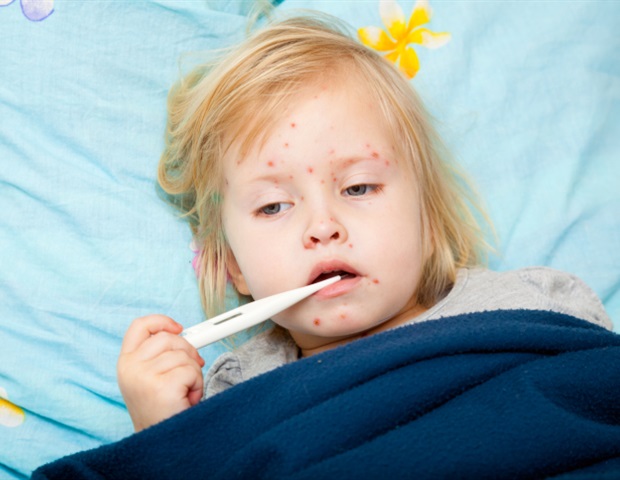
The resurgence of measles in the United States is no longer just a failure of primary care—it is becoming a crisis visible in the nation’s emergency rooms. With California reporting its highest annual measles case count in seven years as of 2026, the battle against this highly contagious disease has shifted to the “safety net” of the healthcare system: the Emergency Department (ED).
- Systemic Vulnerability: A UC Riverside study reveals critical gaps in MMR vaccination status and knowledge among ED patients, driven by structural inequities rather than simple negligence.
- The ED as a Gateway: Because underserved populations often bypass primary care, Emergency Departments are now identified as the most viable intervention points for vaccine education and screening.
- Beyond Misinformation: While vaccine hesitancy persists, barriers such as language differences, insurance status, and limited health literacy are primary drivers of under-vaccination.
The Deep Dive: Why the Safety Net is Fraying
Measles is one of the most infectious diseases known to medicine, requiring a very high threshold of community immunity (typically around 95%) to prevent outbreaks. When coverage dips even slightly, the results are immediate and volatile. The current spike in cases reflects a dangerous convergence of two trends: the proliferation of targeted misinformation and the erosion of accessible primary care.
The UC Riverside study, published in the American Journal of Emergency Medicine, underscores that the “vaccine gap” is not distributed evenly. By surveying 2,459 adult patients across ten U.S. emergency departments, researchers found that race, language, and insurance status are not just demographics—they are determinants of health literacy. When patients lack a steady primary care provider, they lose the consistent guidance necessary to navigate vaccine schedules and debunk safety myths.
This shifts the narrative from “vaccine hesitancy” (a psychological choice) to “vaccine inequity” (a structural failure). For many marginalized communities, the ED is the only point of contact with the medical establishment, making it the only place where these gaps can be identified and addressed in real-time.
The Forward Look: Redefining the Emergency Room
The findings from Dr. Robert Rodriguez and his team suggest a fundamental shift in how we utilize emergency medicine. Moving forward, we can expect to see a transition from reactive care (treating the measles infection) to proactive screening (identifying the unvaccinated patient during a visit for an unrelated issue).
What to watch for in the coming months:
- Integrated Referral Pipelines: As EDs cannot always administer the MMR vaccine on-site, look for the implementation of “warm hand-offs”—direct, coordinated referrals from ED staff to local pharmacies and clinics to ensure the patient actually receives the shot.
- Culturally Tailored Literacy Tools: To combat the systemic barriers identified in the study, healthcare systems will likely invest in multilingual, low-literacy educational materials specifically designed for the fast-paced ED environment.
- Policy Pressure on Primary Care: This data provides a strong argument for policymakers to increase funding for community health centers. If the ED is the only place we are finding unvaccinated adults, it signals a critical failure in the preventive care infrastructure that must be addressed to stop the 2026 surge.
Ultimately, the ability to curb the measles outbreak will depend on whether healthcare systems can successfully leverage the emergency department as a public health hub rather than just a trauma center.
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.