The relentless rise of dementia cases – projected to double by 2050 – is placing unprecedented strain on healthcare systems globally. But a new study published in Communications Medicine offers a significant step towards more personalized and proactive dementia care. Researchers have demonstrated that accurate, 12-month forecasts of cognitive and functional decline can be achieved using readily available clinical assessments, bypassing the need for costly and often inaccessible neuroimaging or invasive testing. This isn’t just about better predictions; it’s about shifting from reactive care to a model of precision forecasting that empowers both clinicians and patients.
- Personalized Predictions: Machine learning models accurately forecast cognitive (MMSE) and functional (BADL) decline over a 12-month period.
- Accessibility & Scalability: The models rely on routine clinical data, making them widely applicable without specialized equipment.
- Subdomain Specificity: Specific cognitive and functional areas (e.g., word recall, managing finances) are stronger predictors than overall scores, enabling targeted interventions.
The Challenge of Variability in Dementia Progression
Currently, dementia care often relies on average progression rates, failing to account for the significant variability experienced by individuals. Some patients decline rapidly, while others remain relatively stable for years. This makes it difficult for families to plan for the future and for clinicians to tailor treatment strategies effectively. The need for accessible prognostic tools has been a longstanding challenge, particularly given the logistical and financial barriers associated with neuroimaging and biomarker analysis.
How the Study Achieved Breakthroughs in Prediction
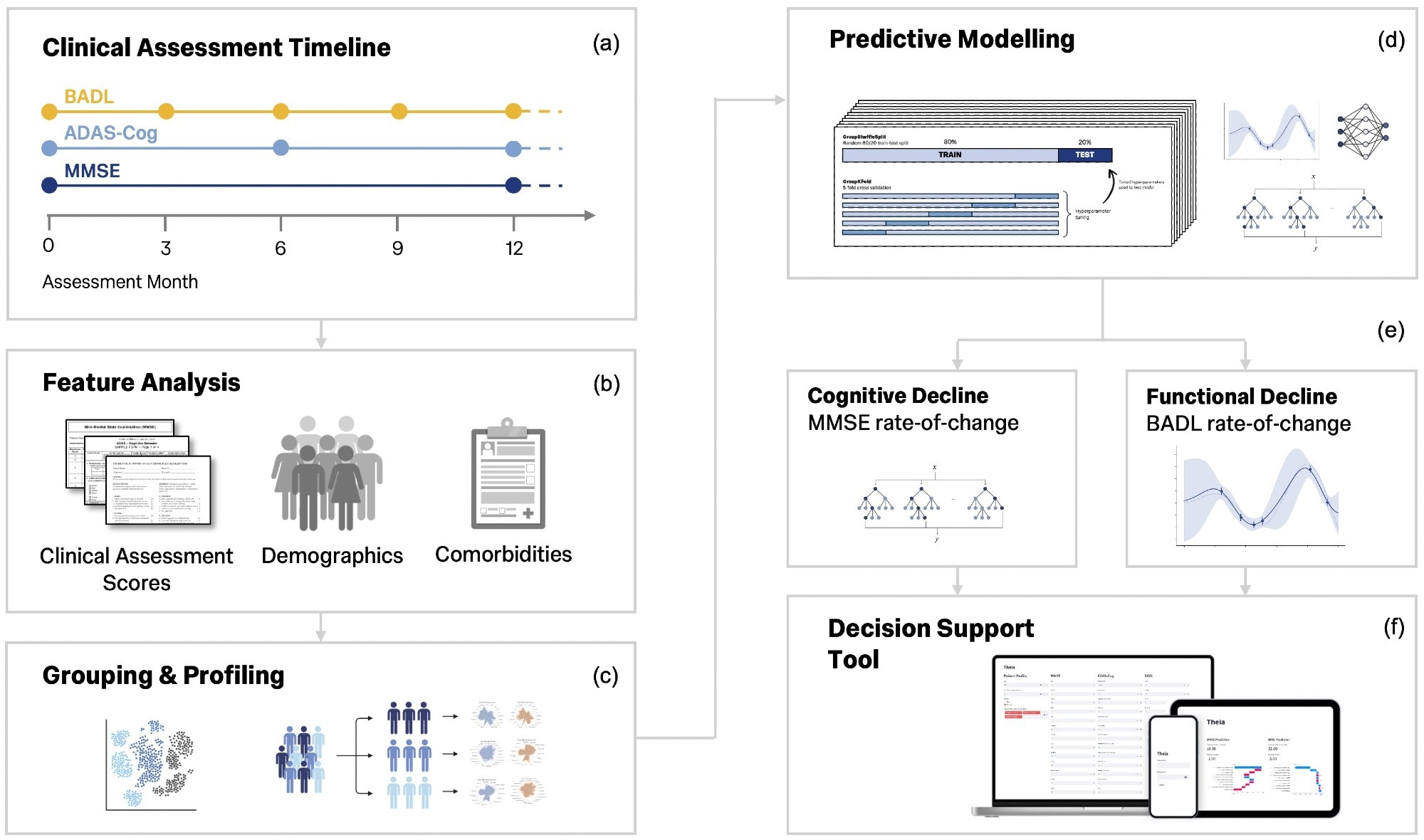
Researchers from the Minder Health Management Study in the UK leveraged data from individuals with Alzheimer’s Disease (AD) and Mild Cognitive Impairment (MCI). They developed ElasticNet regression models, analyzing clinical, demographic, and medical history data – including detailed scores from the MMSE, ADAS-Cog, and BADL assessments. A key methodological innovation was treating each 12-month period as an independent clinical trajectory, allowing for a more nuanced analysis of individual progression patterns. The models were rigorously tested, including external validation against data from the Alzheimer’s Disease Neuroimaging Initiative (ADNI), demonstrating consistent accuracy despite differences in patient populations.
Beyond Average Decline: The Power of Subdomain Analysis
The study’s findings highlight the importance of looking beyond overall cognitive and functional scores. Specific cognitive subdomains – such as ideational praxis, word recall, and visuospatial skills – were found to be highly predictive of MMSE decline. Similarly, difficulties with tasks like food preparation, financial management, and hobbies were strong indicators of functional decline. This granular level of detail allows for a more precise understanding of an individual’s strengths and weaknesses, paving the way for targeted interventions and support.
The Forward Look: Clinical Implementation and the Future of Dementia Care
The development of “Theia,” a clinician-facing decision-support tool, represents a crucial step towards translating these research findings into clinical practice. Theia not only generates predicted scores but also provides SHAP-based explanations, enhancing interpretability and building clinician trust. However, the study’s relatively modest sample size underscores the need for broader, multi-center validation in real-world clinical settings.
Looking ahead, we can anticipate several key developments. First, the integration of these predictive models into Electronic Health Records (EHRs) will become increasingly common, enabling proactive identification of patients at risk of rapid decline. Second, the use of these predictions to personalize care plans – including medication adjustments, lifestyle interventions, and support services – will become standard practice. Finally, and perhaps most importantly, these tools will empower patients and their families to have more informed conversations about their future, fostering a sense of control and reducing anxiety. This research isn’t just about predicting decline; it’s about enabling a more proactive, personalized, and ultimately, more humane approach to dementia care.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.