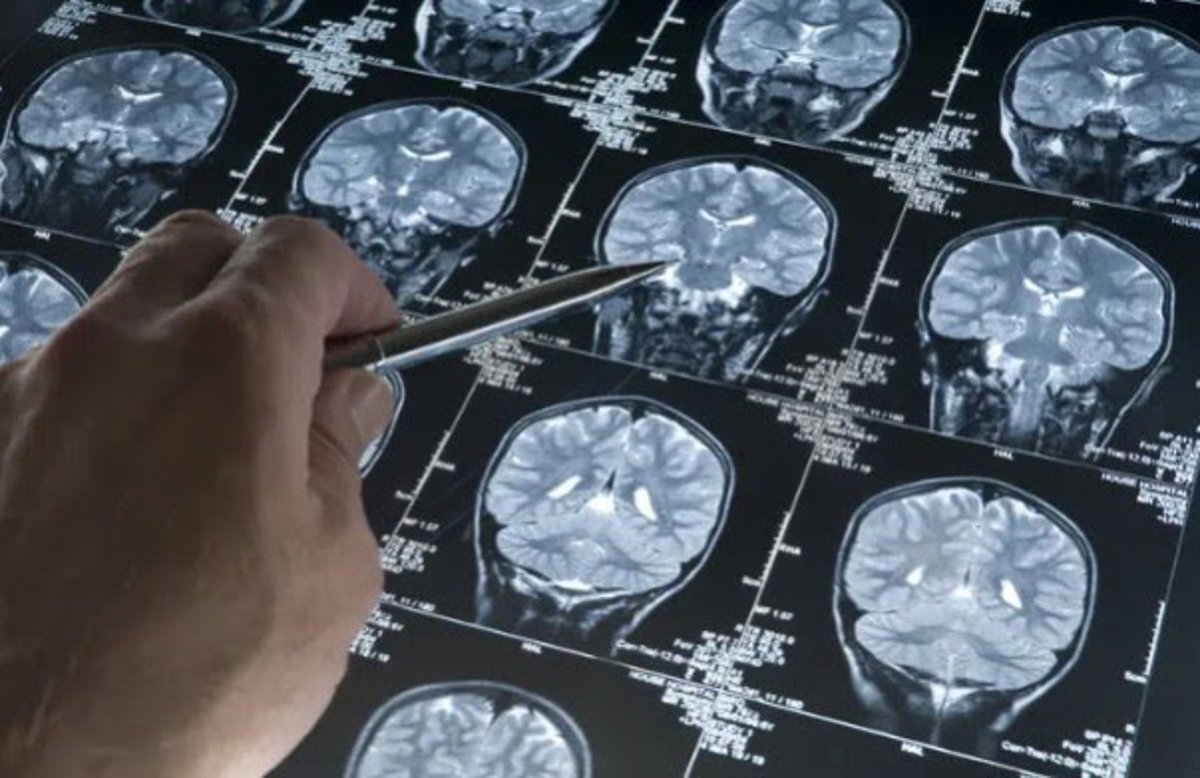
The Cancer-Alzheimer’s Paradox: How Blood Mutations are Redefining Dementia
For decades, medical science has observed a strange anomaly: patients battling cancer rarely develop Alzheimer’s, and those suffering from advanced dementia seldom face malignancy. This cancer and Alzheimer’s inverse relationship has long been a curiosity of epidemiology, suggesting a biological “tug-of-war” where the presence of one disease somehow shields the body from the other. However, new research is flipping this narrative on its head, revealing that while the diseases may not coexist, the genetic seeds of cancer may actually be the catalysts for cognitive decline.
The Great Paradox: Why Cancer and Alzheimer’s Seldom Coexist
The inverse relationship between these two killers suggests a complex interplay between the immune system and cellular aging. In cancer, cells proliferate uncontrollably; in Alzheimer’s, neurons wither and die. At first glance, they appear to be opposite ends of the biological spectrum.
