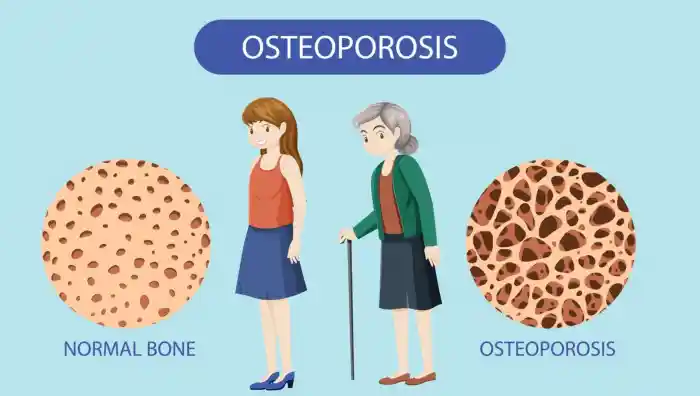
Beyond the Brittle Bone: The Future of Precision Health and Osteoporosis in Women
For decades, we have treated bone loss as an inevitable tax on aging—a biological certainty for women as they navigate the transition of menopause. However, viewing osteoporosis in women as an unavoidable destiny is not only outdated; it is a dangerous medical narrative that leads millions to ignore early warning signs until a catastrophic fracture occurs.
The reality is that the “silent thief” of bone density doesn’t always start with a break. It often begins with a dull ache in the knee or a slight stiffness in the joints—symptoms that are frequently dismissed as “just part of getting older” or a result of a busy lifestyle. When we ignore these signals, we aren’t just tolerating discomfort; we are missing the critical window for preventative intervention.
The Gender Gap in Musculoskeletal Vulnerability
Medical data consistently confirms that women are significantly more susceptible to bone density loss than men. This isn’t merely a matter of frame size, but a complex interplay of hormonal shifts. The drop in estrogen during menopause accelerates bone resorption, meaning the body breaks down bone faster than it can rebuild it.
Yet, a more insidious problem exists: the psychological normalization of pain. Women are more likely to ignore chronic joint pain or knee instability, attributing it to daily stress or domestic labor. This cognitive gap between feeling pain and seeking professional diagnosis creates a dangerous lag in treatment.
The Danger of the “Normal Pain” Narrative
Chronic knee pain is rarely just about the joint itself. In many cases, it serves as a canary in the coal mine for the entire musculoskeletal system. When joint mobility decreases, the mechanical load on the bones shifts, often exacerbating existing weaknesses in bone structure.
Ignoring these early indicators of joint decay often leads to a cascade of mobility issues. Once mobility is compromised, the lack of weight-bearing exercise further accelerates bone loss, creating a feedback loop that culminates in severe osteoporosis.
The Shift Toward Precision Prevention
We are currently witnessing a paradigm shift in how we approach bone health. The future is moving away from generic calcium supplements and toward “Precision Prevention”—a personalized approach to musculoskeletal longevity.
Nutrigenomics and Bone Density
Rather than a one-size-fits-all vitamin regimen, the next frontier is nutrigenomics. By analyzing an individual’s genetic markers, clinicians can now determine exactly how a woman’s body absorbs minerals and responds to Vitamin D, allowing for bespoke nutritional protocols that optimize bone mineralization based on DNA.
AI-Driven Early Detection
The future of screening lies in AI-enhanced imaging. Traditional DEXA scans provide a snapshot, but emerging AI tools can analyze subtle changes in bone architecture and joint alignment long before bone density drops to critical levels. This allows for “pre-habilitation”—intervening while the bone is still salvageable.
| Feature | Traditional Reactive Care | Future Precision Prevention |
|---|---|---|
| Detection | Post-fracture or scheduled DEXA | AI-driven continuous monitoring |
| Nutrition | Generic Calcium/Vitamin D | DNA-based Nutrigenomics |
| Approach | Managing the disease | Optimizing bone architecture |
| Goal | Preventing the next break | Maintaining lifelong mobility |
Integrating Holistic Mobility into Longevity
True bone health cannot exist in a vacuum. The synergy between muscular strength and bone density is absolute. The emerging trend of “functional longevity” emphasizes that strength training is not about aesthetics, but about creating a mechanical shield for the skeleton.
By integrating high-impact resistance training with regenerative therapies, women can effectively “signal” their bones to increase density. The goal is no longer just to avoid a fracture, but to maintain an athletic, mobile frame well into the eighth and ninth decades of life.
Frequently Asked Questions About the Future of Bone Health
Is osteoporosis in women completely preventable?
While genetics play a role, the majority of bone loss can be mitigated through early intervention, precision nutrition, and targeted weight-bearing exercise, moving the focus from “cure” to “prevention.”
Can simple knee pain actually be a sign of osteoporosis?
Yes. While knee pain can be caused by many things, chronic joint instability often correlates with systemic musculoskeletal weakness, which can be an early indicator of declining bone health.
How does AI improve the detection of bone loss?
AI can detect micro-architectural changes in bone structure that the human eye might miss on a standard scan, allowing doctors to treat patients years before they reach the osteoporosis threshold.
The era of accepting bone fragility as a feminine certainty is over. By shifting our perspective from treating fractures to optimizing bone architecture through technology and personalized medicine, we can redefine the aging process. The key lies in listening to the “whispers” of joint pain today to avoid the “screams” of a fracture tomorrow.
What are your predictions for the future of personalized health? Do you believe AI will eventually eliminate the risk of osteoporosis? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.