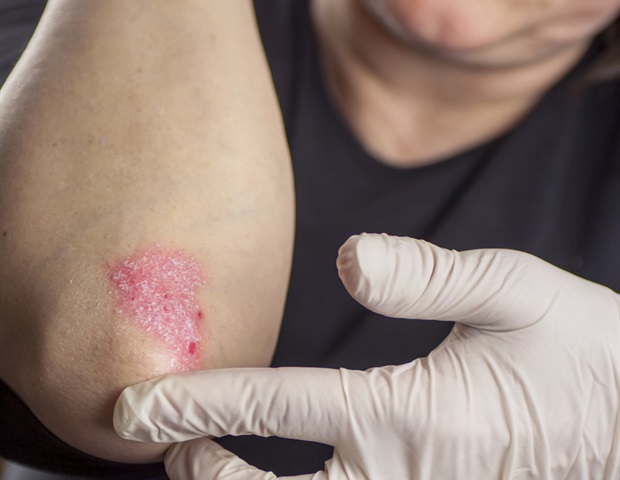
Psoriasis treatment is on the cusp of a potential paradigm shift, moving beyond solely targeting the immune system to addressing a previously unrecognized role of fat metabolism in the disease’s progression. New research from the Medical University of Vienna reveals a molecular mechanism linking fatty acid metabolism to inflammation and cell death in psoriasis, opening doors for more targeted therapies and a potential biomarker to identify patients most likely to respond.
- New Mechanism Identified: Researchers pinpointed fatty acid-binding protein 5 (FABP5) as a key driver of ferroptosis – a specific type of cell death – and inflammation in psoriasis.
- Potential Biomarker: FABP5 levels are elevated in psoriasis patients and could serve as a biomarker to predict treatment response.
- Beyond Immunomodulation: The findings suggest a combined approach – addressing both immune dysfunction *and* metabolic imbalances – may be the most effective strategy for managing psoriasis.
For decades, psoriasis has been understood primarily as an immune-mediated disease, with treatments largely focused on suppressing the overactive immune response. While biologics and other immunomodulatory therapies have significantly improved outcomes for many, a substantial portion of patients experience limited or no relief. This research suggests a critical piece of the puzzle has been missing: the interplay between skin cell metabolism and inflammation. The team’s discovery that changes in fat metabolism within skin cells contribute significantly to the development and progression of psoriasis provides a new avenue for therapeutic intervention.
The study highlights an imbalance between FABP5 and a protective enzyme, GPX4. Elevated FABP5 levels, observed in both psoriasis patients and an animal model, trigger ferroptosis, a form of iron-dependent cell death known to exacerbate inflammation. Importantly, pharmacologically blocking FABP5 and ferroptosis demonstrably reduced skin inflammation in the study, suggesting a direct causal link. This is particularly significant as ferroptosis has emerged as a key player in a range of inflammatory conditions beyond dermatology.
The Forward Look: Personalized Psoriasis Treatment & Beyond
The identification of FABP5 as a potential biomarker is arguably the most immediate impact of this research. Currently, selecting the optimal treatment for psoriasis often involves a trial-and-error approach. A biomarker like FABP5 could allow clinicians to identify patients who are likely to respond to therapies targeting fat metabolism, avoiding unnecessary exposure to less effective – and often costly – immunomodulatory drugs. We can anticipate a surge in research focused on developing assays to reliably measure FABP5 levels in skin biopsies or even blood samples.
Furthermore, the implications extend beyond psoriasis. The researchers themselves note the potential relevance to other inflammatory skin conditions like atopic dermatitis. Given the established link between psoriasis and metabolic diseases like cardiovascular disease and diabetes, this research also raises intriguing questions about shared underlying mechanisms. Future studies will likely investigate whether FABP5 plays a similar role in these systemic conditions, potentially opening up new therapeutic strategies for a broader range of diseases. The convergence of dermatology, metabolic research, and immunology is poised to accelerate, driven by this fundamental shift in understanding inflammatory disease.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.