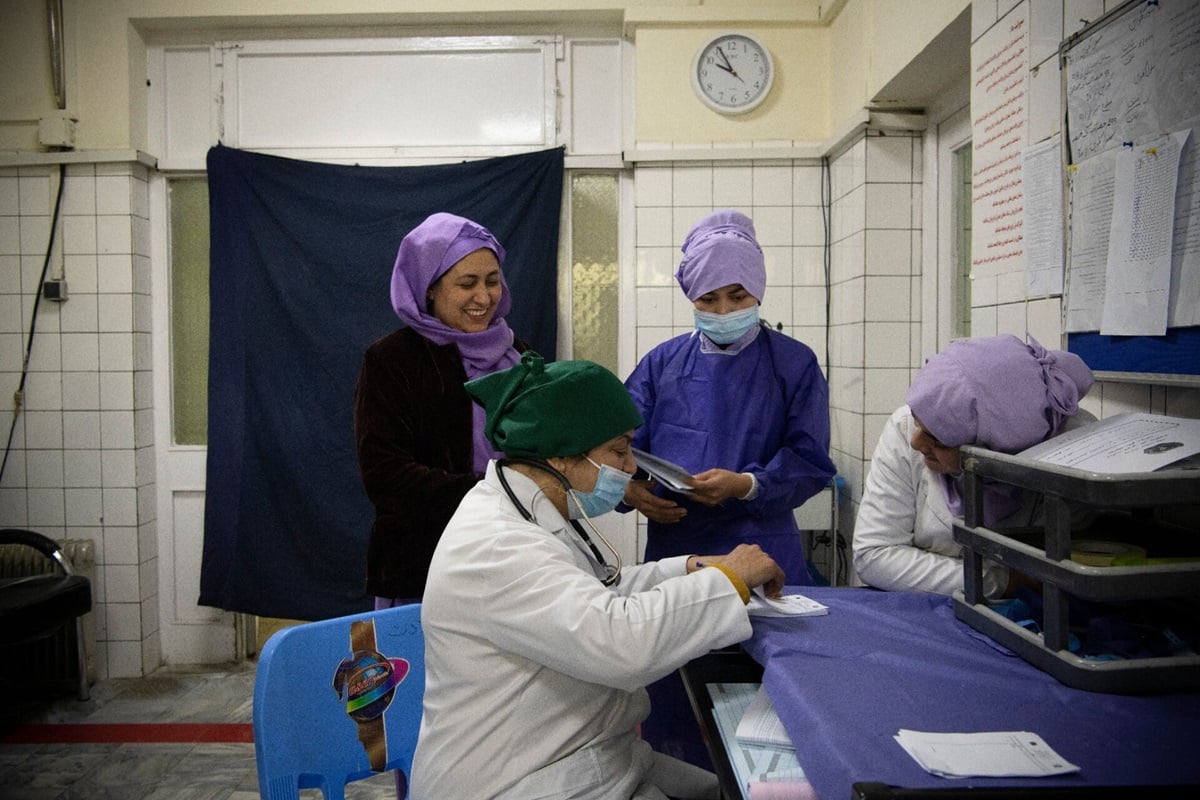
Beyond Uterotonic Drugs: The Emerging Tech & Global Strategies to Eradicate Postpartum Hemorrhage
Every minute, approximately two women die from postpartum hemorrhage (PPH) – excessive bleeding after childbirth. While seemingly a relic of the past in developed nations, PPH remains a leading cause of maternal mortality globally, responsible for roughly 20% of all maternal deaths. But a quiet revolution is underway, moving beyond traditional uterotonic drugs and embracing a multi-faceted approach fueled by technological innovation and strengthened global collaboration. This isn’t just about saving lives today; it’s about building resilient maternal healthcare systems prepared for the challenges of tomorrow.
The Limitations of Current Approaches & The Urgent Need for Innovation
For decades, the primary response to PPH has centered around uterotonic drugs like oxytocin and misoprostol. While effective, these medications face significant hurdles in low-resource settings: cold chain requirements for oxytocin, administration challenges, and potential side effects. Furthermore, relying solely on medication addresses the *symptom* of PPH, not the underlying risk factors. **Postpartum hemorrhage** is often exacerbated by delayed access to care, inadequate antenatal screening, and a lack of skilled birth attendants.
