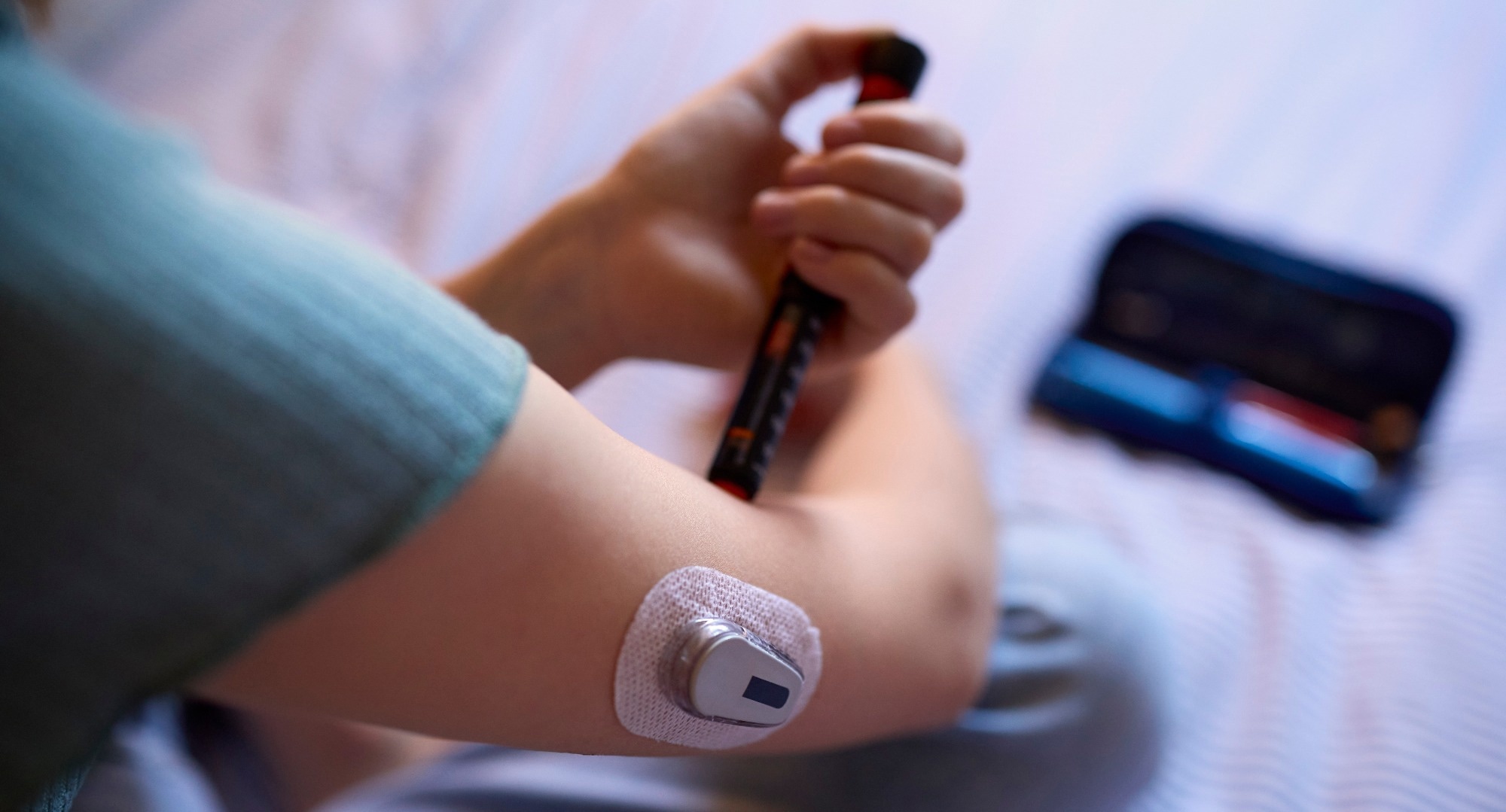
Beyond Diabetes: GLP-1s Poised to Redefine Cardiovascular & Renal Health
Nearly 1.4 million Americans are living with Type 1 diabetes, and for decades, managing the disease has primarily focused on blood sugar control. But a recent wave of research, culminating in studies published in Nature and reported by News-Medical, suggests a far more expansive role for GLP-1 receptor agonists. These drugs, initially developed for Type 2 diabetes and obesity, are now demonstrating a remarkable ability to mitigate cardiovascular and kidney risks even in individuals with Type 1 diabetes – a finding that could fundamentally reshape how we approach chronic disease management. This isn’t just about better diabetes care; it’s about a potential revolution in preventative cardiology and nephrology.