Some theorists suggest that the aggressive immune response triggered by malignancy—or the treatments used to fight it—might inadvertently clear the amyloid plaques and tau tangles associated with Alzheimer’s. Conversely, the systemic inflammation and cellular senescence found in Alzheimer’s patients might create an environment where cancer cells struggle to take root.
But the most provocative discovery isn’t about why they stay apart, but how they are secretly linked through the blood.
The Hidden Link: Clonal Hematopoiesis and Brain Inflammation
Recent breakthroughs have identified a phenomenon known as clonal hematopoiesis of indeterminate potential (CHIP). This occurs when hematopoietic stem cells in the bone marrow acquire mutations—often the same mutations found in blood cancers like leukemia—without actually becoming cancer.
These “pre-cancerous” cells enter the bloodstream and migrate into the brain, where they transform into microglia, the brain’s resident immune cells. Unlike healthy microglia, these mutated cells are hyper-inflammatory.
Instead of protecting the brain, these mutated immune cells trigger a cascade of chronic inflammation that accelerates the accumulation of toxic proteins, effectively driving the progression of Alzheimer’s disease. In essence, the “cancerous” nature of the cells is not causing a tumor, but is instead poisoning the neural environment.
| Concept | Traditional View | Emerging Science |
|---|---|---|
| Relationship | Mutually exclusive diseases | Linked via immune dysfunction |
| Blood Role | Passive transport system | Vector for mutated immune cells |
| Trigger | Amyloid plaques as the cause | Systemic mutations as the driver |
From Paradox to Prediction: The Future of Early Diagnosis
The realization that blood-borne mutations can drive brain decay opens a revolutionary door: the ability to predict Alzheimer’s long before the first memory fails. If we can detect these specific cancerous mutations in a routine blood test, we may be able to identify high-risk individuals decades before clinical symptoms appear.
The Rise of Immuno-Neurology
We are entering the era of Immuno-Neurology. Rather than focusing solely on the brain’s internal chemistry, clinicians will look at the body’s systemic health. If the bone marrow is producing inflammatory, mutated cells, the brain is at risk.
This shift moves the treatment target from the brain (which is difficult to access due to the blood-brain barrier) to the blood and bone marrow, where interventions are far more feasible.
Precision Prevention and Targeted Therapies
Imagine a future where a “mutation profile” determines your preventative care. Patients with high levels of clonal hematopoiesis could be prescribed specific anti-inflammatory agents or therapies designed to “silence” these mutated clones before they ever reach the brain.
This represents a fundamental shift from reactive medicine—treating the dementia—to proactive genetic management—stopping the trigger.
Frequently Asked Questions About the Cancer-Alzheimer’s Link
Does having cancer protect me from Alzheimer’s?
While statistical data shows an inverse relationship, it is not a “protective” effect in a clinical sense. It suggests biological trade-offs and different immune profiles, but it is not a recommended or reliable shield against dementia.
If cancer mutations cause Alzheimer’s, does that mean I have cancer?
No. These are “somatic mutations” or clonal hematopoiesis. The cells have the genetic markers of cancer, but they do not form tumors or behave like a malignant growth. They cause inflammation, not oncology.
Can we cure Alzheimer’s by treating these blood mutations?
This is the current frontier of research. While we cannot yet “cure” it, targeting the inflammatory pathways created by these mutated cells is one of the most promising avenues for slowing the disease’s progression.
The intersection of oncology and neurology is revealing that the brain does not exist in a vacuum. The cancer and Alzheimer’s inverse relationship is not a mystery of coincidence, but a roadmap to understanding how systemic genetic instability manifests as cognitive failure. By treating the blood to save the brain, we are moving toward a world where dementia is not an inevitable part of aging, but a manageable systemic condition.
What are your predictions for the future of preventative neurology? Do you believe blood-based genetic screening will become the gold standard for dementia prevention? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.