. Investing in proactive surveillance, robust pandemic preparedness, and addressing the underlying environmental drivers is not just a matter of public health – it’s a matter of global security. What are your predictions for the future of zoonotic disease control? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.