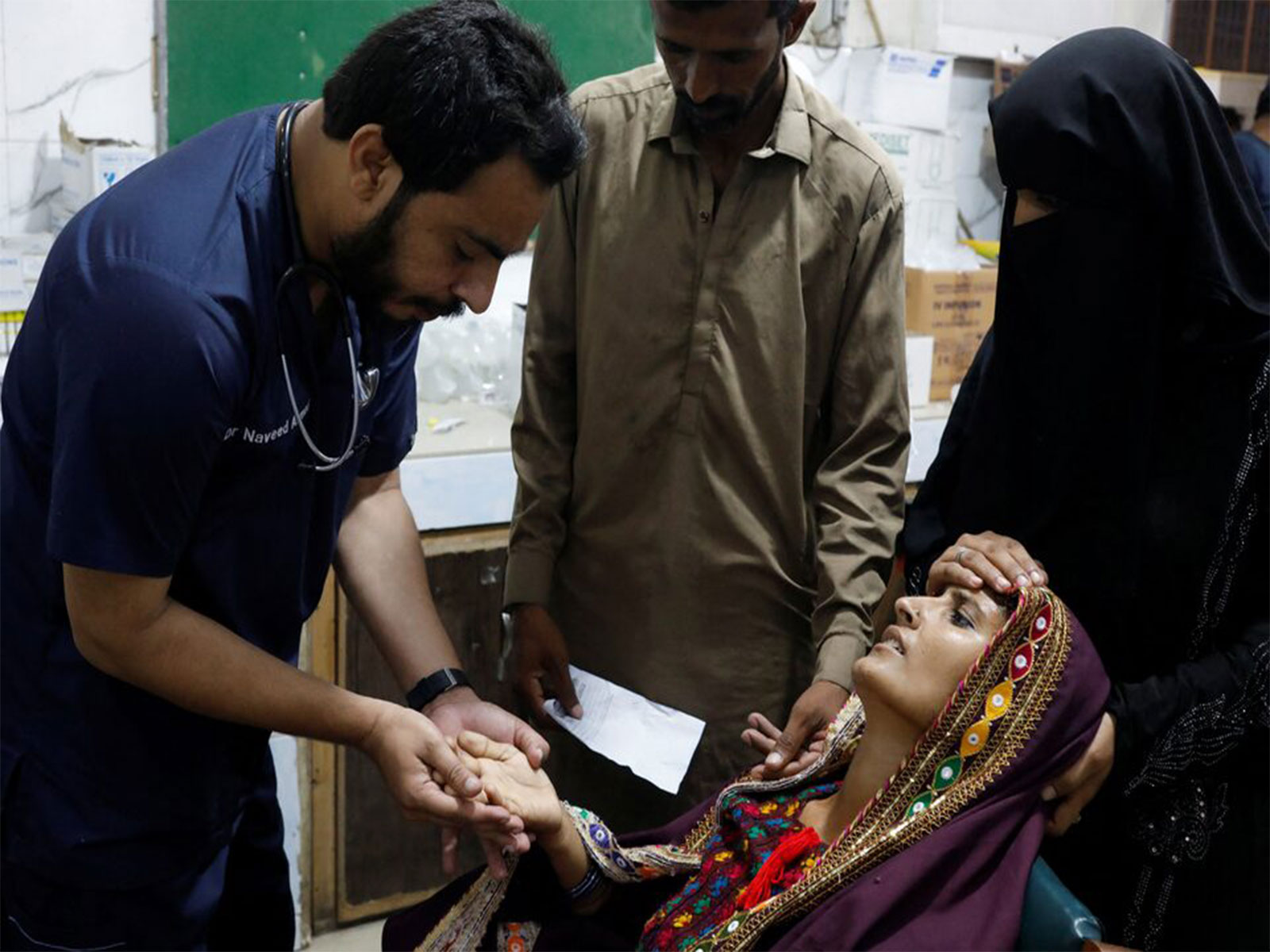
A staggering 215,000 malaria cases reported in Sindh province, Pakistan, in 2025 isn’t just a regional health statistic – it’s a flashing warning signal. The escalating incidence of malaria, alongside concurrent outbreaks of dengue, isn’t simply a matter of insufficient mosquito control. It’s a complex interplay of climate change, governmental shortcomings, and, critically, questions surrounding the reliability of public health data. This situation in Sindh is increasingly becoming a blueprint for challenges other regions will face as climate patterns shift and vector-borne diseases expand their reach.