The recent recommendations from the World Health Organization (WHO), the International Confederation of Midwives, and highlighted in Newsweek, signal a crucial shift. They emphasize a proactive, multi-pronged strategy encompassing prevention, early detection, and rapid response. But these recommendations are just the starting point. The real progress will come from integrating cutting-edge technologies and addressing systemic inequalities.
Tech-Enabled Solutions: From Predictive Analytics to Remote Monitoring
Several promising technologies are emerging to tackle PPH on multiple fronts. Predictive analytics, powered by machine learning, are being developed to identify women at high risk of PPH based on factors like medical history, gestational age, and even socioeconomic indicators. This allows for targeted interventions *before* delivery.
Remote monitoring devices, including wearable sensors, are showing potential for early detection of excessive bleeding. These devices can track vital signs and alert healthcare providers to potential problems in real-time, even in remote areas with limited access to facilities. Imagine a future where a simple, affordable sensor worn by a new mother can automatically summon help if bleeding becomes dangerous – a game-changer for maternal survival.
The Rise of Uterine Balloon Tamponade & Non-Invasive Techniques
Beyond prevention and detection, advancements in treatment are also critical. Uterine balloon tamponade (UBT), a technique involving the insertion of a balloon into the uterus to apply pressure and stop bleeding, is gaining traction as a life-saving intervention, particularly in settings where blood transfusions are scarce. Furthermore, research is exploring non-invasive techniques like focused ultrasound to control hemorrhage, offering a potentially less traumatic alternative to surgical interventions.
Strengthening Healthcare Systems: Training, Infrastructure & Equity
Technology alone isn’t enough. Sustainable progress requires a fundamental strengthening of healthcare systems. This includes investing in comprehensive training for skilled birth attendants, ensuring access to essential supplies (including uterotonics, UBT devices, and blood products), and improving infrastructure in underserved communities.
Crucially, addressing the social determinants of health is paramount. Poverty, lack of education, and limited access to healthcare disproportionately impact women’s risk of PPH. Equitable access to quality maternal care must be a central tenet of any successful strategy.
| Metric | Current Status (2024) | Projected Improvement (2030) |
|---|---|---|
| Global Maternal Mortality Rate (per 100,000 live births) | 223 | Below 70 |
| PPH Contribution to Maternal Deaths | 20% | Below 10% |
| Access to Skilled Birth Attendants (Global) | 80% | 95% |
The Future of PPH Prevention: Personalized Medicine & AI-Driven Protocols
Looking ahead, the future of PPH prevention lies in personalized medicine. Imagine a scenario where a woman’s risk profile is assessed early in pregnancy, and a tailored prevention plan is developed based on her individual needs. This could involve prophylactic medication, targeted monitoring, or even genetic screening to identify predispositions to bleeding disorders.
Artificial intelligence (AI) will play an increasingly important role, not only in predictive analytics but also in developing standardized treatment protocols and providing real-time guidance to healthcare providers. AI-powered decision support tools could help clinicians quickly assess a patient’s condition and select the most appropriate intervention, even in challenging circumstances.
Frequently Asked Questions About Postpartum Hemorrhage
<h3>What is the biggest challenge in preventing PPH in developing countries?</h3>
<p>The biggest challenge is a combination of factors: limited access to skilled birth attendants, inadequate infrastructure, lack of essential supplies, and the social determinants of health that disproportionately affect vulnerable populations.</p>
<h3>How can technology help reduce PPH-related deaths?</h3>
<p>Technology offers solutions for prevention (predictive analytics), early detection (remote monitoring), and treatment (uterine balloon tamponade, focused ultrasound). AI can also play a role in optimizing treatment protocols.</p>
<h3>What role do midwives play in preventing PPH?</h3>
<p>Midwives are crucial in providing antenatal care, identifying risk factors, managing labor and delivery, and providing immediate postpartum care. Their training and expertise are essential for preventing and managing PPH.</p>
<h3>Is PPH preventable in most cases?</h3>
<p>Yes, PPH is largely preventable with access to quality maternal care, proactive risk assessment, and timely interventions. The new WHO recommendations and emerging technologies are paving the way for a future where PPH-related deaths are significantly reduced.</p>The fight against postpartum hemorrhage is far from over, but the convergence of innovative technologies, strengthened healthcare systems, and a renewed global commitment offers a beacon of hope. The goal of eradicating preventable maternal deaths is within reach, but it requires sustained investment, collaborative action, and a relentless focus on equity. What are your predictions for the future of maternal healthcare and PPH prevention? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.