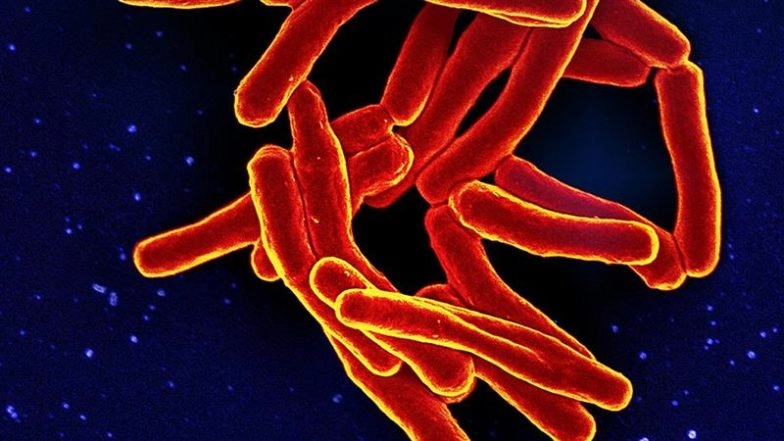
The resurgence of Tuberculosis (TB), now officially the world’s deadliest infectious disease as of 2023, isn’t merely a statistical blip – it’s a stark warning about the fragility of public health infrastructure and the cascading consequences of pandemic-era disruptions. While COVID-19 rightly dominated global attention, the focus diverted resources and expertise away from essential TB control programs, creating a breeding ground for this ancient foe to regain its foothold. The reported 10,260 cases in the US for 2025, a continuation of increases since 2020, represents a worrying reversal of decades of progress and underscores a systemic vulnerability we can no longer ignore.
- TB is Back: After a brief decline during the COVID-19 pandemic, TB has reclaimed its position as the world’s deadliest infectious disease.
- US Cases Rising: Provisional data shows a continued increase in TB cases in the US, with 10,260 reported in 2025.
- Drug Resistance Threat: Incomplete treatment and delayed diagnosis are fueling the rise of drug-resistant TB strains, complicating treatment and posing a broader public health risk.
The Deep Dive: Why Now?
Tuberculosis is a bacterial infection spread through the air, and its recent resurgence is multi-faceted. The COVID-19 pandemic significantly disrupted TB diagnosis and treatment programs globally. Lockdowns, overwhelmed healthcare systems, and redeployment of healthcare workers all contributed to delays in detection and treatment initiation. This created a backlog of undiagnosed cases and allowed the disease to spread silently within communities. Furthermore, the pandemic exacerbated existing risk factors for TB, such as poverty, malnutrition, and overcrowded living conditions. The similarity in initial symptoms – cough, fever, fatigue – between TB and COVID-19 also led to misdiagnosis and delayed appropriate care. The BCG vaccine, while common in many countries, isn’t routinely used in the US, leaving a larger proportion of the population susceptible. Crucially, the long and complex treatment regimen for TB – typically six to nine months of antibiotics – requires significant patient adherence, which is often compromised by socioeconomic factors and the potential for debilitating side effects.
The Forward Look: What Happens Next?
The current trajectory is deeply concerning, but not inevitable. We can expect to see increased investment in rapid diagnostic tools for TB, particularly those that can quickly identify drug-resistant strains. Public health campaigns will need to refocus on raising awareness of TB symptoms and emphasizing the importance of early testing, especially among vulnerable populations. However, the most critical need is a renewed commitment to strengthening public health infrastructure. This includes bolstering TB control programs, training healthcare workers, and addressing the social determinants of health that contribute to TB risk.
Looking ahead, the CDC will likely issue updated guidelines for TB screening and treatment, potentially expanding recommendations for preventative therapy among high-risk groups. We can also anticipate increased research into new TB vaccines and shorter, more effective treatment regimens. However, without a substantial and sustained investment in global TB control efforts, the threat of drug-resistant strains will continue to grow, potentially reversing decades of progress and jeopardizing global health security. The rise of TB serves as a potent reminder that neglecting one infectious disease can have far-reaching and devastating consequences for all.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.