Genetic Factors Linked to IVF Failure: New Research Offers Hope for Improved Fertility Treatments
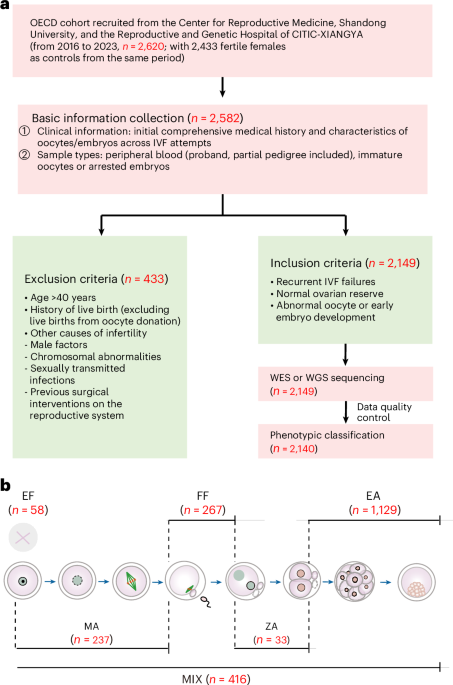
A groundbreaking study has identified specific genetic variations that may contribute to unsuccessful in vitro fertilization (IVF) cycles, offering a potential pathway toward more personalized and effective fertility treatments. Researchers analyzed the genetic makeup of over 2,140 women experiencing recurrent IVF failure, pinpointing genes crucial for both egg quality and early embryo development. This discovery represents a significant leap forward in understanding the complex biological factors underlying female infertility.
For couples struggling with infertility, repeated IVF failures can be emotionally and financially draining. Often, the cause remains elusive, leaving patients and physicians frustrated. This new research, however, suggests that in a substantial number of cases, the root of the problem may lie within the patient’s genetic code. Identifying these genetic markers could allow for pre-treatment screening, enabling doctors to tailor IVF protocols or explore alternative reproductive options.
Unlocking the Secrets of Oocyte and Embryo Competence
The study, detailed in Nature Medicine, utilized whole-exome sequencing – a technique that analyzes the protein-coding regions of genes – to identify variations associated with diminished oocyte (egg) and early embryo competence. Researchers didn’t just identify these genes; they also conducted functional analyses to confirm their role in the critical processes of egg maturation and early embryonic development. This dual approach strengthens the validity of the findings.
What exactly does “oocyte competence” mean? It refers to an egg’s ability to be successfully fertilized, undergo normal chromosomal division, and support early embryonic growth. Similarly, embryo competence describes the embryo’s capacity to implant in the uterus and develop into a healthy pregnancy. Defects in either of these areas can lead to IVF failure, even when other factors appear optimal.
The Role of Genetics in IVF Success Rates
While IVF has revolutionized reproductive medicine, success rates remain far from 100%. Factors like age, lifestyle, and underlying medical conditions all play a role. However, this research highlights the often-overlooked contribution of genetics. Could genetic testing become a standard part of the IVF workup in the future? It’s a possibility that’s now much closer to reality.
The identified genes are involved in a variety of cellular processes, including DNA repair, chromosome segregation, and cellular metabolism. Variations in these genes can disrupt these processes, leading to errors in egg and embryo development. Interestingly, some of the genes identified have previously been linked to other genetic disorders, suggesting a potential overlap between infertility and broader genetic health.
What are the implications for patients currently undergoing IVF? While widespread genetic testing isn’t yet available, this research provides a crucial foundation for developing such tests. Furthermore, it opens up new avenues for research into potential therapies that could overcome the effects of these genetic variations. Do you think genetic counseling should be mandatory for all couples considering IVF?
The study also underscores the importance of considering both the mother’s and father’s genetic contributions to infertility. While this research focused specifically on women, genetic factors from the male partner can also significantly impact IVF outcomes. Understanding the interplay between maternal and paternal genetics is a key area for future investigation.
Understanding Female Infertility: A Comprehensive Overview
Female infertility is a complex issue affecting millions of women worldwide. It can stem from a variety of factors, including ovulation disorders, fallopian tube blockage, endometriosis, and uterine abnormalities. However, in many cases, the cause remains unexplained. This is often referred to as unexplained infertility, and it’s in these cases that genetic factors are increasingly suspected to play a role.
IVF, while a powerful tool, isn’t a guaranteed solution. The average success rate per cycle varies depending on age and other factors, but it’s typically around 30-40%. This means that many couples undergo multiple cycles before achieving a successful pregnancy. Identifying genetic risk factors could help to improve these odds and reduce the emotional and financial burden of repeated IVF failures.
Beyond genetic testing, other advancements in reproductive technology are also showing promise. These include preimplantation genetic testing (PGT), which screens embryos for chromosomal abnormalities before implantation, and advancements in egg freezing techniques. RESOLVE: The National Infertility Association provides comprehensive resources and support for individuals and couples facing infertility.
Frequently Asked Questions About Genetic Factors and IVF
A: While genetic testing can identify potential risk factors, it cannot definitively predict IVF success. It provides valuable information that can help tailor treatment plans and manage expectations.
A: This research identified several genes involved in DNA repair, chromosome segregation, and cellular metabolism. The specific genes vary, and further research is ongoing to identify additional genetic markers.
A: Insurance coverage for genetic testing for infertility varies widely. It’s important to check with your insurance provider to determine your specific coverage.
A: Egg quality is a critical factor in IVF success. Eggs with genetic abnormalities or defects in their cellular machinery are less likely to be fertilized or develop into healthy embryos.
A: Alternatives may include donor eggs or donor sperm, depending on the specific genetic factors involved. Adoption is also a viable option.
This research offers a beacon of hope for individuals and couples navigating the challenges of infertility. By unraveling the genetic complexities of reproductive health, we move closer to a future where personalized fertility treatments are the norm, maximizing the chances of a successful pregnancy for all.
What further research do you believe is most crucial in this field?
Disclaimer: This article provides general information and should not be considered medical advice. Please consult with a qualified healthcare professional for personalized guidance on fertility treatments and genetic testing.
Share this article with anyone who may find it helpful, and join the conversation in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.