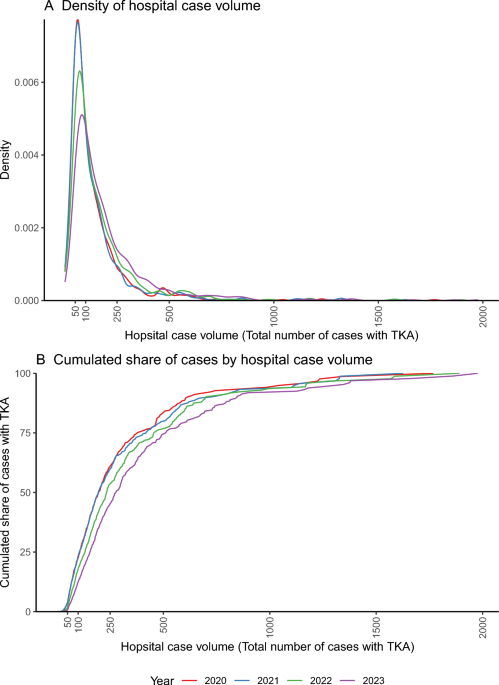
For millions of patients facing a total knee arthroplasty (TKA), the most critical question isn’t just which implant to use, but where to have the surgery. A sophisticated new analysis of German healthcare data is digging into the “volume-outcome relationship”—the medical theory that hospitals performing a higher number of procedures achieve superior patient results through a process of institutional “learning-by-doing.”
- Massive Data Scale: Researchers analyzed routine health insurance data from BARMER, covering approximately 8.7 million individuals (over 10% of the German population) from 2020 to 2023.
- Precision Metrics: The study tracks two primary failure points: the necessity of revision surgery within one year and the occurrence of surgical complications (e.g., infections, dislocations, or fractures).
- The “Experience” Variable: By using natural cubic splines, the study seeks to identify the exact “tipping point” where increased hospital volume stops providing additional benefit to patient safety.
The Deep Dive: Why Volume Matters in Orthopedics
In complex surgeries like TKA, the margin for error is slim. The “volume-outcome” hypothesis suggests that surgeons and hospital staff who perform these procedures frequently develop a refined “muscle memory” and more efficient perioperative protocols, which reduces the risk of complications. This isn’t just about the surgeon’s skill, but the entire ecosystem—from the anesthesia team to the post-operative nursing care.
This study is particularly rigorous because it doesn’t just look at raw numbers; it controls for “confounders” that typically skew medical data. For instance, the researchers isolated obesity (BMI ≥ 30) and osteoporosis, both of which are known to increase the risk of implant failure or surgical complications. By adjusting for these variables, the study can determine if a lower complication rate is due to the hospital’s expertise or simply because a specific hospital treats “healthier” patients.
Furthermore, the study distinguishes between contemporary volume (how many surgeries the hospital did this year) and historical volume (the average over the previous three years). This distinction is vital for understanding whether quality is a result of current capacity or long-term institutional expertise.
The Forward Look: Toward “Centers of Excellence”
The implications of this research extend far beyond academic curiosity; they point toward a potential restructuring of orthopedic care in Europe. If the data confirms a steep correlation between high volume and lower revision rates, we can expect several shifts in the healthcare landscape:
1. Accelerated Consolidation: We may see a move away from generalist hospitals performing a handful of TKAs toward specialized “Centers of Excellence.” This consolidation ensures that surgeons maintain the “learning-by-doing” threshold necessary for optimal outcomes.
2. Tighter Regulatory Thresholds: The German Federal Joint Committee (G-BA) already utilizes minimum volume regulations. Evidence from this study could lead to an increase in those minimums, effectively barring low-volume hospitals from performing TKA to protect patient safety.
3. Data-Driven Patient Choice: As this data becomes public, patient advocacy groups will likely demand more transparent reporting on hospital volume, transforming “number of procedures performed” into a primary KPI for patients choosing their surgical provider.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.