Timing Matters: Chemotherapy Infusion Schedule Significantly Impacts Lung Cancer Progression
New research reveals a critical factor in the fight against advanced non-small cell lung cancer: when patients receive their chemotherapy infusions. A groundbreaking phase 3 clinical trial demonstrates that administering chemotherapy, in combination with either sintilimab or pembrolizumab, earlier in the day—before 3:00 PM—leads to substantially improved progression-free survival rates compared to later infusions. This discovery could revolutionize treatment protocols and offer renewed hope to individuals battling this aggressive disease.
Understanding Non-Small Cell Lung Cancer and Immunotherapy
Non-small cell lung cancer (NSCLC) accounts for approximately 80-85% of all lung cancer diagnoses. Stage III and IV NSCLC represent advanced stages of the disease, often characterized by metastasis and a more challenging prognosis. Traditional treatments, including chemotherapy and radiation therapy, aim to shrink tumors and alleviate symptoms, but often come with significant side effects.
Immunotherapy, a newer approach, harnesses the power of the body’s own immune system to fight cancer. Drugs like sintilimab and pembrolizumab are checkpoint inhibitors, which work by blocking proteins that prevent immune cells from attacking cancer cells. Combining immunotherapy with chemotherapy has shown promise in improving outcomes for NSCLC patients, but this latest research suggests that even the timing of treatment can play a crucial role.
The Circadian Rhythm and Cancer Treatment
The body’s natural circadian rhythm—the internal clock that regulates various physiological processes—influences the effectiveness of many medications. Emerging evidence suggests that cancer cells are also susceptible to these rhythmic variations. The timing of chemotherapy administration may impact drug metabolism, tumor cell sensitivity, and immune response. This study provides compelling evidence supporting the idea that aligning treatment with the body’s natural rhythms can optimize therapeutic benefits.
Could this finding extend to other cancer types and treatments? Further research is needed to explore the potential of chronotherapy—timing treatments to coincide with optimal biological conditions—across a broader range of malignancies. What other factors, beyond infusion time, might influence the efficacy of cancer therapies?
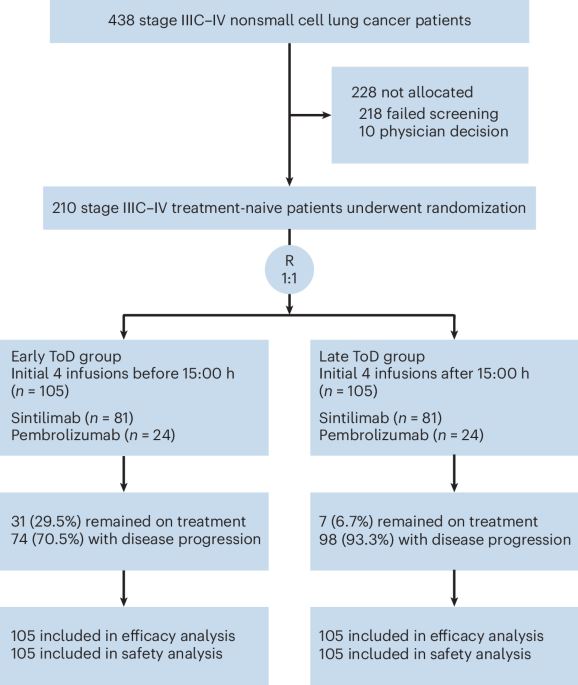
The study, detailed in Nature Medicine, involved patients with treatment-naive stage III–IV NSCLC. Researchers randomly assigned participants to receive either sintilimab or pembrolizumab in combination with chemotherapy, with infusions administered either before 3:00 PM or later in the day. The results clearly demonstrated a statistically significant improvement in progression-free survival among those receiving early-day infusions.
For more information on lung cancer and treatment options, visit the American Cancer Society and the American Lung Association.
Frequently Asked Questions About Lung Cancer Treatment Timing
- Does the timing of chemotherapy infusions affect lung cancer progression?
Yes, this research indicates that administering chemotherapy and immunotherapy earlier in the day (before 3:00 PM) significantly improves progression-free survival in patients with advanced non-small cell lung cancer. - What is the role of the circadian rhythm in cancer treatment?
The body’s circadian rhythm influences drug metabolism, tumor cell sensitivity, and immune response, potentially impacting the effectiveness of cancer therapies. - Are sintilimab and pembrolizumab the only immunotherapies affected by infusion timing?
While this study focused on sintilimab and pembrolizumab, further research is needed to determine if other immunotherapies are also affected by the timing of administration. - What stages of lung cancer were included in this study?
The study included patients with treatment-naive stage III–IV non-small cell lung cancer, representing advanced stages of the disease. - Should all lung cancer patients inquire about early-day infusions?
Patients undergoing chemotherapy should discuss their daily schedules with their oncology team to explore the possibility of scheduling infusions earlier in the day, as it may potentially maximize treatment effectiveness. - What is progression-free survival and why is it important?
Progression-free survival measures the length of time during which a patient lives with the disease without it getting worse. It’s a key indicator of treatment effectiveness.
This research underscores the importance of personalized medicine and the need to consider individual biological rhythms when designing cancer treatment plans. As we continue to unravel the complexities of cancer, optimizing treatment timing may prove to be a simple yet powerful strategy for improving patient outcomes.
Share this vital information with your network and join the conversation below. What are your thoughts on the potential of chronotherapy in cancer treatment?
Disclaimer: This article provides general information and should not be considered medical advice. Please consult with a qualified healthcare professional for any health concerns or before making any decisions related to your treatment.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.