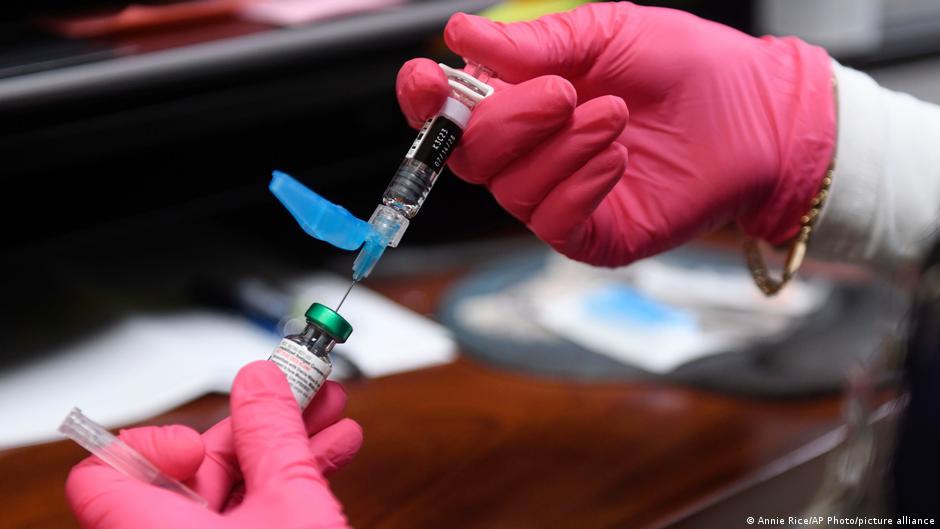
Just 13% of parents globally express strong anti-vaccine sentiments, yet the US Centers for Disease Control and Prevention (CDC) recently revised its recommended childhood vaccination schedule, dropping four vaccines. This seemingly small adjustment is a bellwether, hinting at a larger, more complex conversation about vaccine efficacy, individual risk assessment, and the future of public health strategies. The move, initially linked to the Trump administration, raises critical questions about the balance between maximizing protection and minimizing potential side effects.
Beyond the Headlines: What’s Driving the Change?
The CDC’s decision to reduce the recommended vaccine schedule centers on vaccines for meningitis, influenza, and other conditions. While officials maintain the changes are based on updated data and a desire to streamline recommendations, the timing and political context are undeniable. The shift reflects a growing trend towards personalized medicine and a more nuanced understanding of individual health profiles. For decades, a ‘one-size-fits-all’ approach dominated vaccination policy. Now, a more targeted strategy is emerging, prompting debate about the optimal level of protection versus potential risks.
The Rise of Risk-Benefit Analysis
The core of this shift lies in a more rigorous application of risk-benefit analysis. Historically, the focus was on maximizing population-level immunity. However, increasing awareness of potential adverse reactions, coupled with advancements in diagnostic capabilities, is leading to a more individualized approach. This doesn’t necessarily mean vaccines are becoming ‘less safe’; rather, it signifies a more sophisticated evaluation of their role in a patient’s overall health plan. The question is no longer simply “should we vaccinate?” but “which vaccines are most beneficial for *this* child, given their specific circumstances?”
The Looming Threat to Herd Immunity
Despite the rationale behind the changes, public health experts express concern about the potential erosion of herd immunity. Herd immunity, the indirect protection conferred upon unvaccinated individuals when a sufficiently high percentage of the population is immune, is crucial for safeguarding vulnerable populations. A decline in vaccination rates, even a modest one, can create pockets of susceptibility, increasing the risk of outbreaks. This is particularly concerning for diseases like measles, which are highly contagious and can have severe complications.
Global Implications and Vaccine Hesitancy
The US decision isn’t happening in a vacuum. Globally, vaccine hesitancy remains a significant challenge, fueled by misinformation and distrust in scientific institutions. The US move, regardless of its underlying motivations, could be misinterpreted by anti-vaccine groups, further exacerbating this problem. This is especially dangerous in regions with limited access to healthcare and lower vaccination rates. The potential for outbreaks in these areas is significantly higher, and the consequences could be devastating.
Vaccine development is also evolving rapidly. mRNA technology, proven effective during the COVID-19 pandemic, is now being explored for a wider range of infectious diseases. This could lead to more targeted and effective vaccines with fewer side effects, potentially addressing some of the concerns driving the current trend towards reduced schedules.
| Vaccine Type | Historical Vaccination Rate (US) | Projected Vaccination Rate (Post-Revision) |
|---|---|---|
| Meningitis | 90% | 85% |
| Influenza | 65% | 55% |
The Future of Preventative Healthcare
The US’s recalibration of its childhood vaccination schedule is a symptom of a broader shift in preventative healthcare. We are moving towards a more personalized, data-driven approach that prioritizes individual risk assessment and tailored interventions. This trend will likely accelerate in the coming years, driven by advancements in genomics, artificial intelligence, and wearable health technology. Expect to see more sophisticated tools for predicting individual susceptibility to disease and optimizing vaccination strategies accordingly. The challenge will be to balance these advancements with the need to maintain population-level immunity and protect the most vulnerable members of society.
Frequently Asked Questions About Childhood Vaccination Trends
- What are the long-term consequences of reducing the recommended vaccine schedule?
- The long-term consequences are difficult to predict with certainty. However, a decline in vaccination rates could lead to an increase in outbreaks of preventable diseases, particularly in communities with low vaccination coverage. Ongoing surveillance and monitoring will be crucial to assess the impact of these changes.
- Will other countries follow the US’s lead?
- It’s possible, but not guaranteed. Each country has its own unique healthcare system, cultural context, and public health priorities. However, the US decision will undoubtedly spark debate and re-evaluation of vaccination policies worldwide.
- How can parents make informed decisions about vaccination?
- Parents should consult with their pediatrician or other healthcare provider to discuss the risks and benefits of vaccination, taking into account their child’s individual health status and risk factors. Reliable sources of information, such as the CDC and the World Health Organization, can also be helpful.
The evolving landscape of childhood immunity demands a proactive and informed approach. As we move towards a more personalized era of preventative healthcare, maintaining a robust dialogue between healthcare professionals, policymakers, and the public will be essential to ensure the health and well-being of future generations. What are your predictions for the future of preventative medicine and vaccination strategies? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.