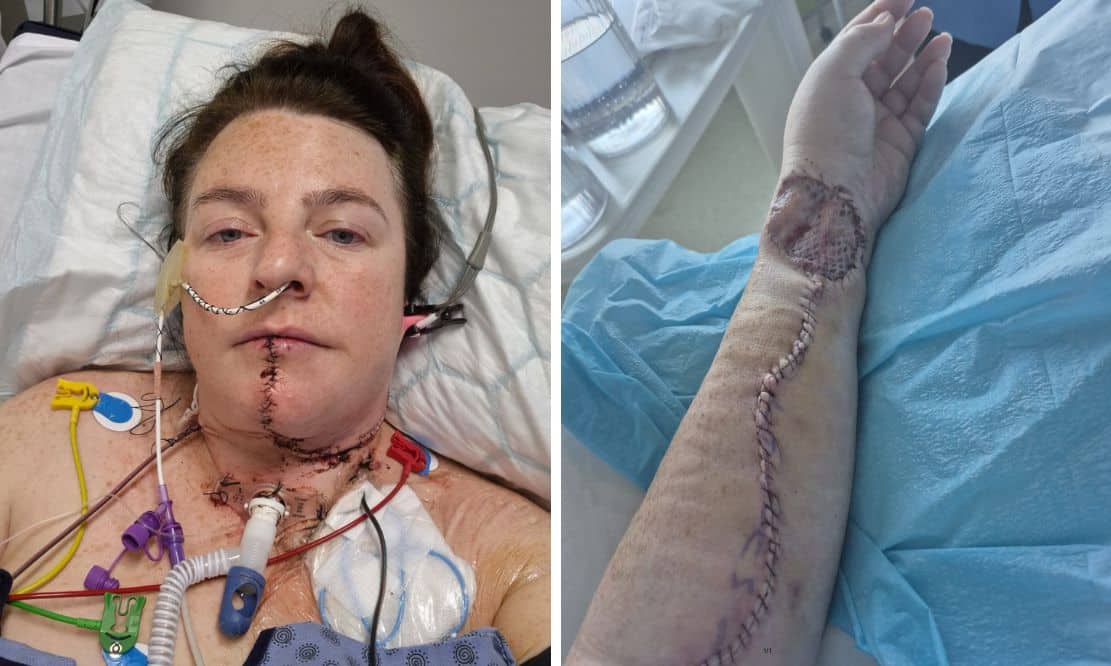
The most dangerous medical symptoms are often the ones that feel familiar. For Jennifer O’Hanlon, a 44-year-old nurse from Killeavy, a persistent “mouth ulcer” was not a minor annoyance—it was the camouflage for Stage Four squamous cell carcinoma. Her journey from a routine dental concern to a harrowing 15-hour surgery serves as a stark reminder that the gap between a benign sore and a life-threatening malignancy can be perilously thin.
- Symptom Masking: Oral cancers, specifically squamous cell carcinoma, often mimic common ailments like mouth ulcers, leading to dangerous delays in diagnosis.
- Aggressive Intervention: Stage Four diagnosis required a partial glossectomy (tongue removal) and a “free flap” reconstructive surgery using tissue from the arm.
- The “New Normal”: Survival often comes with a lifelong “war wound” portfolio, including speech impediments, chronic pain, and endocrine dysfunction.
The Deep Dive: The Danger of the “Benign” Assumption
Jennifer’s experience highlights a critical failure in early symptom recognition—not necessarily by the patient, but by the natural tendency to normalize discomfort. For months, O’Hanlon attributed her sore to dental rubbing, a common rationalization that allowed the cancer to progress to Stage Four. From a clinical perspective, squamous cell carcinoma (SCC) in the oral cavity is aggressive; by the time it reaches the lymph nodes, the surgical requirements become extreme.
The complexity of her treatment underscores the brutality of late-stage head and neck cancers. A 15-hour surgery involving the “cracking” of the jaw and the removal of 39 lymph nodes is a systemic trauma. Furthermore, the use of a “free flap” (transferring skin and blood vessels from the arm to the tongue) represents the pinnacle of reconstructive plastics, yet it leaves the patient with a permanent physiological alteration.
Beyond the surgery, the “hidden” cost of recovery is the systemic collapse caused by radiotherapy. The induced early menopause, underactive thyroid, and chronic “brain fog” described by O’Hanlon are not mere side effects—they are permanent shifts in biological baseline. This is what medical professionals refer to as the “new normal,” a psychological state of mourning for one’s former physical self.
The Forward Look: Patient-Led Advocacy and the Screening Gap
Jennifer’s move to document her recovery on TikTok (Jen’s Journey | SCC) represents a growing trend in “patient-advocacy” that is filling a void left by traditional healthcare brochures. By humanizing the “horrendous” aspects of treatment, survivors are effectively conducting public health screenings via social media, urging others to seek biopsies for sores that do not heal within two weeks.
Looking ahead, O’Hanlon’s case suggests three critical areas of focus for public health:
First, there is a pressing need for increased vigilance in primary dental care. Because dentists are often the first to see oral lesions, the window between a “careful look” and a biopsy referral is the most critical period for patient survival.
Second, the integration of psychological support—such as the counselors and psychologists O’Hanlon now sees—must be standardized as part of the oncology protocol, rather than an afterthought. The “mourning” process of losing basic functions like eating a burger or speaking clearly is a distinct form of trauma.
Finally, we can expect a rise in the use of digital support networks to combat the isolation of rare or disfiguring cancers. As Jennifer’s 3,000+ followers demonstrate, the peer-to-peer support model is becoming an essential component of the recovery process, providing the emotional scaffolding that clinical settings often lack.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.