The Dawn of Predictive Oncology: How Singapore’s New Molecular Imaging Centre Signals a Revolution in Cancer Care
Every two minutes, someone in the world begins cancer treatment. But what if, instead of reacting to cancer, we could predict its trajectory and intervene *before* it becomes a life-threatening crisis? Singapore’s recent launch of a new molecular imaging and theranostic centre, spearheaded by the National University Hospital (NUH) and the National University of Singapore (NUS), isn’t just about faster, safer scans – it’s a pivotal step towards that future. This isn’t merely an incremental improvement; it’s a paradigm shift in how we approach cancer, moving from detection to prediction and personalized intervention.
Beyond Detection: The Power of Theranostics
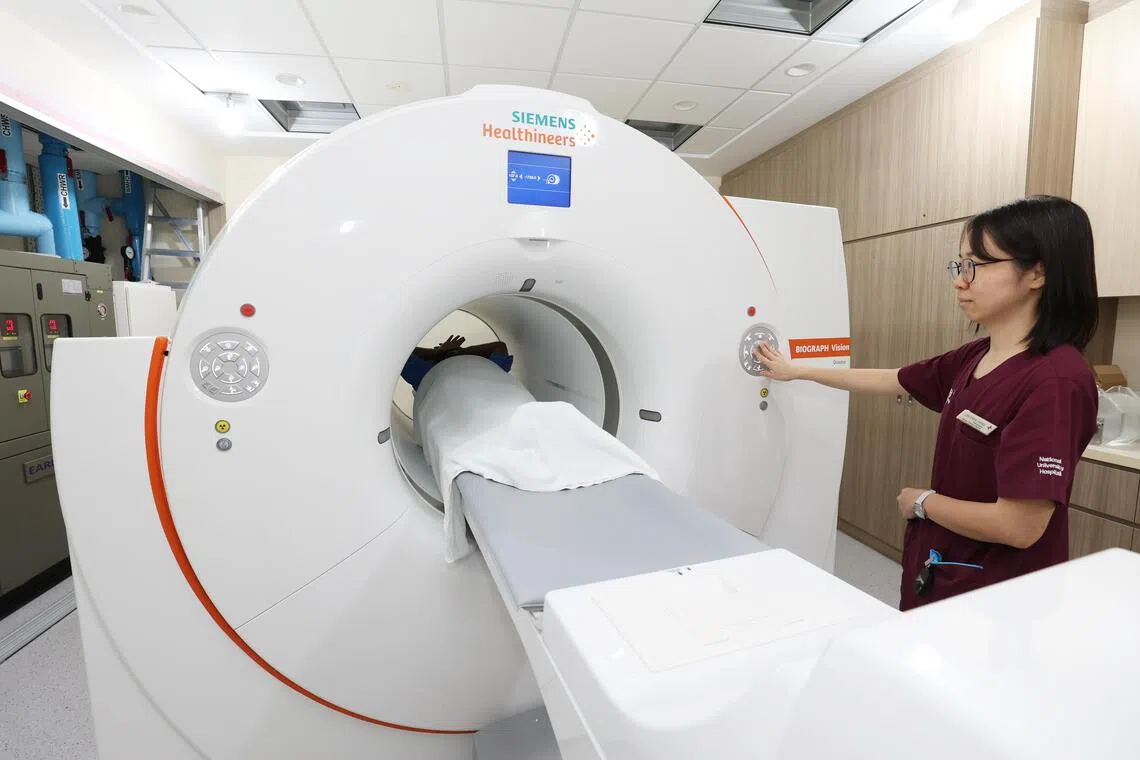
Traditional cancer diagnostics often rely on identifying tumors *after* they’ve grown to a significant size. The new centre, however, focuses on theranostics – a powerful combination of diagnostic imaging and targeted therapy. This means doctors can not only visualize the molecular characteristics of a tumor but also deliver therapeutic agents directly to cancer cells, minimizing damage to healthy tissue. The new scanner at NUH, as reported by The Straits Times, significantly enhances this capability, offering both speed and improved patient safety.
Molecular Imaging: Seeing Cancer at the Cellular Level
Molecular imaging isn’t about seeing the *size* of a tumor; it’s about understanding its *behavior*. It allows clinicians to visualize biological processes at the molecular level, identifying biomarkers that indicate the aggressiveness of the cancer, its potential to metastasize, and its responsiveness to different treatments. This level of detail is crucial for tailoring treatment plans to the individual patient, a cornerstone of precision medicine.
The Rise of AI-Powered Predictive Oncology
The data generated by these advanced imaging techniques is immense. This is where Artificial Intelligence (AI) comes into play. AI algorithms can analyze complex imaging data to identify subtle patterns that might be missed by the human eye, predicting a patient’s response to therapy with increasing accuracy. We’re already seeing early applications of AI in radiology, but the potential for predictive oncology is far greater. Imagine a future where AI can predict which patients are at high risk of developing cancer years before symptoms appear, allowing for preventative interventions.
Liquid Biopsies and the Future of Early Detection
While advanced imaging is crucial, it’s not the whole story. The convergence of molecular imaging with liquid biopsies – analyzing circulating tumor DNA (ctDNA) in the bloodstream – promises even earlier detection. Liquid biopsies can identify cancer cells or genetic material shed by tumors, even before they are visible on traditional scans. Combining the insights from both approaches will create a more comprehensive and proactive approach to cancer management.
Implications for Global Healthcare
Singapore’s investment in this technology isn’t just a national benefit; it’s a model for healthcare systems worldwide. The cost of cancer care is skyrocketing, and early detection and personalized treatment are key to reducing both human suffering and economic burden. The success of this centre could pave the way for similar facilities in other countries, accelerating the adoption of theranostics and AI-powered predictive oncology globally.
| Metric | Current Status (2024) | Projected Status (2030) |
|---|---|---|
| Global Cancer Cases (Annual) | ~19.3 Million | ~30 Million |
| 5-Year Cancer Survival Rate (Global Average) | ~65% | ~80% (with widespread adoption of predictive oncology) |
| Cost of Cancer Care (Global Annual) | ~$1.1 Trillion | ~$2.5 Trillion (without significant advancements in early detection) |
The future of cancer care isn’t about simply treating the disease; it’s about preventing it, predicting its course, and intervening with precision. Singapore’s new molecular imaging and theranostic centre is a beacon of hope, illuminating the path towards a world where cancer is no longer a death sentence, but a manageable condition.
Frequently Asked Questions About Predictive Oncology
What is the biggest challenge to implementing predictive oncology on a large scale?
The biggest challenge is the cost and complexity of the technology, as well as the need for highly trained personnel to interpret the data. Furthermore, ensuring equitable access to these advanced technologies will be crucial.
How will AI impact the role of oncologists in the future?
AI will not replace oncologists, but it will augment their abilities. AI will handle the complex data analysis, allowing oncologists to focus on patient interaction, treatment planning, and emotional support.
What are the ethical considerations surrounding predictive cancer testing?
Ethical considerations include the potential for anxiety and psychological distress caused by identifying a predisposition to cancer, as well as the potential for genetic discrimination. Robust ethical guidelines and patient counseling are essential.
What are your predictions for the future of cancer diagnostics and treatment? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.