The Age of Insularity: How the Global Healthcare Trust Crisis is Redefining Patient Care
GENEVA — A staggering collapse in consumer confidence is fueling a global healthcare trust crisis, as a surplus of available medical information paradoxically leaves patients feeling less capable of making informed decisions.
New data from the 2026 Edelman Trust Barometer reveals that “information abundance” is no longer an asset. Instead, it has become a catalyst for confusion and insularity.
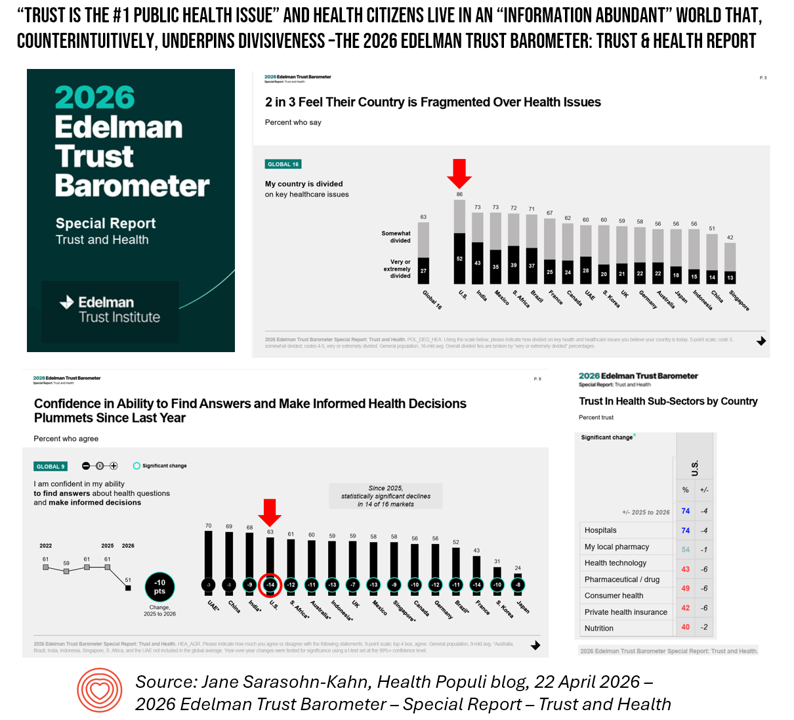
In the United States, confidence in the ability to find reliable health answers plummeted by 14 percentage points in a single year. This decline is among the steepest globally, matched only by France.
From Pandemic Shock to the ‘Age of Insularity’
The road to the current crisis was paved over the last five years. In 2022, the COVID-19 pandemic exposed deep structural failures in global health systems, leaving citizens feeling abandoned by the institutions designed to protect them.
By 2023, a generational shift occurred. Younger populations began viewing social media as a viable substitute for professional medical consultation, believing their digital research put them on a par with physicians.
This trend accelerated in 2024, as peers became as influential as scientists. By 2025, the “Year of Grievance,” trust localized; people began trusting their immediate neighbors more than national governments or mainstream media.
Now, in 2026, we have entered the “Age of Insularity.” The primary challenge for the medical community is no longer just fighting misinformation, but penetrating the closed loops of trust that patients have built around themselves.
The Trust Hierarchy: Who Still Holds the Key?
Despite the turmoil, the individual physician remains the most resilient anchor in the ecosystem. Globally, 80% of people still trust “my doctor” above all others.
Medical scientists follow at 73%, while friends and family hold a 64% trust rating. Interestingly, this outweighs the 61% who trust global health authorities like the World Health Organization.
However, this trust is highly compartmentalized. While doctors are the gold standard for diagnosis and acute treatment, they are losing ground in the “competitive clinical domain” of prevention.
When it comes to nutrition, vitamins, and supplements, patients are increasingly turning to AI, social media creators, and peers over licensed clinicians.
The Paradox of the ‘Super-Information Seeker’
One of the most counterintuitive findings of the 2026 report is the behavior of those with divisive health beliefs. People who hold views contrary to medical consensus—such as skepticism regarding water fluoridation or vaccine safety—actually consult more sources of information than those who trust the consensus.
This suggests that for a significant portion of the population, formal credentials are no longer the primary metric of truth. Instead, “relatability” and shared experience have become the new currency of credibility.
Do we trust the degree on the wall, or the person who has walked in our shoes? Is the abundance of data liberating the patient or simply isolating them in a digital echo chamber?
Strategic Pathways to Rebuilding Trust
To combat the healthcare trust crisis, a panel of global experts suggests a shift from “broadcasting” to “dialogue.”
Dr. Uché Blackstock, CEO of Advancing Health Equity, emphasizes the power of “small moments.” She argues that when patients bring self-researched data into the exam room, it should not be viewed as a challenge to authority, but as a symptom of gaps in access and connection.
Sreejit Mohan of Sanofi suggests that divisiveness does not actually cause disengagement; rather, it inspires a different kind of engagement. He calls for pharma and life science companies to stop “speechmaking” and start acting as guides and conveners.
Dr. Megan Ranney of the Yale School of Public Health identifies trust as the “number one public health crisis globally,” surpassing issues of nutrition or violence. Her solution? A “hyper-local” approach that integrates doulas, pharmacists, and community leaders into the care delivery model.
Finally, Dr. Garth Graham of Google/YouTube reminds practitioners that “no one likes to be spoken down to.” He posits that the most valuable credential a provider can possess is not a degree, but a demonstrated capacity for active listening.
By broadening the tent to include creators and community advocates, the medical establishment can move toward an “All of Society” approach to wellness.
Frequently Asked Questions
The crisis is driven by “information abundance,” where a surplus of conflicting health data leads to “insularity,” causing patients to trust hyper-local sources over national health institutions.
AI provides immediate, convenient answers, leading 66% of fluent AI users to believe the technology can handle certain health tasks as well as or better than a doctor.
Despite the decline in institutional trust, the personal physician remains the most trusted entity, with an 80% global trust rating.
The Age of Insularity refers to a trend where people move from polarization to complete isolation within trusted local circles, ignoring broader expert consensus.
Providers can rebuild trust through active listening, acknowledging patient-led research, and partnering with hyper-local community influencers.
Is the rise of AI-driven health advice a tool for empowerment or a risk to public safety? We want to hear your perspective.
Share this article with your network and join the conversation in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.