The Unexpected Benefits: A Deeper Dive into the Data
Traditionally, Type 1 diabetes has been associated with an increased risk of cardiovascular disease and kidney failure. The recent trials, however, show a statistically significant reduction in major adverse cardiovascular events (MACE) – including heart attack, stroke, and cardiovascular death – in Type 1 diabetes patients treated with GLP-1 receptor agonists. Similarly, kidney function, as measured by eGFR decline, showed marked improvement. These aren’t merely incremental improvements; the magnitude of the effect is prompting a reassessment of treatment guidelines.
Why GLP-1s Work Beyond Glucose Control
The mechanism behind these benefits extends far beyond simply lowering blood sugar. **GLP-1 receptor agonists** stimulate insulin release, but they also exert direct protective effects on the heart and kidneys. They reduce inflammation, improve endothelial function (the lining of blood vessels), and promote weight loss – all factors that contribute to cardiovascular and renal health. Furthermore, emerging research suggests GLP-1s may have neuroprotective effects, potentially offering benefits for cognitive function as well.
Navigating the Regulatory Landscape & Future Guidance
The FDA is currently evaluating the data and preparing guidance on the appropriate use of GLP-1 drugs in Type 1 diabetes, as highlighted by Medscape and National Today. As The Clinical Trial Vanguard points out, the agency isn’t facing a safety issue with GLP-1s, but rather a need for robust evidence to support expanded indications. This cautious approach is understandable, but it also underscores the importance of continued research and real-world data collection.
The Rise of Combination Therapies & Personalized Medicine
Looking ahead, the future of GLP-1 therapy likely lies in combination approaches. We can anticipate trials investigating the synergistic effects of GLP-1 agonists with other medications, such as SGLT2 inhibitors, to maximize cardiovascular and renal protection. Moreover, the field is moving towards personalized medicine, identifying biomarkers that predict which patients will respond most favorably to GLP-1 treatment. Genetic predispositions, gut microbiome composition, and individual metabolic profiles will all play a role in tailoring therapy.
Beyond Type 1: Expanding the Scope of GLP-1 Applications
The success of GLP-1s in Type 1 diabetes is fueling exploration of their potential in other conditions. Research is underway to assess their efficacy in preventing heart failure in patients with pre-diabetes, slowing the progression of chronic kidney disease in individuals without diabetes, and even mitigating the long-term cardiovascular consequences of COVID-19. The versatility of these drugs suggests they could become a cornerstone of preventative medicine across a broad spectrum of diseases.
Here’s a quick look at projected growth:
| Market Segment | 2024 (USD Billion) | 2030 (USD Billion) | CAGR |
|---|---|---|---|
| Type 2 Diabetes | 15.2 | 31.8 | 10.1% |
| Obesity | 8.5 | 18.7 | 12.5% |
| Cardiovascular Disease (Emerging) | 0.5 | 4.2 | 30.3% |
Frequently Asked Questions About GLP-1 Therapies
What are the potential side effects of GLP-1 receptor agonists?
Common side effects include nausea, vomiting, and diarrhea, which are usually mild and transient. More serious, though rare, side effects include pancreatitis and gallbladder problems. Patients should discuss potential risks with their healthcare provider.
Will GLP-1s become a standard of care for all Type 1 diabetes patients?
Not necessarily. The current guidance focuses on patients with established cardiovascular or kidney disease. Further research is needed to determine whether GLP-1s should be used preventatively in all Type 1 diabetes patients.
How accessible will these drugs be, given their increasing demand?
Accessibility is a significant concern. The high cost of GLP-1s and potential supply chain issues could limit access for some patients. Efforts to increase affordability and manufacturing capacity are crucial.
The story of GLP-1 receptor agonists is far from over. What began as a treatment for Type 2 diabetes is rapidly evolving into a powerful tool for combating a wider range of chronic diseases. As research continues to unravel the full potential of these drugs, we can expect to see even more innovative applications emerge, ultimately transforming the landscape of preventative and therapeutic medicine.
What are your predictions for the future of GLP-1 therapies? Share your insights in the comments below!
Discover more from Archyworldys
Subscribe to get the latest posts sent to your email.