The Perfect Storm: Climate Change and Vector-Borne Disease
Pakistan is acutely vulnerable to the impacts of climate change, and Sindh province is on the front lines. Increased rainfall, coupled with rising temperatures, creates ideal breeding grounds for mosquitoes. These altered conditions are extending the transmission season for malaria and dengue, pushing the disease burden beyond traditional peak periods. The recent floods have further exacerbated the problem, creating vast stagnant water pools – perfect mosquito habitats. But climate change isn’t the sole culprit; it’s acting as a threat multiplier, exposing existing weaknesses in Pakistan’s public health infrastructure.
Data Transparency and the Erosion of Trust
Reports from organizations like ANI News and ARY News highlight concerns about government apathy and potential data manipulation regarding the true scale of the crisis. Accurate epidemiological data is the cornerstone of effective public health response. If data is suppressed, misrepresented, or simply unavailable, it becomes impossible to allocate resources effectively, implement targeted interventions, or accurately assess the impact of control measures. The lack of transparency fuels public distrust and hinders collaborative efforts to combat the spread of disease. This isn’t just a Pakistani problem; globally, the integrity of health data is increasingly under scrutiny, particularly in regions facing political instability or resource constraints.
Beyond Mosquito Nets: A Multi-Pronged Approach
The Sindh government’s province-wide anti-dengue and malaria drive, as reported by The Nation, is a necessary first step. However, relying solely on reactive measures like insecticide spraying and mosquito net distribution is insufficient. A truly effective strategy requires a proactive, multi-pronged approach that addresses the root causes of the problem.
Investing in Early Warning Systems
Predictive modeling, leveraging climate data and real-time disease surveillance, can provide early warnings of potential outbreaks. This allows for pre-emptive resource allocation and targeted interventions, minimizing the impact of disease transmission. Investing in robust surveillance systems, including rapid diagnostic testing and community-based reporting, is crucial for detecting outbreaks early and tracking their spread.
Strengthening Public Health Infrastructure
Pakistan’s public health infrastructure, particularly in rural Sindh, is chronically underfunded and understaffed. Investing in training healthcare workers, improving access to essential medicines and diagnostic tools, and strengthening laboratory capacity are essential for building a resilient health system. Furthermore, addressing systemic issues like corruption and bureaucratic inefficiency is critical for ensuring that resources reach those who need them most.
Community Engagement and Education
Effective disease control requires active community participation. Raising awareness about malaria and dengue prevention, promoting personal protective measures, and encouraging early diagnosis and treatment are essential for empowering communities to protect themselves. Community health workers can play a vital role in bridging the gap between the healthcare system and the population, particularly in remote and underserved areas.
The situation in Sindh serves as a stark reminder that the fight against vector-borne diseases is inextricably linked to the broader challenges of climate change, governance, and public health infrastructure. Ignoring these interconnected factors will only lead to more frequent and severe outbreaks, with devastating consequences for vulnerable populations.
| Metric | 2024 (Estimate) | 2025 (Reported) | Projected 2030 (Based on Current Trends) |
|---|---|---|---|
| Malaria Cases (Sindh) | 180,000 | 215,000 | 350,000+ |
| Dengue Cases (Sindh) | 50,000 | 65,000 | 120,000+ |
| Public Health Spending (as % of GDP) | 1.5% | 1.6% | 1.8% (Required to meet projected needs) |
Frequently Asked Questions About the Future of Malaria in Pakistan
Q: What role will urbanization play in the spread of malaria in Pakistan?
A: Rapid, unplanned urbanization creates ideal breeding grounds for mosquitoes due to poor sanitation, inadequate drainage, and increased population density. This can lead to a significant increase in malaria transmission in urban areas, posing a new challenge for public health authorities.
Q: How can technology be leveraged to improve malaria control efforts?
A: Mobile technology can be used for real-time disease surveillance, data collection, and targeted messaging to communities. Drones can be used for aerial spraying of insecticides and mapping of mosquito breeding sites. Artificial intelligence can be used to analyze data and predict outbreaks.
Q: What is the potential impact of insecticide resistance on malaria control?
A: Insecticide resistance is a growing threat to malaria control efforts. Mosquitoes are developing resistance to commonly used insecticides, rendering them ineffective. This necessitates the development of new insecticides and the implementation of integrated vector management strategies.
What are your predictions for the future of vector-borne disease control in Pakistan and beyond? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.