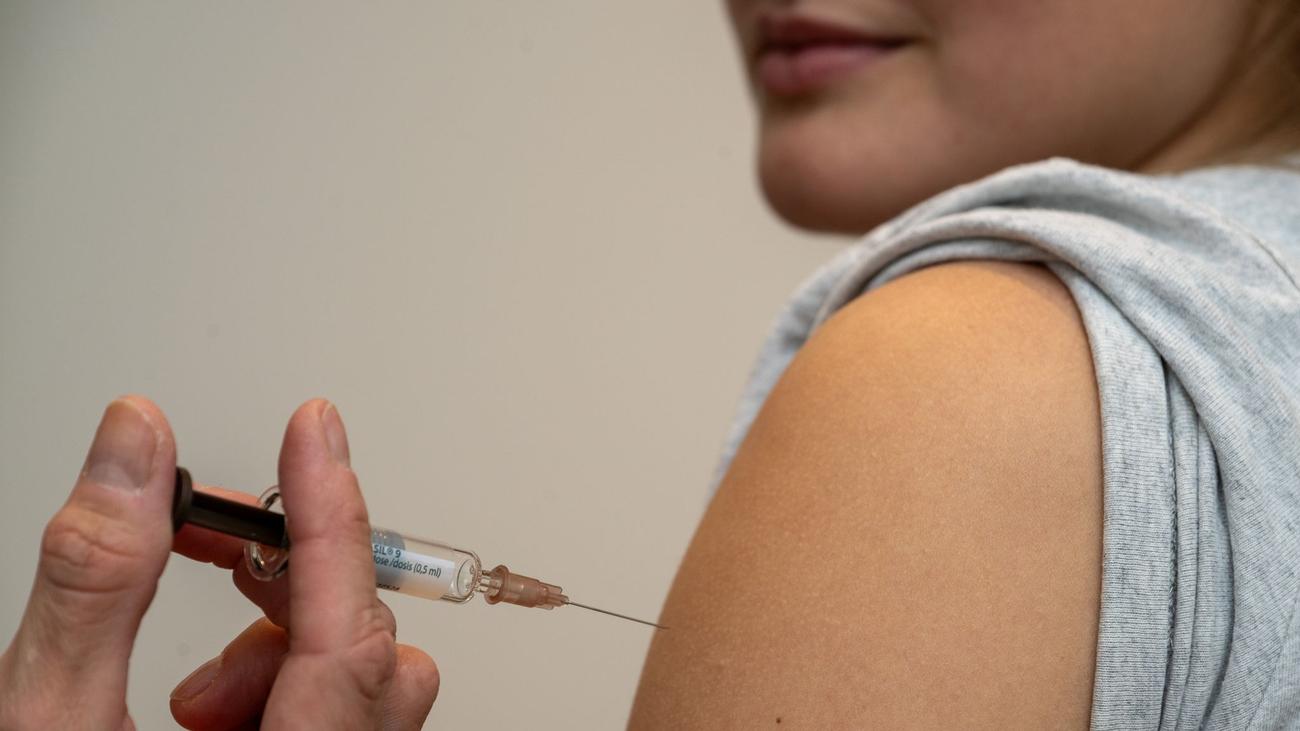
HPV Vaccination: A Critical Shield Against Rising Cancer Rates
Recent reports from Hamburg, Germany, signal a renewed push to bolster HPV vaccination rates, particularly among young people. This initiative comes amidst growing concern over the preventable cancers linked to the human papillomavirus (HPV), and promising advancements in vaccine technology, including potential breakthroughs in treating HPV-related throat cancers. Public health officials and oncologists are increasingly emphasizing the importance of widespread vaccination as a cornerstone of cancer prevention.
For decades, the HPV vaccine has been a vital tool in protecting against cervical cancer. However, its benefits extend far beyond this, offering protection against cancers of the vagina, vulva, anus, penis, and oropharynx (back of the throat, including the base of the tongue and tonsils). The latest research indicates that HPV is responsible for a significant proportion of these cancers – approximately one-third of all cancer cases worldwide are potentially preventable through vaccination, according to experts.
Understanding HPV and its Cancerous Potential
HPV is a remarkably common virus, transmitted through skin-to-skin contact, most often during sexual activity. While many HPV infections clear up on their own, certain high-risk strains can persist and lead to cellular changes that can develop into cancer over time. The HPV vaccine works by stimulating the body’s immune system to produce antibodies that recognize and neutralize these high-risk HPV types.
Traditionally, HPV vaccination programs have focused on girls and young women to prevent cervical cancer. However, recognizing the virus’s impact on men and the rising incidence of HPV-related oropharyngeal cancers, vaccination recommendations are evolving. Increasingly, health organizations advocate for universal HPV vaccination – meaning both boys and girls should receive the vaccine.
The Expanding Scope of HPV Vaccine Protection
The initial HPV vaccines targeted the most common cancer-causing strains of the virus. Newer, more comprehensive vaccines, such as the 9-valent vaccine, offer protection against even more HPV types, significantly broadening the scope of protection. Recent studies, like those highlighted by ekhbary.com, demonstrate promising early success in treating HPV-related throat tumors, offering a potential new avenue for cancer therapy.
What role does early detection play in managing HPV-related cancers? And how can we address vaccine hesitancy to maximize public health benefits?
The push to increase vaccination rates in Hamburg, as reported by THE TIME, underscores the growing recognition of HPV vaccination as a crucial public health intervention. Similar initiatives are gaining momentum globally, driven by the compelling evidence of the vaccine’s effectiveness. Apotheke Adhoc highlights the protective benefits for girls, while NDR.de emphasizes protection against cancers of the vagina and vulva.
Frequently Asked Questions About HPV Vaccination
-
What is the recommended age for HPV vaccination?
The CDC recommends routine HPV vaccination for adolescents aged 11 or 12 years. Vaccination can be started as early as age 9. Catch-up vaccination is recommended for those who didn’t receive the vaccine as adolescents, up to age 26.
-
Is the HPV vaccine safe?
Yes, the HPV vaccine has been extensively studied and is considered very safe. Common side effects are usually mild, such as pain or swelling at the injection site.
-
Can the HPV vaccine protect against all types of HPV?
No, the HPV vaccine does not protect against all types of HPV. However, it protects against the types most likely to cause cancer and genital warts.
-
Does HPV vaccination eliminate the need for regular cancer screenings?
No, even after HPV vaccination, regular cancer screenings, such as Pap tests for cervical cancer, are still important. The vaccine doesn’t provide complete protection, and screenings can detect any early signs of cancer.
-
What if I’m already sexually active – is the HPV vaccine still beneficial?
Yes, even if you’re already sexually active, the HPV vaccine can still provide protection against HPV types you haven’t been exposed to yet. It’s less effective if you’ve already been infected with the HPV types the vaccine targets, but it can still offer significant benefits.
As highlighted by RTL.de, a significant portion of cancer cases are preventable with vaccination. The evidence is clear: HPV vaccination is a powerful tool in the fight against cancer.
Share this vital information with your friends and family. Let’s work together to protect future generations from the devastating impact of HPV-related cancers. Join the conversation – what are your thoughts on expanding HPV vaccination programs?
Disclaimer: This article provides general information and should not be considered medical advice. Please consult with a qualified healthcare professional for personalized guidance.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.