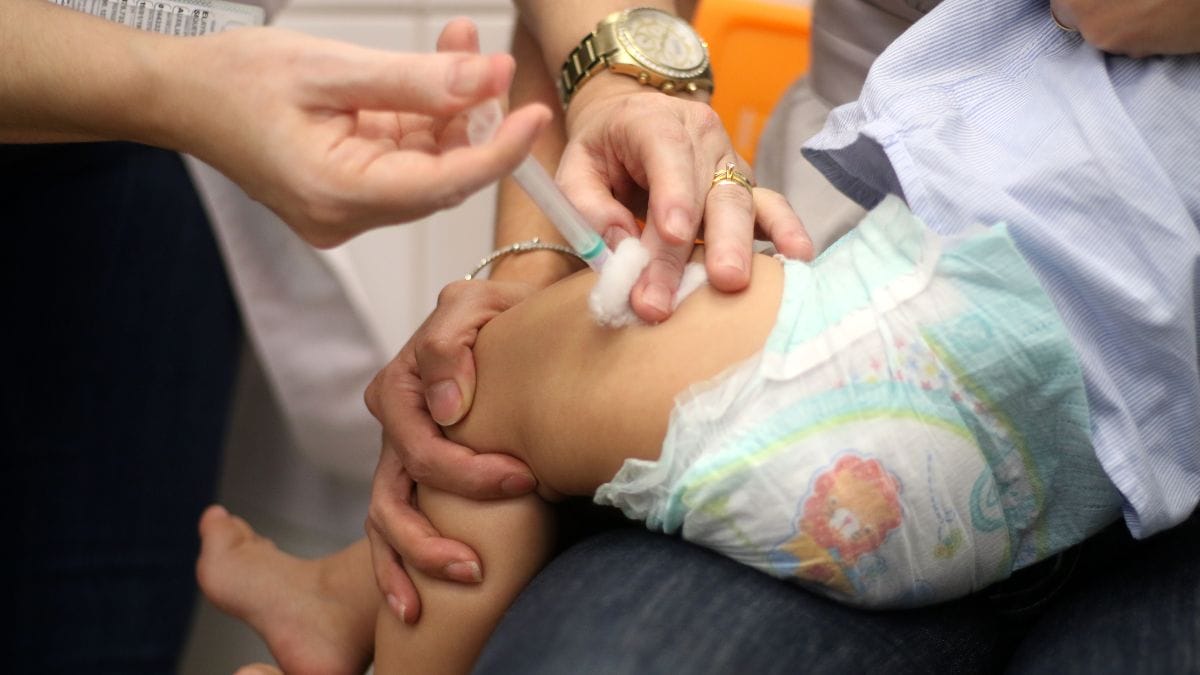
The Invisible Risk: Addressing Meningitis Vaccination Gaps in an Age of Health Misinformation
A single missed appointment is rarely viewed as a catastrophe, but in the realm of pediatric immunology, it can be a death sentence. The recent tragedy in Santa Catarina, where a six-month-old infant succumbed to meningitis due to a delayed vaccine dose, is not an isolated medical failure—it is a symptom of a widening systemic vulnerability. When we allow meningitis vaccination gaps to persist, we aren’t just risking individual lives; we are eroding the collective shield of herd immunity that has protected humanity for decades.
The Lethal Cost of a Missed Dose
Meningitis is a race against time. The inflammation of the protective membranes covering the brain and spinal cord can escalate from mild symptoms to total organ failure within hours. For an infant, whose immune system is still under construction, the margin for error is nonexistent.
The case in Papanduva serves as a harrowing reminder that the vaccination schedule is not a suggestion—it is a precisely engineered timeline. The second dose of a vaccine series is often what cements long-term immunity. When this window is missed, the child remains in a state of partial protection, leaving them dangerously exposed to aggressive bacterial strains.
The Psychology of Delay: Why Schedules are Slipping
Why are we seeing a rise in delayed doses in an era of unprecedented medical access? The answer lies in a complex intersection of “vaccine complacency” and targeted misinformation. As the horrors of polio and smallpox fade from living memory, the perceived risk of the disease drops, while the perceived risk of the vaccine rises.
Furthermore, the fragmentation of healthcare delivery means that a missed appointment may not be flagged until it is too late. In many regions, the burden of tracking falls entirely on the parent, creating a precarious system where a simple clerical error or a family emergency can result in a lethal gap in protection.
| Aspect of Care | Traditional Approach | Future-Proof Strategy |
|---|---|---|
| Tracking | Physical Health Cards | Blockchain-based Digital Health Passports |
| Reminders | Parental Memory/Manual Calls | AI-Driven Automated Alert Systems |
| Education | Generic Brochures | Personalized, Evidence-Based Digital Outreach |
The Future of Pediatric Preventative Care
To prevent future tragedies, the healthcare industry must pivot from a reactive model to a proactive one. We are entering an era where “predictive healthcare” can identify high-risk populations before an outbreak occurs. By utilizing big data, health ministries can pinpoint neighborhoods with declining vaccination rates and deploy mobile clinics to close those gaps in real-time.
Imagine a system where a child’s health record is linked to a global registry that triggers an automatic alert to both the parent and the local clinic the moment a dose becomes overdue. This shift from “waiting for the patient” to “seeking the patient” is the only way to eliminate the lethal windows of vulnerability.
Beyond the Clinic: Building a Culture of Vigilance
Medical technology alone cannot solve the problem of vaccine hesitancy. The future of public health depends on rebuilding trust. This requires a move toward transparent, empathetic communication that acknowledges parental fears without compromising scientific integrity.
Community-led health vigilance—where local leaders and peers advocate for immunization—has proven more effective than top-down government mandates. When the drive for vaccination comes from a place of community protection rather than bureaucratic requirement, adherence rates soar.
Frequently Asked Questions About Meningitis Vaccination Gaps
What happens if a vaccine dose is delayed by a few weeks?
While a short delay may not always result in infection, it creates a “window of vulnerability” where the child is not fully protected. The level of risk depends on the prevalence of the disease in the local community.
Can meningitis be prevented without vaccines?
While hygiene and avoiding crowded spaces can reduce risk, vaccines are the only definitive way to prime the immune system to recognize and fight the specific bacteria and viruses that cause meningitis.
How can parents ensure their children are up to date?
Parents should utilize digital health apps, request automated reminders from their pediatrician, and double-check the national immunization calendar regularly.
Why is the second dose often more critical than the first?
The first dose typically primes the immune system, while subsequent doses (boosters) increase the concentration of antibodies and ensure the immunity lasts for years rather than months.
The loss of a child to a preventable disease is a failure of the system, not just a tragedy of circumstance. As we move forward, the goal must be the total elimination of vaccination gaps through the integration of smarter technology and a renewed commitment to public health literacy. We must treat every missed dose as a critical alarm, because in the fight against meningitis, there are no second chances.
What are your predictions for the future of pediatric health tracking? Do you believe AI can solve the vaccine hesitancy crisis? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.